Center for Cerebrovascular Research
The Center for Cerebrovascular Research (CCR) is a core group of faculty and staff pursuing integrative and interdisciplinary studies of cerebrovascular disease, utilizing the tools of cell biology, animal models, human genetics, epidemiology and treatment outcomes research. Our main area of focus is vascular malformations of the brain, which are an important cause of hemorrhagic stroke, and include arteriovenous malformations (AVM), intracranial aneurysms and cerebral cavernous malformations (CCM).
CCR News/Events
COVID-19: During the current phase of the COVID-19 epidemic, the CCR is continuing research operations in accordance with US, California and UCSF shelter-in-place policies and advisories. On-campus research activities have been minimized and most research is being conducted remotely, where possible. For our human studies, we currently continue those activities, which can be performed via phone call, email or video conference.
Please continue to contact us with any questions about our studies or research participation at [email protected]
General information about COVID-19 is available on the UCSF website: https://coronavirus.ucsf.edu/patients
Additional information regarding the possible impact of COVID-19 on specific diseases is available through Patient Advocacy Group websites:
- for CCM, at Alliance To Cure Cavernous Malformation: Alliance To Cure Cavernous Malformation/covid
- for HHT, at CureHHT: https://curehht.org/covid19/
- for SWS, at the Sturge Weber Foundation: SWS/for-patients/five-step-preparation-for-covid
- for AVM, at The Aneurysm and AVM Foundation: https://taafonline.org/
- Research survey for rare disease patients and their families about impacts of COVID-19. How is the novel coronavirus pandemic impacting people with rare diseases and their families? Complete the 20-minute research survey from home or learn more: COVID-19 Research Survey
____________________________________________________________________________________________________________________________________________________________________________________________________________

https://ucsf.zoom.us/j/95624427396?pwd=Z3p2d3loQUt3ZWFvOWV4Yy83ZE9wUT09
____________________________________________________________________________________________________________________________________________________________________________________________________________
Announcement: The 18h TAAF Annual Aneurysm and AVM Walk will be held at Crissy Field in San Francisco on Sunday, September 24, 2023!
2023 TAAF Annual Aneurysm and AVM Walk

____________________________________________________________________________________________________________________________________________________________________________________________________________
Annoucement: The 12th Annual William L. Young/Allison Raaen Lectureship is on April 20, 2023.

____________________________________________________________________________________________________________________________________________________________________________________________________________

Brain Vascular Malformation Consortium (BVMC) Spotlight features were published on the RDCRN blog #RareDiseasesSpotlight
____________________________________________________________________________________________________________________________________________________________________________________________________________
On November 9 & 10 in San Francisco will be held The Rare Disease Film Festival, over 50 short films on rare disease, with Dr.Helen Kim, Professor, CCR Director and Dr. Navneet Matharu Assistant Researcher in the Department of Bioengineering at UCSF as speakers. Disorder - The Rare Disease Film Festival
____________________________________________________________________________________________________________________________________________________________________________________________________________
A group picture of the BVMC in Person Executive Commitee Meeting which was held in Puerto Rico on June 2019.

____________________________________________________________________________________________________________________________________________________________________________________________________________
The challenge of HHT diagnostic.
Read Zina Martinez's nosebleeds story on Washington Post article: It was just a nosebleed caused by bone-dry air — or was it?
____________________________________________________________________________________________________________________________________________________________________________________________________________
On May 5th CCR members and friends joined the 14th TAAF Annual Aneurysm and AVM Walk at Crissy Field in San Francisco. 2019 TAAF Annual Aneurysm and AVM Walk

___________________________________________________________________________________________________________________________________________________________________________________________________________
Helen Kim, Li Ma from Tiantan Beijing Hospital and Hua Su met at the 2019 Stroke Conference in Honolulu

____________________________________________________________________________________________________________________________________________________________________________________________________________

On August 9, Dr. Awad was the guest speaker at the 9th Annual William L. Young/Allison Raaen Lectureship

____________________________________________________________________________________________________________________________________________________________________________________________________________
On May 14-15 the CCR hosted the 2018 BVMC in Person Executive Committee Meeting in San Francisco

____________________________________________________________________________________________________________________________________________________________________________________________________________
The CCR clinical research group (left to right: Kimberly Yan, Diana Guo, Keva DeKay, and Helen Kim) attended The International Stroke Conference 2018 in Los Angeles

___________________________________________________________________________________________________________________________________________________________________________________________________________
Associate Professor Helen Kim Author on Breakthrough Study Published in Nature
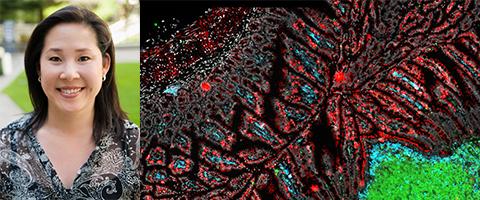
Associate Professor and Center for Cerebrovascular Research investigator, Helen Kim, PhD, MPH, and her colleagues, have published a breakthrough study in Nature, establishing the connection between brain vascular malformations and our microbiome, or gut bacteria. The article, “Endothelial TLR4 and the Microbiome Drive Cerebral Cavernous Malformations,” has recently been featured in major news outlets such as the New York Times. Specifically, Dr. Kim and her colleagues played a major role in demonstrating the relevance of the animal findings for this study, using the human cerebral cavernous malformation (CCM) cohort from their U54-funded BVMC CCM study. The human subjects provided DNA samples that were genotyped at the UCSF Genomics Core Facility.

We need and welcome your participation in our research studies!
For more information about our studies and how you or someone you know can participate, please contact one of our Research Coordinators directly:
- Eliel Rios Leon at (415) 476-2680 - [email protected]
- Nhu Kim Huynh at (415) 502-6192 - [email protected]
- email us at [email protected]
COVID-19: During the current phase of the COVID-19 epidemic, the CCR is continuing research operations in accordance with US, California and UCSF shelter-in-place policies and advisories. On-campus research activities have been minimized and most research is being conducted remotely, where possible. For our human studies, we currently continue those activities, which can be performed via phone call, email or video conference.
Please continue to contact us with any questions about our studies or research participation.
General information about COVID-19 is available on the UCSF website: https://coronavirus.ucsf.edu/patients
Additional information regarding the possible impact of COVID-19 on specific diseases is available through Patient Advocacy Group websites:
- for CCM, at Alliance To Cure Cavernous Malformation: Alliance To Cure Cavernous Malformation/covid
- for HHT, at CureHHT: https://curehht.org/covid19/
- for SWS, at the Sturge Weber Foundation: SWS/five-step-preparation-for-covid-19
- for AVM, at The Aneurysm and AVM Foundation: https://taafonline.org/
- Research survey for rare disease patients and their families about impacts of COVID-19. How is the novel coronavirus pandemic impacting people with rare diseases and their families? Complete the 20-minute research survey from home or learn more: COVID-19 Research Survey
_______________________________________________________________________________________________________________
The CCR is actively recruiting participants for the following studies:
BRAIN ARTERIOVENOUS MALFORMATION (bAVM) STUDIES
Brain arteriovenous malformations (bAVM) are dynamic vascular lesions that can grow, and in some cases grow back (recur) after treatment. The factors that cause these vessels to grow, recur, or rupture are not well understood, especially in the pediatric population.
Predictors of Growth, Recurrence, and High-Risk Features in Pediatric Brain Arteriovenous Malformation
The purpose of this study is to identify imaging characteristics and blood markers that may explain how these blood vessels grow or change over time. By understanding when AVM features develop, doctors will be better able to monitor and develop new drug treatments for bAVM, which do not currently exist.
Eligibility Criteria: Age ≤ 18 years at bAVM diagnosis.
Eligibility for imaging sub-group:
- Age ≥ 3 years and <19 years at bAVM diagnosis
- Ruptured bAVM
- Screening/enrollment date before or within 6-months of bAVM treatment date
- Parent/guardian consent & patient assent obtainable (when appropriate)
_______________________________________________________________________________________________________________
Multicenter Arteriovenous Malformation Research Study (MARS)
Brain arteriovenous malformations (bAVMs) are a leading cause of intracranial hemorrhage (bleeding in the brain) in younger people. In collaboration with study centers across the world, we are recruiting patients with unruptured bAVMs to better understand these malformations. The MARS consortium aims to compare the untreated and treated disease course for unruptured bAVMs and to provide guidance for physicians to provide better treatment plans for their patients.
Eligibility criteria: Patients initially diagnosed with an unruptured bAVM.
_______________________________________________________________________________________________________________
CEREBRAL CAVERNOUS MALFORMATION (CCM) STUDIES
BVMC 6201: Modifiers of Disease Severity and Progression in Cerebral Cavernous Malformation
Individuals with Cerebral Cavernous Malformations (CCMs) have clusters of abnormally enlarged blood vessels in the brain and spinal cord. These abnormal clusters may be sporadic or familial (inherited) and can potentially cause problems such as bleeding in the brain, stroke, seizures, disabilities, or death. This project is funded through collaboration between NCATS and NINDS with the purpose of understanding the natural history, epidemiology, diagnosis, and treatment of people living with familial CCM. We will collect clinical, genetic, imaging, treatment, and outcome data in participants, and follow the cohort over time to understand the natural history of this disease.
Eligibility criteria: Patients must fulfill either requirement listed below:
- Confirmed genetic mutation in any CCM gene
- Without confirmed mutation, diagnosed with familial CCM disease, meet at least 2 of 3 following criteria:
_______________________________________________________________________________________________________________
Biomarkers of Cerebral Cavernous Angioma with Symptomatic Hemorrhage (CASH)
Cerebral cavernous angiomas (CA) can bleed and cause symptomatic hemorrhage (SH). CASH lesions are most likely to re-bleed again, causing clinical problems. In this study, we will collect blood from you to see if we can find markers in the blood that would tell us if you have had a brain bleed or if you will have one in the coming year. This project is done in collaboration with the University of Chicago and the Mayo Clinic – Rochester. We are recruiting adult CA patients who meet the eligibility criteria below.
Eligibility criteria: Age ≥ 18 years and has diagnosis of cavernous angioma
Exclusion criteria:
- Prior stereotactic radiosurgery or any brain irradiation
- Prior excision of Solitary Cavernous Angioma lesion
- Spinal Cavernous Angioma without brain lesion
- Other brain pathology non-related to CA (demyelinating disease, brain tumor)
- Active malignancy or cancer treatment in the past year
- Seizure or stroke unrelated to CA in the prior year
- Current pregnancy or within 6 months postpartum
- Reluctance to undergo venipuncture or donate blood specimen
- Reluctance to be called for clinical follow-up for up to 1 year
______________________________________________________________________________________________________________
HEREDITARY HEMORRHAGIC TELANGIECTASIA (HHT) STUDIES
Hereditary Hemorrhagic Telangiectasia (HHT) is an inherited condition that causes abnormal blood vessels and nose and gastrointestinal bleeding. In HHT, small abnormal blood vessels called telangiectasias occur in the skin and mucous membranes, while larger vessel abnormalities, called arteriovenous malformations occur in various organs, including the brain, where they can cause bleeding and stroke.
BVMC 6203: Cerebral Hemorrhage Risk in Hereditary Hemorrhagic Telangiectasia
- Patient Spotlight: https://www.rarediseasesnetwork.org/news/2021-10-19-BVMC-Patient-Spotlight
- Video: https://vimeo.com/631020190
This project is funded through collaboration between NCATS and NINDS, with the purpose of understanding the natural history, epidemiology, diagnosis, and treatment of people living with HHT, with and without brain arteriovenous malformations (bAVMs). We will collect clinical, genetic, imaging, treatment, and outcome data in participants, and follow the cohort over time to understand the natural history of this disease.
Eligibility criteria: Patients must fulfill either requirement listed below:
- Confirmed genetic mutations in the genes which cause HHT
- Without confirmed mutation, definite clinical HHT diagnosis, defined as fulfilling at least 3 of 4 Curacao criteria:
_______________________________________________________________________________________________________________
Investigating Disparities and Barriers in Access to Research and Care for Patients with Hereditary Hemorrhagic Telangiectasia (HHT)
The purpose of this study is to identify barriers to referrals, care, and research for patients with Hereditary Hemorrhagic Telangiectasa (HHT). Understanding barriers will help us work to lessen disparities and improve care. Eligible participants will be asked to participate in a focus group session via Zoom or in-person or complete a survey. The National Institutes of Health (NIH) is funding this research.
Eligibility criteria for Focus Group:
- Adult (18 years and older)
- Resident of Canada or the USA
- Be familiar with HHT
Eligibility criteria for Survey Group:
- Adult (18 years and older)
- Resident of Canada or the USA
- Definite HHT diagnosis by clinical criteria or genetic testing
_______________________________________________________________________________________________________________
STURGE-WEBER SYNDROME (SWS) STUDIES
Sturge-Weber Syndrome (SWS) is a vascular disorder of capillary angiomas resulting in port wine stain angiomas affecting the skin, angiomas and glaucoma of the eye, and leptomeningeal angiomas surrounding the brain. Serious complications can arise from the effects of the vascular malformation and the surrounding brain tissue.
BVMC 6211: Longitudinal Studies to Identify Biomarkers and Therapeutic Strategies for Sturge-Weber Syndrome
This project is funded through a collaboration between NCATS and NINDS with the purpose of understanding factors associated with clinical symptoms, which patients are at-risk for these symptoms, and which treatment strategies may be preventative.
Eligibility criteria: Patients diagnosed with Sturge-Weber Syndrome
_______________________________________________________________________________________________________________
STROKE
An ischemic stroke is any damage to the brain caused by lack of blood flow to brain blood vessels or in major arteries leading to the brain. A hemorrhagic stroke is damage to the brain due to bleeding into the brain. In the United States, someone suffers a stroke every 40 seconds. Brain vascular malformations and aneurysms are just a few of the many causes of strokes. To learn more:
What Is a Stroke?
About Stroke
What You Should Know About Cerebral Aneurysms
Cerebrovascular And Stroke Program for children
Predictors of Growth, Recurrence, and High-risk Features in Pediatric Brain Arteriovenous Malformation
ARTERIOVENOUS MALFORMATIONS (AVMs)
Normal Blood Vessels Abnormal Connection of Blood Vessels

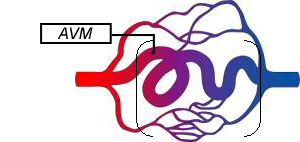
Arteriovenous Malformations (AVMs) are tangles of blood vessels in the brain or on its surface bypasses normal brain tissue and directly diverts blood from the arteries to the veins. ARUBA (A Randomized trial of Unruptured Brain Arteriovenous malformations) was a stroke prevention trial whose findings where groundbreaking in the management and care of AVM. To learn more:
What Is an Arteriovenous Malformation (AVM)? Arteriovenous Malformations and Other Vascular Lesions of the Central Nervous System Fact Sheet
AVM at UCSF Neurovascular Disease and Stroke Center
The Aneurysm and AVM Foundation
Hereditary Hemorrhagic Telangiectasia (HHT)
HHT, also known as Osler-Weber-Rendu syndrome, is a rare autosomal dominant disorder that affects blood vessels throughout the body and results in a tendency for bleeding. To learn more about receiving care at UCSF and for patient advocacy groups (CureHHT):
UCSF HHT Center of Excellence
CureHHT
Cerebral Cavernous Malformations (CCMs)
CCMs, also known as cavernomas and cavernous angiomas, are abnormal clusters of dilated blood vessels, which can be either sporadic or familial, inherited cases. To learn more about these malformations, receiving care at UCSF and for patient advocacy groups (Alliance To Cure):
UCSF CCM Center for Excellence
What is a Cerebral Cavernous Malformation (CCM)?
Alliance To Cure Cavernous Malformation
From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair
What is a brain AVM?
Normally, arteries carry blood containing oxygen from the heart to the brain, and veins carry blood with less oxygen away from the brain and back to the heart. When an arteriovenous malformation (AVM) occurs, a tangle of blood vessels in the brain or on its surface bypasses normal brain tissue and directly diverts blood from the arteries to the veins.
Normal Blood Vessels Abnormal Connection of Blood Vessels


How common are brain AVMs?
Brain AVMs occur in less than one percent of the general population. It is estimated that about one in 200-500 people may have an AVM. AVMs are more common in males than females.
Why do brain AVMs occur?
We do not know why AVMs occur. Brain AVMs are usually congenital, meaning someone is born with one. However, they usually are not hereditary. People probably do not inherit an AVM from their parents, and they probably will not pass an AVM on to their children.
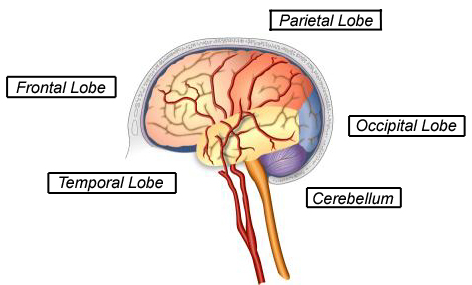
Where do brain AVMs occur?
Brain AVMs can occur anywhere within the brain or on the covering of the brain. This includes the four major lobes of the front part of the brain (frontal, parietal, temporal, occipital), the back part of the brain (cerebellum), the brainstem, or the ventricles (deep spaces within the brain that produce the cerebrospinal fluid).
Do brain AVMs change or grow?
Most AVMs do not grow or significantly change although the vessels involved may dilate. There are some reported cases of AVMs shrinking or enlarging, but this may be due to clots in parts of an AVM causing it to shrink, or to redirecting adjacent blood vessels toward an AVM.
What are the symptoms of a brain AVM?
Symptoms may vary with location.
- More than 50 percent of patients with an AVM complain of headaches.
- 45-60 percent of patients with an AVM have seizures.
- Patients may have localized pain in the head due to increased blood flow around an AVM
- Difficulty with movement, speech and vision may occur.
What causes brain AVMs to bleed?
A brain AVM contains abnormal and, therefore, "weakened" blood vessels that direct blood away from normal brain tissue. These abnormal and weak blood vessels dilate over time and may eventually burst from the high pressure of blood flow from the arteries causing bleeding into the brain.
What are the chances of a brain AVM bleeding?
There is a 1-3 percent chance per year of a brain AVM bleeding. Over a 15-year period, there is a 25 percent total chance of an AVM bleeding into the brain, causing brain damage and stroke.
Does one bleed increase the chance of a second bleed?
With one bleed, the chance of a second bleed is 25 percent over the next four years, or 6 percent per year. If there are two or more bleeds, the chance of more bleeds is even higher, increasing to 25 percent per year. Individuals with an AVM are at a slightly higher risk of bleeding between the ages of 11 and 35.
What can happen if a brain AVM causes a bleed?
There is a 10-15 percent risk of death related to each bleed and a 20-30 percent chance of permanent brain damage. Each time blood leaks into the brain, normal brain tissue is damaged. This results in loss of normal function, which may be temporary or permanent. Some possible symptoms include arm or leg weakness/paralysis, or difficulty with speech, vision or memory. The amount of brain damage depends upon how much blood has leaked from the AVM.
What functions does an AVM affect?
If an AVM bleeds, it can affect one or more normal body functions, depending on the location and extent of the brain injury. Different locations in the brain control different functions:
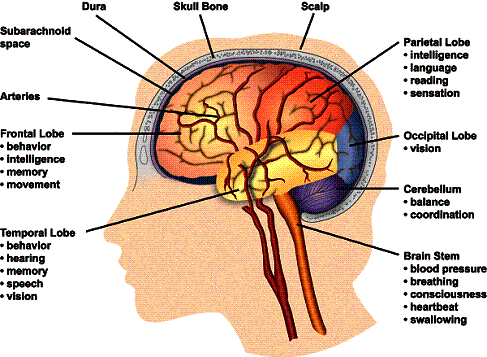
- Frontal lobe controls personality.
- Parietal lobe controls movement of the arms and legs.
- Temporal lobe controls speech, memory and understanding.
- Occipital lobe controls vision.
- The cerebellum controls walking and coordination.
- Ventricles control the secretion of cerebrospinal fluid.
- The brainstem controls the pathways from all of the above functions to the rest of the body.
Are there different types of brain AVMs?
Although all blood vessel malformations involving the brain and its surrounding structures are commonly referred to as AVMs, there are actually several types:
- True Arteriovenous malformation (AVM). This is the most common brain vascular malformation and consists of a tangle of abnormal vessels connecting arteries and veins with no normal intervening brain tissue.
- Occult or cryptic AVM or cavernous malformations. This is a vascular malformation in the brain that does not actively divert large amounts of blood. It may bleed and often produce seizures.
- Venous malformation. This is an abnormality only of the veins. The veins are either enlarged or appear in abnormal locations within the brain.
- Hemangioma. These are abnormal blood vessel structures usually found at the surface of the brain and on the skin or facial structures. These represent large and abnormal pockets of blood within normal tissue planes of the body.
- Dural fistula. The covering of the brain is called the "dura mater." When there is an abnormal connection between blood vessels that involve only this covering, it is called a dural fistula. Dural fistulas can occur in any part of the brain covering.
There are three kinds of dural fistulas.
- Dural carotid cavernous sinus fistula. These occur behind the eye and usually cause symptoms due to diverting too much blood toward the eye. Patients have eye swelling, decreased vision, redness and congestion of the eye. They often can hear a "swishing" noise.
- Transverse-Sigmoid sinus dural fistula. These occur behind the ear. Patients usually complain of hearing a continuous noise that occurs with each heartbeat (bruit), local pain behind the ear, headaches and neck pain.
- Sagittal sinus and scalp dural fistula. These occur toward the top of the head. Patients complain of noise (bruit), headaches, and pain near the top of the head; they may have prominent blood vessels on the scalp and above the ear.
What is the best treatment for a dural fistula?
The best treatment is usually endovascular surgical blocking of the abnormal connections that have caused the fistula. This involves guiding small tubes (catheters) inside the blood vessel and blocking off the abnormal connections with X-ray guidance. Depending upon the location and size, many of these can be treated and cured by these endovascular, less invasive techniques.
How are AVMs diagnosed?
Most AVMs are detected on either a computed tomography (CT) brain scan or with a magnetic resonance imaging (MRI) brain scan. These tests are very good at detecting brain AVMs. They also provide information about the location and size of the AVM and whether it may have bled.
A doctor may also perform a cerebral angiogram. This test involves inserting a catheter (small tube) through an artery in the leg and guiding it into each of the vessels in the neck going to the brain, injecting contrast (dye) and taking pictures of all the blood vessels in the brain. For any type of treatment involving an AVM, an angiogram may be needed to better identify the type of AVM.
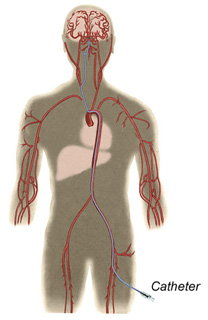
What factors influence whether an AVM should be treated?
In general, an AVM may be considered for treatment if it has bled, if it is in an area of the brain that can be easily treated and if it is not too large.
What is the best treatment for an AVM?
This depends upon what type it is, the symptoms it may be causing, and its location and size.
What different types of treatment are available?
- Medical Therapy. If there are no symptoms or almost none, or if an AVM is in an area of the brain that cannot be easily treated, conservative medical management may be indicated. If possible, a person with an AVM should avoid any activities that may excessively elevate blood pressure, such as heavy lifting or straining, and they should avoid blood thinners like warfarin. A person with an AVM should have regular checkups with a neurologist.
- Surgery. If an AVM has bled and/or is in an area that can be easily operated upon, then surgical removal may be recommended. The patient is put to sleep with anesthesia, a portion of the skull is removed, and the AVM is surgically removed. When the AVM is completely taken out, the possibility of any further bleeding should be eliminated.
- Stereotactic radiosurgery. An AVM that is not too large, but is in an area that is difficult to reach by regular surgery, may be treated by performing stereotactic radiosurgery. In this procedure, a cerebral angiogram is done to localize the AVM. Focused-beam high energy sources are then concentrated on the brain AVM to produce direct damage to the vessels that will cause a scar and allow the AVM to "clot off."
- Interventional neuroradiology/endovascular neurosurgery. It may be possible to treat part or all of the AVM by placing a catheter inside the blood vessels that supply the AVM and blocking off the abnormal blood vessels with a variety of different materials. These include liquid tissue adhesives (glues), micro-coils, particles and other materials used to stop blood flowing to the AVM.
The best course of treatment depends upon what type of symptoms the patient is having, what type of AVM is present, and the AVM's size and location.
What doctors specialize in treating brain AVMs?
- Vascular neurosurgeons specialize in surgically removing brain AVMs.
- Radiation therapists/neurosurgeons specialize in the stereotactic radiosurgery treatment of brain AVMs.
- Interventional neuroradiologists/endovascular neurosurgeons specialize in the endovascular therapy of brain AVMs.
- Stroke neurologists specialize in the medical management of brain AVMs.
- Neuroradiologists specialize in the diagnosis and imaging of the head, neck, brain, and spinal cord. They perform and interpret the CT, MRI, and cerebral angiograms necessary for evaluation, management, and treatment.
Each of these specialists has had advanced training and is highly skilled at treating complex brain vascular malformations.
About Strokes and Cerebrovascular Diseases
Stroke and cerebrovascular diseases are the third-leading cause of death and a leading cause of major disability in the United States. More than 700,000 new and recurrent strokes occur each year, resulting in over 167,000 deaths and more than 250,000 permanent disabilities. About 4.7 million stroke survivors are alive today.
Ischemic strokes occur when the normal blood flow to the brain is blocked. They account for the majority of strokes. Treatment is available but must be started as soon as possible to give the best chance for recovery.
Hemorrhagic strokes are caused by bleeding into the brain, resulting in either death or major disability. Many of these strokes occur when a cerebral aneurysm or brain AVM ruptures.
For more information, contact the American Stroke Association, a division of the American Heart Association, at 1-888-4-STROKE (1-888-478-7653) or visit StrokeAssociation.org.
Funded through an educational grant provided by Boston Scientific


What Is a Stroke?
From the Cerebrovascular Imaging and Interventions Committee of the American Heart Association Cardiovascular Radiology Council
Randall T. Higashida, M.D., Chair
An ischemic stroke is ANY damage to the brain caused by lack of blood flow in the brain blood vessels or in major arteries leading to the brain. This usually results in temporary or permanent loss of one or more normal functions of the body. A hemorrhagic stroke is due to bleeding into the brain causing damage.
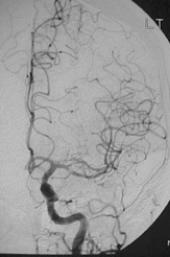
This angiogram shows normal blood vessels to the brain
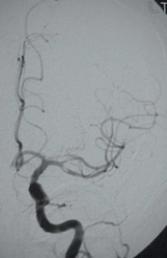
In this angiogram, many normal blood vessels are not visible due to a blood clot blocking blood flow to the brain.
How often do strokes occur?
Strokes are very common. In the United States, someone suffers a stroke every 45 seconds. About 700,000 new and recurrent strokes occur each year. Strokes affect one in five people during their lifetime.
After heart disease and all forms of cancer, stroke is the third-leading cause of death in the United States, Canada, Europe and Japan.
What do strokes cost?
Estimates are that strokes cost about $50 billion a year in the United States. Over $30 billion is spent on hospitalization, medical equipment and rehabilitation. (Strokes are a leading cause of adult disability, often requiring in-patient rehabilitation.) Lost productivity from stroke survivors being unable to return to their jobs accounts for nearly $20 billion.
What factors increase the risk of stroke?
There are two types of risk factors - those you can't control and those you can.
Factors you can't control:
- Age - The older you are the higher your risk.
- Gender - Males are at higher risk than females.
- Race - Blacks, Hispanics/Latinos and Asians have higher risks than whites.
- Family history of stroke and heart disease.
- A prior stroke or TIA (transient ischemic attack).
Factors you can control:
- Diet - Eat a diet low in saturated fat, cholesterol and salt.
- Obesity - The more overweight, the higher the risk.
- High Blood Pressure - Should be controlled and maintained at less than 140/90 mm Hg.
- Heart Disease - Atrial fibrillation (a rapid, irregular heartbeat) should be treated.
- Carotid Artery Disease - Can be treated by surgery, stenting, or medical therapy
- Smoking - Should be avoided.
- High Cholesterol - Should be lowered.
- Excess Alcohol Intake - Should be avoided.
- Diabetes - Increases the risk for stroke and should be controlled through diet, oral hypoglycemics (drugs taken by mouth that lower blood sugar) or insulin.
What will happen if I have a stroke?
One of three things can happen:
- About 28 percent of strokes are fatal.
- Fifty to 70 percent of survivors will have a mild disability or will improve.
- Fifteen to 30 percent who survive will be severely disabled, even years after a stroke.
- Institutional care is required by 20 percent three months post-stroke.
More than 4.6 million people in the United States have some disability from a stroke. Rehabilitation may benefit stroke survivors, but the underlying cause for the stroke still needs to be treated.
There are two major types of stroke. The first is caused by blocked blood flow and oxygen to the brain. This is called an "ischemic" stroke. They account for nearly 80 percent of all strokes. The second type is caused by bleeding into or around the brain. This is called a "hemorrhagic" stroke. Hemorrhagic strokes account for about 20 percent of strokes.
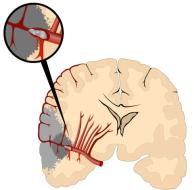
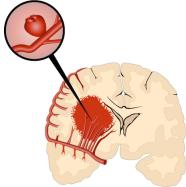
Ischemic Stroke Hemorrhagic Stroke
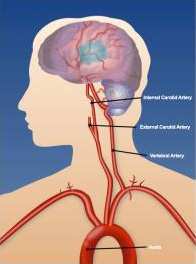
An ischemic stroke is caused when blood flow is blocked either by a blood clot that forms in the heart or on a hardened fatty buildup (atherosclerotic plaque) in one of the larger blood vessels going to the brain. These vessels are the carotid artery in the front of the brain or the vertebral and basilar arteries in the back of the brain.
What causes an ischemic stroke?
A blood clot that travels into the brain is called a "cerebral embolus." A clot that builds up in the brain and ultimately blocks this blood vessel is called a "cerebral thrombosis."
What causes a hemorrhagic stroke?
A common cause is a ruptured "cerebral aneurysm." This is a weakened section of a brain artery that has ballooned out and burst. Other causes are:
- A brain vascular malformation (commonly called an "arteriovenous malformation or AVM)
- High blood pressure that ruptures a tiny artery
- Drugs that cause acute blood pressure changes
- Direct brain injury
What is a transient ischemic attack (TIA)?
A TIA occurs when a person briefly experiences stroke symptoms that last from several seconds to minutes, and then go away. There's usually no permanent brain damage. However, a person experiencing a TIA should be examined immediately, because a TIA is often a sign that a major stroke will occur. Never ignore the warning signs of a stroke. A TIA is a very important warning sign!
What are the warning signs of a stroke?
The most common warning signs of a stroke are:
- Sudden numbness or weakness of the face, arm, or leg, especially on one side of the body.
- Sudden confusion, trouble speaking or understanding.
- Sudden trouble seeing in one or both eyes.
- Sudden trouble walking, dizziness, loss of balance or coordination.
- Sudden, severe headache with no known cause.
What should a person do if they suspect they are having a stroke?
The immediate response to experiencing or witnessing any of the symptoms outlined above is to call 9-1-1. The patient or their guardian should ask to be taken to the closest hospital or emergency room that specializes in stroke treatment. Staff at some hospitals may not be adequately prepared to recognize and treat stroke. A person having a stroke needs to be evaluated quickly and treated before it's too late!
What happens if a person ignores symptoms or delays treatment?
The longer the delay for evaluation and treatment, the more likely the damage will be irreversible and permanent and the higher the chances of dying or experiencing severe disability from an acute stroke. Intravenous tPA (tissue Plasminogen Activator) is an FDA approved drug that improves the likelihood of partial or complete recovery for certain strokes. This drug can only be given to patients who qualify for this therapy and must be administered by properly trained personnel within 3 hours of the onset of certain strokes.
What if a patient arrives after three hours from the start of a stroke?
With a stroke, time is brain. The longer a person waits, the more likely the brain damage will be irreversible. Intravenous tPA (tissue Plasminogen Activator), the only FDA-approved drug treatment for acute, ischemic stroke, has not been shown to be effective after three hours. However, depending upon the severity of symptoms, a stroke patient may be eligible for other types of treatments. Evidence shows that placing a small tube (catheter) directly into the blood clot within the brain and giving a clot-dissolving drug within six hours may also improve outcome compared to no treatment. Depending upon a patient's overall medical condition and specific stroke type, they may be eligible for this treatment. These treatments are more specialized and require special facilities and physicians who are trained to perform these procedures.
Currently, a large number of clinical studies are looking at ways to improve the outcome of patients having a stroke. Most of these treatments, however, need to be started within six hours from stroke onset. This time factor makes it very important to seek medical attention as quickly as possible and at a hospital that specializes in stroke treatment.
What tests are available to diagnose a stroke?
One or more of the following tests may be required to accurately diagnose a stroke:
- Computed tomography (CT) brain scan. This test involves taking a series of images of the brain to determine if bleeding may be a cause of the stroke. The brain tissue is also examined to see if irreversible brain damage has occurred. This test takes 15-20 minutes with only a slight amount of X-ray exposure. It is non-invasive and does not hurt.
- Computed tomography angiogram (CTA). This test is done in the CT scanner. Intravenous contrast (dye) is given and pictures are taken of the major blood vessels in and around the brain. This test is used to detect large blood vessels that may be blocked. It takes 15-20 minutes to perform and does not hurt.
- Magnetic resonance imaging (MRI)/Magnetic resonance angiography (MRA). This test uses the body's own magnetic properties to look at the brain tissue and the blood vessels. In some cases, an MRI can also be used to evaluate how much damage has already occurred to the brain tissue and brain function. This test takes 20-30 minutes to perform and does not hurt.
- Cerebral angiogram. This test involves guiding a catheter (small tube) from the leg blood vessels into the blood vessels of the neck and injecting a contrast material to see the blood flow. This lets a doctor see all the brain's large and small blood vessels. It is the most accurate test for directly looking at all of the brain's blood vessels to detect any blockages that may have caused a stroke. It is also used to determine if an aneurysm is present or if a blood vessel is abnormal. Although slightly more invasive, it is often required to accurately assess whether there is an abnormality.
- Lumbar puncture (Spinal Tap). This test involves placing a very small needle into the back and into the lumbar subarachnoid space and withdrawing a small amount of cerebrospinal fluid (CSF). It is the most accurate test to find out if a small amount of bleeding has occurred around the brain that may have resulted in a hemorrhagic stroke.
- Ultrasound or "Doppler" scan. This test involves placing a small transducer probe over the neck or forehead. Ultrasound waves are then used to look at the blood flow in the neck and the larger blood vessels of the brain. It does not hurt, and it allows rapid evaluation of the relative amount of blood flowing to the brain.
- Nuclear medicine scan. This test involves administering very small amounts of radioactive dye intravenously. The blood vessels and/or brain tissue are scanned to evaluate the relative amount of blood flowing to the brain and to look at brain function and activity.
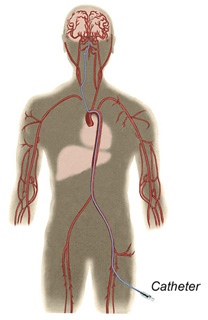
Cerebral angiogram
What treatments are available for ischemic strokes?
Ischemic strokes are caused by blood clots that block normal flow in brain blood vessels. If a person can be treated within three hours of their first symptoms, they benefit from intravenous tPA given to dissolve the blood clot. It has been shown that chances of complete recovery improve by 30 percent when tPA is used soon enough on the correct types of stroke.
If a stroke is caused by an atherosclerotic plaque blocking a blood vessel, the patient may need a procedure to open up the vessel. If the blocked blood vessel is in the neck, they may need surgery (carotid endarterectomy) to open it.
However, if the blood vessel isn't in an area suitable for surgery, a procedure called balloon angioplasty and stent placement may be more appropriate. This procedure involves going inside the blood vessel with a small balloon, and inflating the balloon to open and dilate the blocked artery. In some cases, a small metallic tube called a "stent" is inserted to help keep the blood vessel open.
What treatments are available for hemorrhagic (bleeding) strokes?
Many hemorrhagic strokes are caused by bleeding from a ruptured intracranial aneurysm. An aneurysm should be treated as quickly as possible, since there is a very high chance of repeated bleeding.
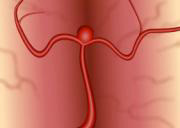
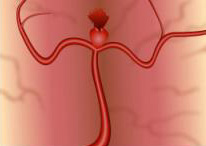
Aneurysm that has not ruptured Ruptured aneurysm
More bleeding results in further brain injury or possibly death.
An aneurysm can be treated either by direct surgical clipping by a neurosurgeon or by treatment from inside the blood vessels (similar to an angiogram) by an interventional neuroradiologist.
Using X-ray guidance, the interventional neuroradiologist threads a catheter through the brain blood vessels directly into the aneurysm. Very soft, tiny platinum coils can then be carefully placed into the aneurysm to prevent more bleeding. Depending upon the size and location of the aneurysm, and the patient's condition, either surgical clipping or this endovascular coil treatment may be recommended.
Sometimes bleeding may be due to other causes, including an arteriovenous malformation. This occurs when, tiny abnormal blood vessels have become weakened and burst.
An angiogram is usually performed to identify the cause of bleeding into the brain.
What specialists are trained to evaluate stroke patients?
Different kinds of specialists are available depending on the type of stroke being treated.
- Emergency room doctor. Specializes in the rapid evaluation of any and all types of medical emergencies. Patients should inform the emergency room doctor if they believe they may be having a stroke so the emergency room doctor can make a rapid and thorough assessment. If a patient arrives within three hours of when the stroke began, they could be eligible to receive a clot-dissolving drug. This drug has been shown to improve outcomes by 30 percent if it is given within the first three hours.
- Stroke neurologist. Specializes in evaluating and medically managing ischemic and hemorrhagic strokes. Has special training to recognize and treat strokes and to offer the most effective management of clot-dissolving drugs, blood pressure and other required medical therapies.
- Neurosurgeon. Specializes in surgically managing strokes. If a stroke is due to a ruptured aneurysm, vascular malformation or cerebral bleeding, surgery may be necessary to clip the aneurysm or remove a blood clot in the brain.
- Vascular surgeon. Specializes in surgically treating carotid artery disease due to atherosclerosis. If one of the major blood vessels to the brain, such as the carotid artery, is blocked, treating the blockage may require a procedure called "carotid endarterectomy." This procedure involves opening up the blood vessel in the neck and surgically removing the atherosclerotic plaque to restore normal blood flow.
- Interventional neuroradiologist/endovascular neurosurgeon. Specializes in the interventional treatment of stroke using X-rays to see the damage and visualize treatment of the condition. If a stroke is due to a blood clot in the brain, it may be possible to place a small tube (catheter) directly into the clot and dissolve it or break it up to improve blood flow.
If the stroke is due to a blockage from plaque, it may be possible to open up the artery with balloon angioplasty to dilate the artery and possibly place a small metal stent across the blockage to keep the blood vessel open.
If the stroke is due to an aneurysm or vascular malformation in the brain, it may be possible to treat the condition by placing small coils and other materials into the bleeding site to prevent more bleeding. - Diagnostic neuroradiologist. Specializes in the rapid diagnostic evaluation of stroke and brain and spinal cord diseases. Special tests may be done to quickly and accurately diagnose the cause of a stroke, including computed tomography, magnetic resonance imaging, and diagnostic cerebral angiography. Has special expertise and training to rapidly perform these examinations, and diagnose the underlying condition.
Who performs the more-advanced interventional stroke treatments?
Interventional neuroradiologist/endovascular neurosurgeons perform these delicate operations in the brain to treat acute strokes. These doctors have had additional specialized training. That training is required in order to navigate within the delicate brain blood vessels to open up blocked arteries or close off weakened areas of blood vessels (aneurysms) that may have ruptured and bled.
Not every hospital has interventional neuroradiologists with these capabilities, so it is important that a patient who has stroke symptoms be taken to a facility that has these capabilities to maximize their chances for successful treatment.
For more information, contact the American Stroke Association, a division of the American Heart Association, at 1-888-4-STROKE (1-888-478-7653) or visit StrokeAssociation.org.


What You Should Know About Cerebral Aneurysms
From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council
Randall T. Higashida, M.D., Chair
What is a cerebral aneurysm?
An aneurysm is a weak area in a blood vessel that usually enlarges. It's often described as a "ballooning" out of the blood vessel.
How common are aneurysms?
It is estimated that 1.5-5 percent of the general population has or will develop a cerebral aneurysm. It is also estimated that 3-5 million people in the United States have cerebral aneurysms, but most are not producing any symptoms. Annually, between 0.5-3 percent of people with a brain aneurysm may suffer from bleeding.
How do aneurysms form? Are people born with an aneurysm?
Usually, people are not born with them. Most develop after the age of 40. Aneurysms usually develop at branching points of arteries and are caused by constant pressure from blood flow. They often enlarge slowly and become weaker as they grow, just as a balloon becomes weaker as it stretches. Aneurysms may be associated with other types of blood vessel disorders, such as fibromuscular dysplasia, cerebral arteritis or arterial dissection, but these are very unusual. They may run in families, but people are rarely born with a predisposition for aneurysms. Some aneurysms are due to infections, drugs such as amphetamines and cocaine that damage the brain's blood vessels, or direct brain trauma from an accident.
Are all aneurysms the same?
Brain aneurysms are all different. They vary in size, shape and location.
Size
- Small aneurysms are less than 5 mm (1/4 inch).
- Medium aneurysms are 6-15 mm (1/4 to 3/4 inch).
- Large aneurysms are 16-25 mm (3/4 to 1 1/4 inch).
- Giant aneurysms are larger than 25 mm (1 1/4 inch).
Shape
Aneurysms can be:
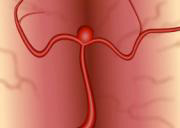
Saccular (sac-like), with a well-defined neck
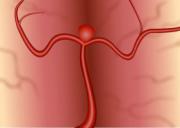
Broad-based with a wide neck
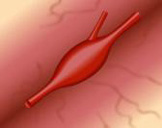
Fusiform (spindle shaped) without a distinct neck
Location
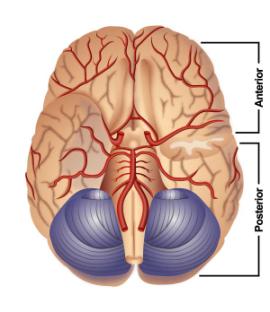
An aneurysm is usually located along the major arteries deep within brain structures. When approaching an aneurysm during surgery, normal brain tissue must be carefully spread apart to expose it. Aneurysms can occur in the front part of the brain (anterior circulation) or the back part of the brain (posterior circulation) .
How is an aneurysm diagnosed?
A brain aneurysm needs to be detected by special imaging tests. Two non-invasive tests show the blood vessels in the brain. In the first, called CTA (Computed Tomographic Angiography), patients are placed on a table that slides into a CT scanner. A special contrast material (dye) is injected into a vein and images are taken of the blood vessels to look for abnormalities such as an aneurysm.
In the second test, called an MRA (Magnetic Resonance Angiography), patients are placed on a table that slides into a magnetic resonance scanner, and the blood vessels are imaged to detect a cerebral aneurysm. Both of these screening tests are useful to detect most cerebral aneurysms larger than 3-5 mm (about 3/16 inch).
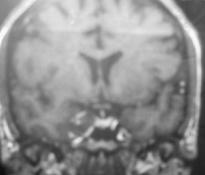
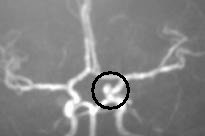
Magnetic resonance image of normal brain tissues Magnetic resonance angiogram of a small brain aneurysm
The most reliable test is called a diagnostic cerebral angiogram. In this test, the patient lies on an X-ray table. A small tube (catheter) is inserted through a blood vessel in the leg and guided into each of the blood vessels in the neck that go to the brain. Contrast material (dye) is then injected, and pictures are taken of all of the blood vessels in the brain. This test is slightly more invasive and less comfortable, but it is the most reliable way to detect all types and sizes of cerebral aneurysms.
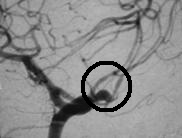
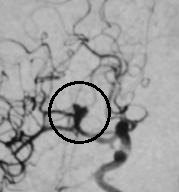
Two cerebral angiogram images showing brain aneurysms
Before any treatment is considered, a diagnostic cerebral angiogram is usually performed in order to fully map a plan for therapy.
If one aneurysm forms, will others form?
The presence of one aneurysm is associated with a 15-20 percent chance of having at least one or multiple other aneurysms.
What are the symptoms of an unruptured aneurysm?
Most smaller aneurysms have no symptom. As an aneurysm enlarges, however, it can produce headaches or localized pain. If an aneurysm gets very large, it may produce pressure on the normal brain tissue or adjacent nerves. This pressure can cause difficulty with vision, numbness or weakness of an arm or leg, difficulty with memory or speech, or seizures.
What causes an aneurysm to bleed?
We usually don't know why an aneurysm bleeds or exactly when it will bleed. We do know what increases the chance for bleeding:
- High blood pressure, often due to heavy lifting or straining, is one possibility.
- Strong emotions, as when people become upset or angry, can also cause aneurysms to rupture.
- Blood "thinners" (such as warfarin), some medications and prescription drugs (including diet pills that act as stimulants such as ephedrine and amphetamines), and harmful drugs like cocaine can cause aneurysms to rupture and bleed.
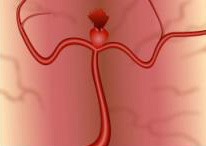
Ruptured aneurysm
What are the chances that an unruptured aneurysm may bleed?
Many factors determine whether an aneurysm is likely to bleed. These include the size, shape and location of the aneurysm and symptoms that it causes. Smaller aneurysms that are uniform in size may be less likely to bleed than larger, irregularly shaped aneurysms. Once an aneurysm has bled, there is a very high chance of re-bleeding. That is why treatment as soon as possible is recommended.
What happens if an aneurysm bleeds?
If an aneurysm ruptures, it leaks blood into the space around the brain. This is called a "subarachnoid hemorrhage." Depending upon the amount of blood, it can produce:
- a sudden severe headache that can last from several hours to days
- nausea and vomiting
- drowsiness and/or coma.
The hemorrhage may also damage the brain directly, usually from bleeding into the brain itself. This is called a " hemorrhagic stroke" This can lead to
- weakness or paralysis of an arm or leg
- trouble speaking or understanding language
- vision problems
- seizures
What is the usual damage to the brain after an aneurysm bleeds?
Once an aneurysm bleeds, there is a 30-40 percent chance of death, and a 20-35 percent chance of moderate to severe brain damage, even if the aneurysm is treated. 15-30 percent of patients have only mild difficulties or almost none. If the aneurysm is not treated quickly enough, another bleed may occur from the already ruptured aneurysm.
In 15-20 percent of patients, vasospasm (irritation by the leaked blood causing narrowing of the blood vessels) may occur. This can lead to further brain damage. Other problems may include hydrocephalus (enlargement of the spaces within the brain that produce cerebrospinal fluid); difficulty breathing that requires a mechanical ventilator, and infection. Heart and lung problems may result due to extensive brain damage that can affect the body's normal functions.
Why is the damage so extensive after bleeding?
Once blood enters the brain and the space around it, direct damage to the brain tissue and brain function results. This amount of damage is usually related to the amount of blood. Damage is due to the increased pressure [DM7]and swelling from bleeding directly into the brain tissue, or from local cellular damage to brain tissue from irritation of blood in the space between the brain and the skull.
Blood can also irritate and damage the normal blood vessels and cause vasospasm (constriction). This can interrupt normal blood flow to the healthy brain tissue and can cause even more brain damage.
Will treating a ruptured aneurysm reverse or improve brain damage?
Once an aneurysm bleeds and brain damage occurs, treating the aneurysm will not reverse the damage. Treatment is necessary, but the treatment only helps prevent more bleeding, which can cause more damage to the brain and, consequently, to the body's functions.
If bleeding has already caused brain damage, patients may benefit from rehabilitation therapy once the aneurysm has been treated.
How is a treatment method for aneurysm chosen?
Each patient and each aneurysm is different. Doctors must evaluate the risk factors that favor treatment vs. non-treatment and must decide which technique may be best.
It is important to consult with experts in this field. This should include a discussion with a cerebrovascular neurosurgeon who specializes in surgically clipping aneurysms and an interventional neuroradiologist/endovascular surgeon who specializes in the less invasive treatment of cerebral aneurysms by coiling. These 2 types of medical specialists are usually different, and have different expertise and training backgrounds. It is highly recommended to have a consultation with both types of physicians.
How should an aneurysm be treated?
The best treatment depends upon many things, including whether the aneurysm has ruptured or not. A ruptured aneurysm usually requires treatment right away, because the re-bleeding rate remains quite high. However, the treatment time and options for treatment depend upon the size, location and shape of the aneurysm, as well as the patient's overall medical condition.
If an aneurysm has not ruptured, the treatment decision depends upon its size, location and shape, and the patient's symptoms. Each factor is important and requires consultation with a neurosurgeon and an interventional neuroradiologist who has special skills and training in treating these types of aneurysms.
What treatments are available?
Medical therapy. Small, unruptured aneurysms that are not creating any symptoms may not need treatment unless they grow, trigger symptoms or rupture. It is very important to have annual check-ups to monitor blood pressure, cholesterol, and other medical conditions. Small, unruptured aneurysms require regular imaging examinations to make sure that they have not grown or changed significantly.
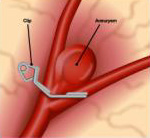
Surgical clipping of an aneurysm
Neurosurgery. Depending upon an individual's risk factors, open surgery may be recommended. Patients are placed under general anesthesia, an opening is made in the skull, the brain tissue is spread apart and the aneurysm is surgically exposed. Then the neurosurgeon places a surgical clip around its base. The clip seals off the aneurysm so blood cannot enter. For an uncomplicated surgical clipping procedure, the hospital stay is usually 4-6 days. Recovery after the operation takes 3-6 weeks.
Interventional neuroradiology/endovascular neurosurgery. Depending upon the aneurysm's size, location and shape, it may be possible to treat the aneurysm from inside the blood vessel. This minimally invasive procedure is similar to the cerebral angiogram. However, in addition to taking pictures, a small tube (catheter) is directed through the blood vessels into the aneurysm itself.
Then, using X-ray guidance, the endovascular surgeon carefully places soft platinum micro-coils into the aneurysm and detaches them. The coils stay within the aneurysm and act as a mechanical barrier to blood flow, thus sealing it off. For an uncomplicated procedure, the hospital stay usually lasts 1-2 days. Recovery after the operation usually takes 5-7 days.
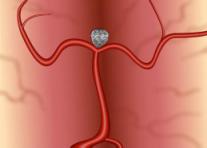
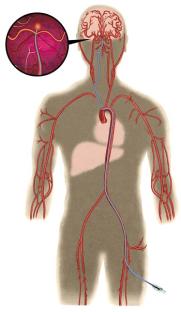
Endovascular coiling of a cerebral aneurysm
For a complicated surgery or endovascular treatment, or if an aneurysm has bled into the brain, hospitalization may be for 1-4 weeks, depending upon the patient's medical condition and any complications caused by the hemorrhage.
What are the potential complications of aneurysm treatment?
Until the aneurysm is safely and completely treated, there is always the risk it may re-bleed and cause more brain damage. If normal blood vessels are damaged, it could also result in more brain damage. This could cause weakness or paralysis of the arm or leg, difficulty with speech or understanding, vision loss, confusion, loss of memory and/or seizures. There is also the risk of the anesthesia itself, infection, bleeding, damage to the kidneys from the X-ray dye and other potential problems.
All these risks need to be carefully considered when deciding upon a course of treatment. There are risks if the aneurysm is not treated. The aneurysm may bleed or grow in size.
What follow-up is required after aneurysm treatment?
There are two follow-up procedures depending on the type of treatment:
- Surgical clipping. After this type of surgery, a post-operative angiogram is usually performed during the hospital stay to make sure the surgical clip has completely treated the aneurysm.
- Interventional neuroradiology/endovascular neurosurgery. After coiling an aneurysm, a routine follow-up angiogram is usually performed 6-12 months after the procedure to make sure the aneurysm remains blocked off. In some cases, particularly with larger aneurysms, further coil treatment may be needed to make sure the aneurysm is no longer at risk.
About Strokes and Cerebrovascular Diseases
Stroke and cerebrovascular diseases are the third-leading cause of death and a leading cause of major disability in the United States. More than 700,000 new and recurrent strokes occur each year, resulting in about 167,000 deaths and more than 250,000 permanent disabilities per year in the United States. More than 4.7 million stroke survivors are alive today.
Hemorrhagic strokes are caused by bleeding into the brain, causing either death or major disability. Cerebral aneurysm ruptures account for the majority of these hemorrhagic strokes each year.
About ISAT: International Subarachnoid Aneurysm Trial
What is ISAT?
The International Subarachnoid Aneurysm Trial, or ISAT is the only multi center prospective randomized trial that compares surgical clipping with endovascular coiling for the treatment of ruptured intracranial aneurysms. This means that patients with aneurysms that could be treated by either surgery or coiling were enrolled and randomly assigned to receive one of these two treatments. They were then followed to see how they recovered. Published in the British Medical Journal, The Lancet, the study concluded that "in patients with a ruptured intracranial aneurysm, for which endovascular coiling and neurosurgical clipping are therapeutic options, the outcomes in terms of survival free of disability at 1 year is significantly better with endovascular coiling."1
Which kind of patients suffering from an aneurysm were treated in ISAT?
ISAT's primary criteria for enrollment was that a patient with a ruptured aneurysm who was treated at one of the trial centers had to be judged equally suitable for either surgical or endovascular therapy by the treating physician. The trial was designed to show whether a policy of endovascular treatment would reduce the percentage of patients with poor or moderate outcomes at one year post treatment compared to a policy of surgical treatment. The trial protocol was peer reviewed and approved by the Medical Research Council of the United Kingdom.
How many patients were enrolled in ISAT and what does the data mean?
On May 2, 2002, after enrolling 2143 of the planned 2,500 patients, ISAT halted patient enrollment into the trial following a planned data review by the Data Monitoring Committee that found that the trial had reached its primary endpoint and that it was no longer ethical to randomize patients to neurosurgery with clipping. Although enrollment ended, data analysis and patient follow-up still continues.
How can I find more date about ISAT?
On October 26, 2002, The Lancet published the ISAT findings. The article was reprinted in the November-December issue of the Journal of Stroke and Cerebrovascular Disease. For the 1594 patients with one-year post treatment outcomes, the relative risk of dependence or death for patients assigned to endovascular therapy was 22.6% lower than that of patients assigned to surgical therapy with an absolute risk reduction of 6.9%. The study concluded that "in patients with a ruptured intracranial aneurysm, for which endovascular coiling and neurosurgical clipping are therapeutic options, the outcomes in terms of survival free of disability at 1 year is significantly better with endovascular coiling." The risk of rebleeding after one year was low for both procedures- two per 1276 patient years for endovascular therapy and zero per 1081 patient years for surgery.
Will there be additional data coming out of this trial?
Begun in 1994 with a pilot study and commencing full enrollment in 1997, ISAT involved 43 centers in the UK, Europe, Australia, and North America. The trial was funded by the Medical Research Council (UK), French Ministry of Health, Assistance Publique, Hopitaux de Paris, Canadian Institutes of Health Research, and the Stroke Association of the UK. ISAT will continue to publish data and findings through 2007. Among the issues that ISAT will address are long-term risk of rebleeding, neuropsychological outcomes, quality of life and health economic results.
What people are saying about ISAT?
"Patients with an aneurysm really need to be evaluated in a center that offers both kinds of treatment, in a truly unbiased setting where their aneurysm is evaluated by experts." (Associated Press)
1Molyneux, Andrew, et.al., "International Subarachnoid Aneurysm Trial (ISAT) of neurosurgical clipping versus endovascular coiling in 2143 patients with ruptured intracranial aneurysms: a randomised trial." THE LANCET Saturday 26, October 2002 Vol. 360 No. 9342 Pages 1267-1274
For more information, contact the American Stroke Association, a division of the American Heart Association, at 1-888-4-STROKE (1-888-478-7653) or visit StrokeAssociation.org.
Funded through an educational grant provided by Boston Scientific

https://ucsf.zoom.us/j/95624427396?pwd=Z3p2d3loQUt3ZWFvOWV4Yy83ZE9wUT09
____________________________________________________________________________________________________________________________________________________________________________________________________________
The Raaen family established the Allison Raaen Lectureship in 2009 in memory of their daughter who died from an AVM rupture in November 2005. The annual lecture features distinguished speakers involved in cutting edge basic and translational research and aims to stimulate communication and advances in understanding cerebrovascular malformations. In 2014, the Lectureship was renamed to the William L. Young/Allison Raaen Lectureship to honor the seminal contributions of the late Dr. William L. Young, founding Director of the UCSF Center for Cerebrovascular Research and world-renowned AVM researcher.


Allison Raaen Dr. William L. Young
The 12th Annual William L. Young/Allison Raaen Lectureship

April 20, 2023
Guest Speaker: Dr. Beth Roman
More information to be announced soon.
The 11th Annual William L. Young/Allison Raaen Lectureship
September 23, 2021
Guest Speaker: Dr. Ivan Radovanovic MD, PhD
Associate Professor, Department of Surgery, University of Toronto.
"Brain Aretriovenous Malformations: Genetics, Development Biology and Perspectives for Targeted Therapies"
The 10th Annual William L. Young/Allison Raaen Lectureship

September 16, 2019
Guest Speaker: Dr. Patrick Turski, MD, FACR
Emeritus Professor of Radiology, Neurological Surgery and Medical Physics from the University of Wisconsin
"Exploring Brain AVM Morphology and Hemodynamics using 4D Flow MRI."
The 9th Annual William L. Young/Allison Raaen Lectureship

August 9, 2018, 8-9 AM
Guest Speaker: Issam A. Awad, MD, Msc FACS MA (hon)
The John Harper Seeley Professor of Surgery
Director, Neurovascular Surgery
Director, Safadi program of Excellence in Clinical and Translational Neuroscience
University of Chicago
“Cavernous Angiomas with Symptomatic Hemorrhage (CASH); Mechanistic Targets and Trial Models”
The 8th Annual William L. Young/Allison Raaen Lectureship

June 15, 2017, 8-9 AM
Guest Speaker: Kevin J. Whitehead, MD, FAHA
Associate Professor of Cardiovascular Medicine and Pediatric Cardiology
University of Utah
Co-Director, Utah HHT Center for Excellence
“Medical Therapy for Vascular Malformations: the Hope and the Challenges”
The 7th Annual William L. Young/Allison Raaen Lectureship

June 23, 2016, 8-9 AM
Guest Speaker: Christian Stapf, MD
Principal Scientist & Professor
Department of Neurosciences, University of Montréal
Attending Neurologist, Department of Neurology
Centre Hospitalier de l’Université de Montréal
"Evidence-based Approach to AVM Patient Management"
The 6th Annual William L. Young/Allison Raaen Lectureship

June 25, 2015, 8:00 AM
Guest Speaker: Hui Meng, Ph.D.
Professor of Mechanical & Aerospace Engineering and Neurosurgery
Department of Biomedical Engineering
State University of New York at Buffalo
"Role of Modeling in Translational Research of Intracranial Aneurysm"
The 5th Annual William L. Young/Allison Raaen Lectureship

April 24, 2014, 8:00 AM
Guest Speaker: Doug Marchuk, Ph.D.
Professor and Vice-Chair,
Department of Molecular Genetics and Microbiology, Duke University
Director, Duke University Program in Genetics and Genomics
"Cerebral Cavernous Malformations: From Gene Discovery to Potential Therapy"
The 4th Annual Allison Raaen Lectureship

November 8, 2012, 8:00 AM
Guest Speaker: Marie E. Faughnan, MD, MSc
Associate Professor, University of Toronto Director,
Toronto HHT Program St. Michael's Hospital, Division of Respirology
"HHT and Brain AVMs: Building and Breaking Connections"
The 3rd Annual Allison Raaen Lectureship

October 6, 2011, 8:00 AM
Guest Speaker: Christopher C. W. Hughes, PhD
Professor and Chair, Department of Molecular Biology and Chemistry
University of California, Irvine
"Why Does Loss of Alk1 and Endoglin Cause HHT? Probing the Molecular Mechanisms of Blood Vessel Assembly"
The 2nd Annual Allison Raaen Lectureship
September 9, 2010, 8:00 AM
Guest Speaker: Dean Li, MD, PhD
HA and Edna Benning Endowed Professor, Medicine and Cardiology
Director, Molecular Medicine Program
University of Utah
"Vascular Stability in Sepsis and Stroke"
The 1st Annual Allison Raaen Lectureship
April 2, 2009, 8:00 AM
Guest Speaker: S. Paul Oh, PhD
Associate Professor, Department of Physiology
University of Florida
"Novel Genetic Models for Brain Arteriovenous Malformations"
Reduction of brain AVM severity through inhibition of pathogenic angiogenesis
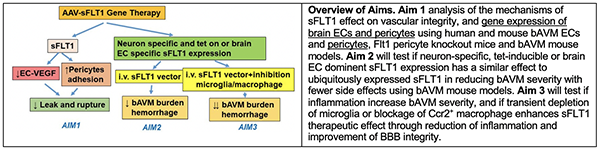
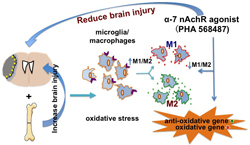
The most devastating symptom in patients with brain arteriovenous malformation (bAVM) is intracranial hemorrhage caused by rupture of bAVM vessels, which is unpredictable and life threatening. Available treatment options for bAVM are invasive and risky. Treatment of unruptured bAVMs has become increasingly controversial because the natural history for these patients may be less morbid than invasive therapies. There is currently no specific medical therapy available to bAVM patients. Vascular endothelial growth factor (VEGF) is involved in normal and pathological angiogenesis. The level of VEGF is abnormally high in bAVM lesions, which is associated with the increase of blood-brain barrier (BBB) permeability and bAVM hemorrhage. Therefore, inhibition of VEGF may stabilize bAVM vessel walls and reduce bAVM rupture. Soluble FMS-related tyrosine kinase 1 (sFLT1) contains the extracellular domain of VEGFR-1 and binds to VEGF with high affinity and thus reduces VEGF signaling through all of its membrane-bound receptors, not just VEGFR-2. sFLT1 also has a direct role in maintaining normal pericytic function. However, ubiquitous expression of sFLT1 caused minor liver inflammation and growth arrest in young mice with. In this study, we will test our hypotheses that sFLT1 improves bAVM vessel integrity by inhibiting VEGF downstream signaling and improving adhesion of pericytes and endothelial cells, targeted and controlled sFLT1 expression reduces bAVM severity with minimal side effects, and reduction of microglia/macrophage infiltration enhances sFLT1 therapeutic effect. The overarching goal of this project is to develop a safe and effective method to prevent bAVM hemorrhage.
Genetics of cerebrovascular anomalies
The genetic defects in several familial or inherited types of stroke syndromes are known; much less well understood are the genetic defects in "sporadic" stroke syndromes. In collaboration with the UCSF Cardiovascular Research Institute and the Department of Genetics at Duke University, these studies are designed to define the interaction of subtle genetic alterations in key signaling pathways that are necessary for normal development and maintenance of the vascular endothelium. If these systems are not operating correctly, defects such as structural flaws in the blood vessel or a predisposition to clot formation may result.
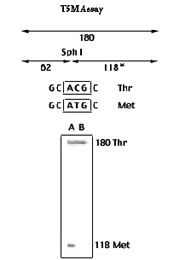
Brain Vascular Malformation Consortium
The Brain Vascular Malformation Consortium (BVMC) seeks to explore the natural history, epidemiology, diagnosis, and treatment of several rare vascular diseases of the brain. In collaboration with patient advocacy groups, we are actively recruiting patients with familial cerebral cavernous malformations (CCM), Sturge-Weber Syndrome (SWS), and hereditary hemorrhagic telangiectasia (HHT) with and without brain arteriovenous malformations (BAVM). The BVMC is one of 20 funded consortia that comprise the Rare Diseases Clinical Research Network (RDCRN), a collaboration between the Office of Rare Diseases, the National Center for Advancing Translational Sciences, and the National Institute for Neurological Disorders and Stroke.
- Consortium Spotlight: https://www.rarediseasesnetwork.org/news/2021-10-07-BVMC-Consortium-Spotlight
- Senior Researcher Spotlight: https://www.rarediseasesnetwork.org/news/2021-10-13-BVMC-Researcher-Spotlight

Publications on CCM since 2014
Publications on SWS since 2014
Publications on HHT since 2014
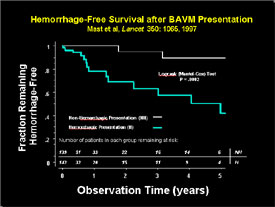
Epidemiology and clinical course of brain arteriovenous malformations (BAVM)
BAVMs are a rare but treatable cause of stroke from bleeding into the brain. These studies seek to define what the risks of neurologic damage are from both the natural history of the disease as well as from treatment of the disease. By knowing the balance between natural history and treatment risks in different subgroups of patients, more rational care can be offered to patients. Use of novel clinical trial methodologies and statistical modeling are used for this work. Parts of these studies are undertaken in conjunction with Kaiser-Permanente Northern California to examine aspects of natural history in a population-based cohort
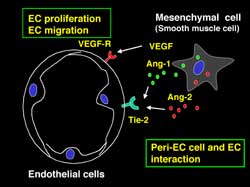
Endothelial biology of brain cerebrovascular malformations
By examining surgical specimens with the tools of molecular biology, the pathways associated with the development of human vascular malformations can be studied. Examples of these malformations include BAVMs, cavernous malformations, dural arteriovenous fistulas, and aneurysms. By use of cell culture systems and the development of small animal models, mechanistic studies can be undertaken to unravel the missteps in development or maturation which result in the human disease. From these studies, insights into better treatment strategies can be undertaken. A key system of interest is the Tie-2 / Angiopoietin signaling pathway.
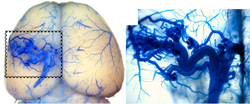
Cerebrovascular malformation modeling, mechanistic study and new therapy developmen
Modeling, exploring the pathogenesis and developing new therapies for arteriovenous malformation (AVM) are the major focuses of the basic research team. Through manipulation of relative genes, and the levels of various angiogenic factors, we have successfully built several brain arteriovenous malformation (AVM) models. These models also have AVM in other organs. They are powerful tools for dissecting AVM pathogenesis and test innovative therapeutic strategies. The figures show an AVM lesion in the brain in one of our models.
Impact of peripheral and brain injuries
We found that long-bone fracture upregulates innate immune response systemically and locally in the brain, which causes exaggerated neuronal damage and behavior deficits. We are trying to understand how peripheral injury influences stroke recovery. We are also testing new strategies to modulate innate immune response to improve the outcomes in stroke patients with advanced age or with peripheral injury.
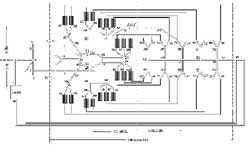
Computational modeling of the cerebral circulation
By the development of computational models, it is often possible to take incomplete sets of experimental data and generate likely hypotheses to further test. Further, theoretical modeling of BAVM rupture risk can be used to improve selection of variables to develop for use in risk stratification purposes in clinical trials. A long-term goal of this line of inquiry is to eventually develop "patient-specific" physiologic models that can be used in conjunction with modern anatomic imaging for treatment planning and outcome assessment.
In collaboration with scientists from the Vascular Imaging Research Center, we are studying the effect of abnormal flow profiles that are present in cerebral aneurysms and arteriovenous malformations using magnetic resonance imaging and computational fluid dynamic modeling.
Books Edited by CCR Members
Hua Su, Michael T Lawton (Co-Editor), Molecular Genetic and Cellular Advances in Cerebrovascular Disease (Book). Publisher: World Scientific Publishing Co., 2018.
Cottrell JE, Young WL, Editors: Cottrell and Young's Neuroanesthesia, 5th ed. Philadelphia, Mosby Elsevier, 2010
Miller RD, Eriksson LI, Fleischer LA, Wiener-Kronish JP, Young WL, Editors: Miller's Anesthesia, Vol 1 & 2. 7th ed. New York, Churchill Livingstone, 2010
Jin K, Yang GY, Co-Editors: Experimental Stroke, Bentham eBooks. Bentham Science Publishers, 2008
Miller RD, Fleischer LH, Johns RA, Savarese JJ, Wiener-Kronish J, Young WL, Editors: Miller's Anesthesia, Vol 1 & 2. 6th ed. New York, Churchill Livingstone, 2005
Batjer HH, Editor-in-Chief, Caplan LR, Friberg L, Greenlee RG, Jr., Kopitnik TA, Young WL, Associate Editors: Cerebrovascular Disease, Philadelphia, Lippincott-Raven, 1997
Selected Publications
2023
Lu AY, Winkler EA, Garcia JH, Raygor KP, Fullerton HJ, Fox CK, Kim H, Auguste KI, Sun PP, Hetts SW, Lawton MT, Abla AA, Gupta N. A comparison of incidental and symptomatic unruptured brain arteriovenous malformations in children. J Neurosurg Pediatr. 2023 05 01; 31(5):463-468. PubMed
Kim KH, Nelson NJ, Salman SR, Flemming FK, Hess HC, Hetts HS, Koroknay-Pál KP, Laakso LA, Lanzino LG, Lawton LM, McCulloch MC, Moayeri MN, Mohr MJ, Morgan MM, Stefani SM, Zaroff ZJ, Zhao ZY. Abstract 53: Long-term Treatment Risk Of Hemorrhage In Unruptured Brain Arteriovenous Malformation Patients. Stroke. 2023 Feb 1; 54(Suppl_1):a53-a53. View in Publisher Site
Zaw ZT, Weinsheimer WS, Nelson NJ, McCulloch MC, Zaroff ZJ, Kim KH. Abstract TMP17: Polymorphisms In DNA Methylated Genes And Risk Of Intracranial Hemorrhage In Brain Arteriovenous Malformation Patients. Stroke. 2023 Feb 1; 54(Suppl_1):atmp17-atmp17. View in Publisher Site
Chawla CS, Weinsheimer WS, Nelson NJ, McCulloch MC, Abla AA, Gupta GN, Cooke CD, Hetts HS, Saloner SD, Li LY, Fox FC, Fullerton FH, Kim KH. Abstract TP157: Interleukin Plasma Levels And Risk Of Hemorrhage In Pediatric Brain Arteriovenous Malformation Patients View in Publisher Site
Winkler WE, Garcia GJ, Tsang TC, Nelson NJ, McCulloch MC, Weinsheimer WS, Fox FC, Fullerton FH, Ko KN, Su SH, Nowakowski NT, Cooke CD, Hetts HS, Guney GE, PEKMEZCI PM, Tihan TT, Lawton LM, Abla AA, Gupta GN, Kim KH. Abstract 52: Prevalence Of Somatic Activating Kras Mutations In Pediatric And Adult Sporadic Brain Arteriovenous Malformations. View in Publisher Site
Weinsheimer S, Nelson J, Abla AA, Ko NU, Tsang C, Okoye O, Zabramski JM, Akers A, Zafar A, Mabray MC, Hart BL, Morrison L, McCulloch CE, Kim H, Brain Vascular Malformation Consortium Cerebral Cavernous Malformation Investigator Group *. Intracranial Hemorrhage Rate and Lesion Burden in Patients With Familial Cerebral Cavernous Malformation. PubMed
Yusuf H, Rasheed A, Kim H, Conrad MB, Hetts SW. Identifying racial disparities in hereditary hemorrhagic telangiectasia. J Neurointerv Surg. 2023 Oct; 15(10):1050-1054. PubMed
2022
Winkler E, Wu D, Gil E, McCoy D, Narsinh K, Sun Z, Mueller K, Ross J, Kim H, Weinsheimer S, Berger M, Nowakowski T, Lim D, Abla A, Cooke D. Endoluminal Biopsy for Molecular Profiling of Human Brain Vascular Malformations. Neurology. 2022 Apr 19;98(16):e1637-e1647. doi: 10.1212/WNL.0000000000200109. Epub 2022 Feb 10. PubMed
Similuk MN, Yan J, Ghosh R, Oler AJ, Franco LM, Setzer M, Kamen M, Jodarski C, DiMaggio T, Davis J, Gore R, Jamal L, Borges A, Gentile N, Niemela J, Lowe C, Jevtich K, Yu Y, Hullfish H, Hsu AP, Hong C, Littel P, Seifert BA, Milner J, Johnston JJ, Cheng X, Li Z, Veltri D, Huang K, Kaladi K, Barnett J, Zhang L, Vlasenko N, Fan Y, Karlins E, Ganakammal SR, Gilmore R, Tran E, Yun A, Mackey J, Yazhuk S, Lack J, Kuram V, Cao W, Huse S, Frank K, Fahle G, Rosenzweig S, Su Y, Hwang S, Bi W, Bennett J, Myles IA, De Ravin SS, Fussm I, Strober W, Bielekova B, Almeida de Jesus A, Goldbach-Mansky R, Williamson P, Kumar K, Dempsy C, Frischmeyer-Guerrerio P, Eisch R, Bolan H, Metcalfe DD, Komarow H, Carter M, Druey KM, Sereti I, Dropulic L, Klion AD, Khoury P, O' Connell EM, Holland-Thomas NC, Brown T, McDermott DH, Murphy PM, Bundy V, Keller MD, Peng C, Kim H, Norman S, Delmonte OM, Kang E, Su HC, Malech H, Freeman A, Zerbe C, Uzel G, Bergerson JRE, Rao VK, Olivier KN, Lyons JJ, Lisco A, Cohen JI, Lionakis MS, Biesecker LG, Xirasagar S, Notarangelo L, Holland SM, Walkiewicz MA. Clinical Exome Sequencing of 1000 Families with Complex Immune Phenotypes: Towards comprehensive genomic evaluations. J Allergy Clin Immunol. 2022 Jun 23. PubMed
Ananiadis T, Faughnan ME, Clark D, Prabhudesai V, Kim H, Lawton MT, Vozoris NT. Neurovascular Complications and Pulmonary Arteriovenous Malformation Feeding Artery Size. Am Thorac Soc. 2022 Apr 20. PubMed
Winkler EA, Wu D, Gil E, McCoy D, Narsinh K, Sun Z, Mueller K, Ross J, Kim H, Weinsheimer S, Berger M, Nowakowski T, Lim D, Abla A, Cooke D, Winkler E, Wu D, Gil E, McCoy D, Narsinh K, Sun Z, Mueller K, Ross J, Kim H, Weinsheimer S, Berger M, Nowakowski T, Lim D, Abla A, Cooke D. Endoluminal Biopsy for Molecular Profiling of Human Brain Vascular Malformations. Neurology. 2022 Apr 19; 98(16):e1637-e1647. PubMed
Winkler EA, Kim CN, Ross JM, Garcia JH, Gil E, Oh I, Chen LQ, Wu D, Catapano JS, Raygor K, Narsinh K, Kim H, Weinsheimer S, Cooke DL, Walcott BP, Lawton MT, Gupta N, Zlokovic BV, Chang EF, Abla AA, Lim DA, Nowakowski TJ. A single-cell atlas of the normal and malformed human brain vasculature. Science. 2022 03 04; 375(6584):eabi7377. PubMed
Sheth KN, Anderson CD, Biffi A, Dlamini N, Falcone GJ, Fox CK, Fullerton HJ, Greenberg SM, Hemphill JC, Kim A, Kim H, Ko NU, Roland JL, Sansing LH, van Veluw SJ, Rosand J, Anderson CD, Biffi A, Fox CK, Fullerton HJ, Greenberg SM, Hemphill JC, Kim A, Kim H, Ko NU, Roland JL, van Veluw SJ, Rosand J. Maximizing Brain Health After Hemorrhagic Stroke: Bugher Foundation Centers of Excellence. Stroke. 2022 03; 53(3):1020-1029. PubMed
Garcia JH, Rutledge C, Winkler EA, Carrete L, Morshed RA, Lu AY, Saggi S, Fox CK, Fullerton HJ, Kim H, Cooke DL, Hetts SW, Lawton MT, Gupta N, Abla AA. Validation of the Ruptured Arteriovenous Malformation Grading Scale in a pediatric cohort. J Neurosurg Pediatr. 2022 Feb 25; 1-5. PubMed
Sporns PB, Fullerton HJ, Lee S, Kim H, Lo WD, Mackay MT, Wildgruber M. Childhood stroke. Nat Rev Dis Primers. 2022 Feb 24; 8(1):12. PubMed
2021
Girard GR, Li LY, Stadnik SA, Shenkar SR, Hobson HN, Romanos RS, Srinath SA, Moore MT, Lightle LR, Shkoukani SA, Akers AA, Carroll CT, Christoforidis CG, Koenig KJ, Lee LC, Piedad PK, Greenberg GS, Kim KH, Flemming FK, Ji JY, Awad AI. A Roadmap for Developing Plasma Diagnostic and Prognostic Biomarkers of Cerebral Cavernous Angioma With Symptomatic Hemorrhage (CASH). Neurosurgery. 2021 Nov 18; 89(Supplement_2):s109-s109.
Kim H, Flemming KD, Nelson JA, Lui A, Majersik JJ, Cruz MD, Zabramski J, Trevizo O, Lanzino G, Zafar A, Torbey M, Mabray MC, Robinson M, Narvid J, Lupo J, Thompson RE, Hanley DF, McBee N, Treine K, Ostapkovich N, Stadnik A, Piedad K, Hobson N, Carroll T, Shkoukani A, Carrión-Penagos J, Mendoza-Puccini C, Koenig JI, Awad I. Baseline Characteristics of Patients With Cavernous Angiomas With Symptomatic Hemorrhage in Multisite Trial Readiness Project. Stroke. 2021 Sep 16; STROKEAHA120033487. PubMed
Garcia JH, Winkler EA, Morshed RA, Lu A, Ammanuel SG, Saggi S, Wang EJ, Braunstein S, Fox CK, Fullerton HJ, Kim H, Cooke DL, Hetts SW, Lawton MT, Abla AA, Gupta N. Factors associated with seizures at initial presentation in pediatric patients with cerebral arteriovenous malformations. J Neurosurg Pediatr. 2021 Sep 24; 1-6. Pubmed
Wetzel-Strong SE, Weinsheimer S, Nelson J, Pawlikowska L, Clark D, Starr MD, Liu Y, Kim H, Faughnan ME, Nixon AB, Marchuk DA. Pilot investigation of circulating angiogenic and inflammatory biomarkers associated with vascular malformations. Orphanet J Rare Dis. 2021 09 03; 16(1):372. Pubmed
Eisenmenger LB, Junn JC, Cooke D, Hetts S, Zhu C, Johnson KM, Manunga JM, Saloner D, Hess C, Kim H. Presence of Vessel Wall Hyperintensity in Unruptured Arteriovenous Malformations on Vessel Wall Magnetic Resonance Imaging: Pilot Study of AVM Vessel Wall "Enhancement". Front Neurosci. 2021; 15:697432. Pubmed
Gao S, Nelson J, Weinsheimer S, Winkler EA, Rutledge C, Abla AA, Gupta N, Shieh JT, Cooke DL, Hetts SW, Tihan T, Hess CP, Ko N, Walcott BP, McCulloch CE, Lawton MT, Su H, Pawlikowska L, Kim H. Somatic mosaicism in the MAPK pathway in sporadic brain arteriovenous malformation and association with phenotype. J Neurosurg. 2021 Jul 02; 1-8. Pubmed
Keränen S, Suutarinen S, Mallick R, Laakkonen JP, Guo D, Pawlikowska L, Jahromi BR, Rauramaa T, Ylä-Herttuala S, Marchuk D, Krings T, Koivisto T, Lawton M, Radovanovic I, Kim H, Faughnan ME, Frösen J. Cyclo-oxygenase 2, a putative mediator of vessel remodeling, is expressed in the brain AVM vessels and associates with inflammation. Acta Neurochir (Wien). 2021 Jun 29. Pubmed
Catapano JS, Frisoli FA, Nguyen CL, Labib MA, Cole TS, Baranoski JF, Kim H, Spetzler RF, Lawton MT. Intermediate-grade brain arteriovenous malformations and the boundary of operability using the supplemented Spetzler-Martin grading system. J Neurosurg. 2021 Jun 25; 1-9. Pubmed
Pan P, Weinsheimer S, Cooke D, Winkler E, Abla A, Kim H, Su H. Review of treatment and therapeutic targets in brain arteriovenous malformation. J Cereb Blood Flow Metab. 2021 Jun 23; 271678X211026771. Pubmed
Catapano JS, Frisoli FA, Nguyen CL, Wilkinson DA, Majmundar N, Cole TS, Baranoski JF, Whiting AC, Kim H, Ducruet AF, Albuquerque FC, Cooke DL, Spetzler RF, Lawton MT. Spetzler-Martin Grade III Arteriovenous Malformations: A Multicenter Propensity-Adjusted Analysis of the Effects of Preoperative Embolization. Neurosurgery. 2021 04 15; 88(5):996-1002. Pubmed
Muster R, Ko N, Smith W, Su H, Dickey MA, Nelson J, McCulloch CE, Sneed PK, Clarke JL, Saloner DA, Eisenmenger L, Kim H, Cooke DL. Proof-of-concept single-arm trial of bevacizumab therapy for brain arteriovenous malformation. BMJ Neurol Open. 2021; 3(1):e000114. Pubmed
Yan KL, Ko NU, Hetts SW, Weinsheimer S, Abla AA, Lawton MT, Kim H. Maternal and Fetal Outcomes in Women with Brain Arteriovenous Malformation Rupture during Pregnancy. Cerebrovasc Dis. 2021 Feb 26; 1-7. Pubmed
Hart BL, Mabray MC, Morrison L, Whitehead KJ, Kim H. Systemic and CNS manifestations of inherited cerebrovascular malformations. Clin Imaging. 2021 Jan 20; 75:55-66. Pubmed
Girard R, Li Y, Stadnik A, Shenkar R, Hobson N, Romanos S, Srinath A, Moore T, Lightle R, Shkoukani A, Akers A, Carroll T, Christoforidis GA, Koenig JI, Lee C, Piedad K, Greenberg SM, Kim H, Flemming KD, Ji Y, Awad IA. A Roadmap for Developing Plasma Diagnostic and Prognostic Biomarkers of Cerebral Cavernous Angioma With Symptomatic Hemorrhage (CASH). Neurosurgery. 2021 Jan 19. Pubmed
Catapano JS, Frisoli FA, Nguyen CL, Wilkinson DA, Majmundar N, Cole TS, Baranoski JF, Whiting AC, Kim H, Ducruet AF, Albuquerque FC, Cooke DL, Spetzler RF, Lawton MT. Spetzler-Martin Grade III Arteriovenous Malformations: A Multicenter Propensity-Adjusted Analysis of the Effects of Preoperative Embolization. Neurosurgery. 2021 Jan 11.Pubmed
2020
Bakker MK, van der Spek RAA, van Rheenen W, Morel S, Bourcier R, Hostettler IC, Alg VS, van Eijk KR, Koido M, Akiyama M, Terao C, Matsuda K, Walters RG, Lin K, Li L, Millwood IY, Chen Z, Rouleau GA, Zhou S, Rannikmäe K, Sudlow CLM, Houlden H, van den Berg LH, Dina C, Naggara O, Gentric JC, Shotar E, Eugène F, Desal H, Winsvold BS, Børte S, Johnsen MB, Brumpton BM, Sandvei MS, Willer CJ, Hveem K, Zwart JA, Verschuren WMM, Friedrich CM, Hirsch S, Schilling S, Dauvillier J, Martin O, Jones GT, Bown MJ, Ko NU, Kim H, Coleman JRI, Breen G, Zaroff JG, Klijn CJM, Malik R, Dichgans M, Sargurupremraj M, Tatlisumak T, Amouyel P, Debette S, Rinkel GJE, Worrall BB, Pera J, Slowik A, Gaál-Paavola EI, Niemelä M, Jääskeläinen JE, von Und Zu Fraunberg M, Lindgren A, Broderick JP, Werring DJ, Woo D, Redon R, Bijlenga P, Kamatani Y, Veldink JH, Ruigrok. Genome-wide association study of intracranial aneurysms identifies 17 risk loci and genetic overlap with clinical risk factors. Nat Genet. 2020 Dec; 52(12):1303-1313. Pubmed
Copelan A, Drocton G, Caton MT, Smith ER, Cooke DL, Nelson J, Abla AA, Fox C, Amans MR, Dowd CF, Halbach VV, Higashida RT, Lawton MT, Kim H, Fullerton HJ, Gupta N, Hetts. Brain Arteriovenous Malformation Recurrence After Apparent Microsurgical Cure: Increased Risk in Children Who Present With Arteriovenous Malformation Rupture. Stroke. 2020 10; 51(10):2990-2996. Pubmed
Mohr JP, Overbey JR, Hartmann A, Kummer RV, Al-Shahi Salman R, Kim H, van der Worp HB, Parides MK, Stefani MA, Houdart E, Libman R, Pile-Spellman J, Harkness K, Cordonnier C, Moquete E, Biondi A, Klijn CJM, Stapf C, Moskowitz AJ. Medical management with interventional therapy versus medical management alone for unruptured brain arteriovenous malformations (ARUBA): final follow-up of a multicentre, non-blinded, randomised controlled trial. Lancet Neurol. 2020 07; 19(7):573-581 Pubmed
Ayushi Gautam, Zhengda Sun, Ethan Winkler, Hua Su, Tim McCalmont, Helen Kim, Tarik Tihan, William Y. Hoffman, Chris F. Dowd, Ilona J. Frieden, Daniel L. Cooke. Concurrent Presentation of Brain Arteriovenous Malformation, Peripheral Arteriovenous Malformation, and Cerebellar Astrocytoma: Case report. Interdisciplinary Neurosurgery. Interdisciplinary Neurosurgery. 2020 Jun 1; 20:100689. Publisher site
Winkler EA, Lu A, Morshed RA, Yue JK, Rutledge WC, Burkhardt JK, Patel AB, Ammanuel SG, Braunstein S, Fox CK, Fullerton HJ, Kim H, Cooke D, Hetts SW, Lawton MT, Abla AA, Gupta N.Bringing high-grade arteriovenous malformations under control: clinical outcomes following multimodality treatment in children. J Neurosurg Pediatr. 2020 Apr 10; 1-10. PubMed
Morshed RA, Winkler EA, Kim H, Braunstein S, Cooke DL, Hetts SW, Abla AA, Fullerton HJ, Gupta N. High-Flow Vascular Malformations in Children. Semin Neurol. 2020 06; 40(3):303-314. PubMed
Rutledge C, Nelson J, Lu A, Nisson P, Jonzzon S, Winkler EA, Cooke D, Abla AA, Lawton MT, Kim H. Cost determinants in management of brain arteriovenous malformations. Acta Neurochir (Wien). 2020 01; 162(1):169-173. PubMed
2019
Rylova A, Maze M: Protecting the Brain With Xenon Anesthesia for Neurosurgical Procedures. J Neurosurg Anesthesiol, 31:18-29, 2019. PubMed
Li Z, M. W, H. L, K. H, L. W, M. Z, H. S: Fracture shortly before stroke in mice leads to hippocampus inflammation and long-lasting memory dysfunction. J Cereb Blood Flow Metab, 271678X19825785, 2019. (Epub ahead of print)
Donzelli G, Nelson J, McCoy D, McCulloch C, Hetts S, Amans M, Dowd C, Halbach V, Higashida R, Lawton M, Kim H, Cooke D: The effect of preoperative embolization and flow dynamics on surgical resection of brain arteriovenous malformations. J Neurosurg, 2019. (in press)
An Q, Chen Z, Huo K, Su H, Qu QM: Risk factors for ischemic stroke post bone fracture. J Neurosurg Anesthesiol, 31:18-29, 2019. PubMed
2018
Burkhardt JK, Chen X, Winkler E, Weiss M, Yue J, Cooke DL, Kim H, Lawton MT: Early Hemodynamic Changes Based on Initial Color-Coding Angiography as a Predictor for Developing Subsequent Symptomatic Vasospasm After Aneurysmal Subarachnoid Hemorrhage. AJNR Am J Neuroradiol, 109:e363-e373, 2018 PubMed
Coburn M, Sanders RD, Maze M, Nguyen-Pascal M, Rex S, Garriques B, Carbonell J, Garcia-Perez M, Stevanovic A, Kienbaum P, Neukirchen M, Schaefer M, Borghi B, van Oven H, Tognu' A, Al tmimi L, Eyrolle L, Iangeron O, Capdevila X, Arnold G, Rossaint R. The hip fracture surgery in elderly patients (HIPELD) study to evaluate xenon anaesthesia for the prevention of postoperative delirium: a multicentre, randomized clinical trial. Br J Anaesth, 120:127-137, 2018. PubMed
Cooke DL, McCoy DB, Halbach VV, Hetts SW, Amans MR, Dowd CF, Higashida RT, Lawson D, Nelson J, Wang CY, Kim H, Werb Z, McCulloch CE, Hashimoto T, Su H, Sun Z: Endovascular biopsy: in vivo cerebral aneurysm endothelial cell sampling and gene expression analysis. Transl Stroke Res , 2018 PubMed
Hu J, Feng X, Valdearcos M, Lutrin D, Uchida Y, Koliwad S, Maze M. Interleukin 6 is both necessary and sufficient to produce postoperative cognitive decline in mice. Br J Anaesth. 2018 Mar 2018; 120(3):537-545.
Hu J, Vacas S, Feng X, Lutrin D, Uchida Y, Lai I, Maze M. Dexmedetomidine Prevents Cognitive Decline by Enhancing Resolution of High Mobility Group Box 1 Protein-induced Inflammation through a Vagomimetic Action in Mice. Anesthesiology. 2018 May 2018; 128(5):921-931. PubMed
LaHue S, Kim H, Pawlikowska L, Nelson J, Cooke D, Hetts S, Singh V. Frequency and characteristics associated with inherited thrombophilia in patients with intracranial dural arteriovenous fistula. J Neurosurg. 2018 Apr 6:1-5. (Epub ahead of print) PMCID: PMCID: 6173991 PubMed
Lew V, McKay E, Maze M. Past, Present, and Future of Nitrous Oxide. Br Med Bull. 125:103-119, 2018 . PubMed
Lubbock-Nisson P. The Unique Features and Outcomes of Microsurgically Resected Cerebellar Arteriovenous Malformations. World Neurosurg. 2018 Sept 3; S1878-8750(18):31977-31976. (Epub ahead of print)
Maze M, Laitio T. Xenon Limits Brain Damage following Cardiac Arrest. ICU Management & Practice. 2018. (In preparation)
Meybodi AT, Kim H, Nelson J, Hetts SW, Krings T, terBrugge KG, Faughnan ME, Lawton MT, Brain Vascular Malformation Consortium HHTIG. Surgical Treatment vs Nonsurgical Treatment for Brain Arteriovenous Malformations in Patients with Hereditary Hemorrhagic Telangiectasia: A Retrospective Multicenter Consortium Study. Neurosurgery. 2018 PubMed
Nelson J, Bendjilali N, Weinsheimer S, McCulloch C, Ko N, Zaroff J, Lawton M, Pawlikowska L, Kim H. Does Intracerebral Hemorrhage in Brain Arteriovenous Malformation Share Genetic Risk Factors With Primary Intracerebral Hemorrhage?[Abstract]. . Stroke 2018 Aug 1. (In press)
Polster SP, Cao Y, Carroll T, Flemming K, Girard R, Hanley D, Hobson N, Kim H, Koenig J, Koskimaki J, Lane K, Majersik JJ, McBee N, Morrison L, Shenkar R, Stadnik A, Thompson RE, Zabramski J, Zeineddine HA, Awad IA. Trial Readiness in Cavernous Angiomas With Symptomatic Hemorrhage (CASH). Neurosurgery. 2018 PubMed
Robel R, Caroccio P, Maze M. Methods for Defining the Neuroprotective Properties of Xenon. Methods Enzymol. 2018; 602:273-288. PubMed
Saxena S, Maze M. Impact on the brain of the inflammatory response to surgery. Presse Med. 2018; 47(4 Pt. 2):e73-e81. PubMed
Saxena S, Uchida Y, Maze M. Restoring Order to Postoperative Neurocognitive Disorders. JAMA: the journal of the American Medical Association. 2018; 75(5):535-536. PubMed
Tayebi Meybodi A, Kim H, Nelson J, Hetts S, Krings T, terBrugge K, Faughnan ME, Lawton MT. Surgical treatment versus non-surgical treatment for brain arteriovenous malformation in patients with hereditary hemorrhagic telangiectasia: a retrospective multicenter consortium study. Neurosurgery. 2018.PubMed
Winkler EA, Birk H, Burkhardt JK, Chen X, Yue JK, Guo D, Rutledge WC, Lasker GF, Partow C, Tihan T, Chang EF, Su H, Kim H, Walcott BP, Lawton MT: Reductions in brain pericytes are associated with arteriovenous malformation vascular instability. World Neurosurg, 116:e1015-e1022, 2018. NIHMSID #978222 PubMed
Tang AT, Goddard LM, Hong CC, Sullivan KR, Mahadevan A, Pardo H, Peiper A, Tanes C, Mattei L, Yang J, Li L, Mericko1 PM, Hobson N, Girard R, Lightle R, Moore T, Shenkar R, Shen L, Zhou N, Whitehead KJ, Zheng X, Akers A, Morrison L, Kim H, Bittinger K, Lengner CJ, Schwaninger M, Velcich A, Augenlicht L, Min W, Marchuk DA, Awad IA, Kahn ML: Distinct cellular roles for PDCD10 define a gut-brain disease axis in cerebral cavernous malformation. Nature 2018. (submitted)
Sun Z, Wang CY, Lawson DA, Kwek S, Velozo HG, Owyong M, Lai MD, Fong L, Wilson M, Su H, Werb Z, Cooke DL: Single-cell RNA sequencing reveals gene expression signatures of breast cancer-associated endothelial cells. Oncotarget, 9:10945-10961, 2018. PMCID: PMC5834272 PubMed
Wu CX, Ma L, Chen X, Chen X, Chen Y, Zhao Y, Hess C, Kim H, Jin W, MA J. Evaluation of Angioarchitectural Features of Unruptured Brain Arteriovenous Malformation by Susceptibility Weighted Image (SWI). World Neurosurg. 2018 Aug 2018; 116:e1015-e1022. NIHMSID #978222 PubMed
Zhang DF, Su X, Meng ZT, Li HL, Wang DX, Li XY, Maze M, Ma D. Impact of Dexmedetomidine on Long-term Outcomes After Noncardiac Surgery in Elderly: 3-Year Follow-up of a Randomized Controlled Trial. Ann Surg. 2018. (Epub ahead of print) Pubmed
Zhang M, Deng Y, Zhang J, Liu J, Li Y, Su H, Qu Q. SIRT3 Protects Rotenone-induced Injury in SH-SY5Y Cells by Promoting Autophagy through the LKB1-AMPK-mTOR Pathway. Aging and Disease. 2018 Apr 1;9(2):273-286. (Epub ahead of print)
Zhu W, Chen W, Zou D, Wang L, Bao C, Zhan L, Saw D, Wang S, Winkler E, Li Z, Li ZZ, M., Shen F, Shaligram S, Lawton M, Su H. Thalidomide Reduces Hemorrhage of Brain Arteriovenous Malformations in a Mouse Model. Stroke. 2018 May 2018; 49(5):1232-1240. PMC
Zhu W, Saw D, Weiss M, Sun Z, Wei M, Shaligram S, Wang S, Su H. Induction of Brain Arteriovenous Malformation through CRISPR/Cas9 Mediated Somatic Alk1 Gene Mutations in Adult Mice. Transl Stroke Res, 2018. (Epub ahead of print) PubMed
Zhu W, Zhang R, Ma L, Su H. Animal Models and Prospective Therapeutic Targets for Brain Arteriovenous Malformation. In: Su H, Lawton M, editors. Molecular, Genetic, and Cellular Advances in Cerebrovascular Diseases. World Scientific Publishing Co.; 2018. p. 83-126.
Yu J, Nicholson A, Nelson J, Alexander M, Tse S, Hetts S, Hemphill C, Kim H, Cooke D: Predictors of Intracranial Hemorrhage Volume and Distribution in Brain Arteriovenous Malformation. Interv Neuroradiol, 2018 PubMed
Nisson PL, Fard SA, Meybodi AT, Mooney MA, Kim H, Jahnke H, Walter CM, Dumont TM, Lemole GM, Jr., Lawton MT, Spetzler RF: The Unique Features and Outcomes of Microsurgically Resected Cerebellar Arteriovenous Malformations. World Neurosurg, 120:e940-e949, 2018. PubMed
Nisson P, Walter C, Meybodi AT, Kim H, Lemole M, Lawton M: A Novel Proposed Grading System for Cerebellar Arteriovenous Malformations. J Neurosurg, 2018. (submitted)
Mascitelli JR, Yoon S, Cole TS, Kim H, Lawton MT: Does eloquence subtype influence outcome following arteriovenous malformation surgery? J Neurosurg, 1-8, 2018. (Epub ahead of print) PubMed
Ma L, Cheng P, Shaligram S, Walker EJ, Yang S-T, Tang C, Zhu W, Li Q, Zhu X, Su H: Elevation of VEGF Exacerbates Hemorrhage in Mouse Brain Arteriovenous Malformation. J Neurosurg 2018. (in press)
Burkhardt JK, Lasker GF, Winkler EA, Kim H, Lawton MT: Microsurgical resection of brain arteriovenous malformations in the elderly: outcomes analysis and risk stratification. J Neurosurg, 129:1107-1113, 2018. PubMed
Alexander MD, Hippe DS, Cooke DL, Hallam DK, Hetts SW, Kim H, Lawton MT, Sekhar LN, Kim LJ, Ghodke BV: Targeted Embolization of Aneurysms Associated With Brain Arteriovenous Malformations at High Risk for Surgical Resection: A Case-Control Study. Neurosurgery, 82:343-349, 2018. PMCID: PMC5640504 PubMed
2017
Akers A, Al-Shahi Salman R, Awad IA, Dahlem K, Flemming K, Hart B, Kim H, Jusue-Torres I, Kondziolka D, Lee C, Morrison L, Rigamonti D, Rebeiz T, Tournier-Lasserve E, Waggoner D, Whitehead K. Synopsis of guidelines for the clinical management of cerebral cavernous malformations: Consensus recommendations based on systematic literature review by the Angioma Alliance Scientific Advisory Board Clinical Experts Panel. Neurosurgery. 2017 May 1;80(5):665-680.PubMed
Arola O, Saraste A, Laitio R, Airaksinen J, Hynninen M, Bäcklund M, Ylikoski E, Wennervirta J, Pietilä M, Roine RO, Harjola VP, Niiranen J, Korpi K, Varpula M, Scheinin H, Maze M, Vahlberg T, Laitio T, Group. X-HS. Inhaled Xenon Attenuates Myocardial Damage in Comatose Survivors of Out-of-Hospital Cardiac Arrest: The Xe-Hypotheca Trial. JACC. 2017 Nov 28;70(21):2652-2660.PubMed
Mohr JP, Overbey JR, von Kummer R, Stefani MA, Libman R, Stapf C, Parides MK, Pile-Spellman J, Moquete E, Moy CS, Vicaut E, Moskowitz AJ, Harkness K, Cordonnier C, Biondi A, Houdart E, Berkefeld J, Klijn CJ, Barreau X, Kim H, Hartmann A: Functional impairments for outcomes in a randomized trial of unruptured brain AVMs. Neurology, 89:1499-1506, 2017 PubMed
Sanders RD, Andropoulos D, Ma D, Maze M. Theseus, the Labyrinth, and the Minotaur of anaesthetic-induced developmental neurotoxicity. Br J Anaesth. 2017 Sep 1;119(3):453-455. PubMed
Saparia T, Faughnan ME, Schneider JL, Almers LM, Chow N, Grosse SD, Kim H, Zaroff JG. Collaborative project to detect hereditary hemorrhagic telangiectasia in a community-based patient population. Orphanet J Rare Dis. 2017. (submitted)
Shao Q, Vacas S, Ning H, Feng X, Uchida Y, Lutrin D, Brazina S, Marcucio R, Walter P, Maze M. Inhibiting integrated stress response prevents postoperative cognitive decline. Proc Nat Acad Sci USA. 2017. (submitted)
Shen F, Jiang L, Han F, Degos V, Chen S, Su H. Increased inflammatory response in aged mice is associated with more severe neuronal injury at the acute stage of ischemic stroke. Aging and Disease. 2017.
Su H. Inflammation and genetic factors in stroke pathogenesis. Neuroimmunol Neuroinflammation. 2017 2017;4:260-262. PubMed
Sun Z, Wang CY, Lawson DA, Kwek S, Velozo HG, Owyong M, Lai MD, Fong L, Wilson M, Su H, Werb Z, Cooke D. Single-cell RNA sequencing reveals gene expression signatures of breast cancer-associated endothelial cells. Oncotarget. 2017 Dec 29;9(13):10945-10961.PubMed
Ma L, Kim H, Chen XL, Wu CX, Ma J, Su H, Zhao YL. Morbidity after hemorrhage in children with untreated brain arteriovenous malformation. Cerebrovasc Dis. 2017 Feb 28;43(5-6):231-241. PubMed
Lang LH, Parekh K, Tsui BY, Maze M: Perioperative management of the obese surgical patient. Br Med Bull, 124:135-155, 2017 PubMed
Hetts S, Yen A, Cooke D, Nelson J, Jolivalt P, Banaga J, Amans M, Dowd C, Higashida R, Lawton M, Kim H, Halbach V: Pial Artery Supply as an Anatomic Risk Factor for Symptomatic Ischemic Stroke in the Treatment of Intracranial Dural Arteriovenous Fistulas. AJNR Am J Neuroradiol, 38:2315-2320, 2017 PubMed
Kasthuri RS, Montifar M, Nelson J, Kim H, Lawton MT, Faughnan ME, Brain Vascular Malformation Consortium HHTIG. Prevalence and predictors of anemia in hereditary hemorrhagic telangiectasia. Am J Hematol. 2017 Jun 22. PubMed
Feng X, Uchida Y, Koch L, Britton S, Hu J, Lutrin D, Maze M: Exercise Prevents Enhanced Postoperative Neuroinflammation and Cognitive Decline and Rectifies the Gut Microbiome in a Rat Model of Metabolic Syndrome. Front Immunol, 2017 PubMed
Alexander MD, Hippe DS, Cooke DL, Hallam DK, Hetts SW, Kim H, Lawton MT, Sekhar LN, Kim LJ, Ghodke BV: Targeted embolization of aneurysms associated with brain AVMs at high risk for surgical resection: a case-control study. Neurosurgery, 2017 PubMed
Burkhardt JK, Lasker GF, Winkler E, Kim H, Lawton MT: Microsurgical resection of brain arteriovenous malformations in the elderly: outcomes analysis and risk stratification. J Neurosurg, 1-7, 2017 PubMed
Burkhardt JK, Chen X, Winkler EA, Cooke DL, Kim H, Lawton MT: Delayed venous drainage in ruptured arteriovenous malformations based on quantitative color-coded digital subtraction angiography. World Neurosurg, 104:619-627, 2017 PubMed
Kasthuri RS, Montifar M, Nelson J, Kim H, Lawton MT, Faughnan ME: Prevalence and predictors of anemia in hereditary hemorrhagic telangiectasia. Am J Hematol, 2017 [BVMC] PubMed
Zhu W, Ma L, Zhang R, Su H: The roles of Endoglin gene in cerebrovascular diseases. Neuroimmunology and Neuroinflammation, 4:199-210, 2017 PubMed
Vacas S, Degos V, Maze M: Fragmented Sleep Enhances Postoperative Neuroinflammation but Not Cognitive Dysfunction. Anes Analg , 124:270-276, 2017 PMCID: PMC5006595 PubMed
Chen X, Cooke D, Saloner D, Nelson J, Su H, Lawton MT, Hess C, Tihan T, Zhao Y, Kim H: Higher flow is present in unruptured arteriovenous malformations with silent intralesional microhemorrhages. Stroke, 48:2881-2884, 2017 PubMed
Chen W, Wang L, Zhu W, Zhang R, Zhan L, Camus M, Winkler E, Su H. Alk1 deficiency impairs mural cell recruitment during brain angiogenesis through reduction of platelet-derived growth factor B expression. 2017
Feng X, Valdearcos M, Uchida Y, Lutrin D, Koliwad SK, Maze M: Microglia mediate postoperative hippocampal neuroinflammation and cognitive decline in mice. JCI Insight, 2:e91229, 2017 PubMed
Forsberg A, Cervenka S, Fagerlun MJ, Rasmussen L, Zetterberg H, Harris HE, Stridh P, Christensson E, Granstrom A, Schening A, Dymmel K, Knave N, Terrando N, Maze M, Borg J, A. V, Varrone A, Halldin C, Blennow K, Farde L, Eriksson L. The immune response of the human brain to abdominal surgery. Ann Neurol. 2017 Apr 2017;81(4):572-582.
Goodwin J, Kim H, Nelson J, Faughnan ME. Organ vascular malformations predict mortality in Hereditary Hemorrhagic Telangiectasia. 2017. (in preparation)
Ma L, Kim H, Chen XL, Wu CX, Ma J, Su H, Zhao YL: Morbidity after hemorrhage in children with untreated brain arteriovenous malformation. Cerebrovasc Dis, 43:231-241, 2017 PubMed
Strickland CD, Eberhardt SC, Bartlett MR, Nelson J, Kim H, Morrison LA, Hart BL. Familial cerebral cavernous malformations are associated with adrenal calcifications on CT: an imaging biomarker for a hereditary cerebrovascular condition. Radiology. 2017 Mar 20. (Epub ahead of print) PubMed
Tang AT, Choi JP, Kotzin JJ, Yang Y, Hong CC, Hobson N, Girard R, Zeineddine HA, Lightle R, Moore T, Cao Y, Shenkar R, Chen M, Mericko P, Yang J, Li L, Tanes C, Kobuley D, Võsa U, Whitehead KJ, Li DY, Franke L, Hart B, Schwaninger M, Henao-Mejia J, Morrison L, Kim H, Awad IA, Zheng X, Kahn ML. Endothelial TLR4 and the gut microbiome drive cerebral cavernous malformations. Nature. 2017 May 18;545(7654):305-310. PubMed
Zhu W, Shen F, Mao L, Zhan L, Kang S, Sun Z, Nelson J, Zhang R, Zou D, McDougall CM, Lawton MT, Vu TH, Wu Z, Scaria A, Colosi P, Forsayeth J, Su H. Soluble FLT1 gene therapy alleviates brain arteriovenous malformation severity. Stroke. 2017 Mar 21. PubMed
Ma L, Kim H, Chen XL, Wu CX, Ma J, Su H, Zhao YL. Morbidity after hemorrhage in children with untreated brain arteriovenous malformation. Cerebrovasc Dis. 2017 Feb 28;43(5-6):231-241. PubMed
Alexander MD, Hippe DS, Cooke DL, Hallam DK, Hetts SW, Kim H, Lawton MT, Sekhar LN, Kim LJ, Ghodke BV. Targeted embolization of aneurysms associated with brain AVMs at high risk for surgical resection: a case-control study. Neurosurgery. 2017.PubMed
2016
Zou D, Luo M, Han Z, Zhan L, Zhu W, Kang S, Bao C, Li Z, Nelson J, Zhang R, Su H. Activation of alpha-7 nicotinic acetylcholine receptor reduces brain edema in mice with ischemic stroke and bone fracture. Mol Neurobiol. 2016 Dec 02. (Epub ahead of print) http://www.ncbi.nlm.nih.gov/pubmed/27914011
Zhang R, Han Z, Degos V, Shen F, Choi EJ, Sun Z, Kang S, Wong M, Zhu W, Zhan L, Arthur HM, Oh SP, Faughnan ME, Su H. Persistent infiltration and pro-inflammatory differentiation of monocytes cause unresolved inflammation in brain arteriovenous malformation. Angiogenesis. 2016 Oct;19(4):451-61.
PubMed abstract
Alexander MD, Cooke DL, Hallam DK, Kim H, Hetts SW, Ghodke BV. Less can be more: targeted embolization of aneurysms associated with arteriovenous malformations unsuitable for surgical resection. Interv Neuroradiol. 2016 Aug;22(4):445-51.
PubMed abstract
Wang L, Kang S, Zou D, Zhan L, Li Z, Zhu W, Su H. Bone fracture pre-ischemic stroke exacerbates ischemic cerebral injury in mice. PLoS One. 2016 Apr 18;11(4):e0153835.
PubMed abstract
Pekmezci M, Nelson J, Su H, Hess C, Lawton MT, Sonmez M, Young WL, Kim H, Tihan T. Morphometric characterization of brain arteriovenous malformations for clinical and radiological studies to identify silent intralesional microhemorrhages. Clin Neuropathol. 2016 Apr 6. 2016 May-Jun;35(3):114-121.
PubMed abstract
Alexander MD, Rebhun JM, Hetts SW, Kim AS, Nelson J, Kim H, Amans MR, Settecase F, Dowd CF, Halbach VV, Higashida RT, Cooke DL. Lesion location, stability, and pre-treatment management: factors affecting outcomes of endovascular treatment for vertebrobasilar atherosclerosis. J Neurointerv Surg. 2016 May; 8(5):466-470
PubMed abstract
Choquet H, Trapani E, Goitre L, Trabalzini L, Akers A, Fontanella M, Hart BL, Morrison LA, Pawlikowska L, Kim H, Retta SF. Cytochrome P450 and matrix metalloproteinase genetic modifiers of disease severity in Cerebral Cavernous Malformation type 1. Free Radic Biol Med. 2016 Mar; 92:100-109
PubMed abstract
Ma L, Shen F, Jun K, Bao C, Kuo R, Young WL, Nishimura SL, Su H. Integrin β8 deletion enhances vascular dysplasia and hemorrhage in the brain of adult Alk1 heterozygous mice. Transl Stroke Res. 2016 Dec;7(6):488-96.
PubMed Abstract
Alexander MD, Cooke DL, Hallam DK, Kim H, Hetts SW, Ghodke BV. Less can be more: targeted embolization of aneurysms associated with arteriovenous malformations unsuitable for surgical resection. Interv Neuroradiol. 2016 Aug;22(4):445-451.
PubMed abstract
Weinsheimer S, Bendjilali N, Nelson J, Guo DE, Zaroff JG, Sidney S, McCulloch CE, Al-Shahi Salman R, Berg JN, Koeleman BP, Simon M, Bostroem A, Fontanella M, Sturiale CL, Pola R, Puca R, Lawton MT, Young WL, Pawlikowska L, Klijn CJ, Kim H. Genome-wide association study of sporadic brain arteriovenous malformations. J Neurol Neurosurg Psychiatry. 2016 Sep;87(9):916-923.
PubMed abstract
2015
Choquet H, Pawlikowska L, Lawton MT, Kim H. Genetics of cerebral cavernous malformations: current status and future prospects. J Neurosurg Sci. 2015 Sep;59(3):211-220.
PubMed abstract
Sun Z, Lawson DA, Sinclair E, Wang CY, Lai MD, Hetts SW, Higashida RT, Dowd CF, Halbach VV, Werb Z, Su H, Cooke DL. Endovascular biopsy: strategy for analyzing gene expression profiles of individual endothelial cells obtained from human vessels. Biotechnol Rep (Amst). 2015 Sep;7:157-165.
PubMed abstract
Ma L, Guo Y, Zhao YL, Su H. The role of macrophage in the pathogenesis of brain arteriovenous malformation. Int J Hematol Res. 2015 Jan 1;1(2):52-56.
PubMed abstract
Lawton MT, Rutledge WC, Kim H, Stapf C, Whitehead KJ, Li DY, Krings T, terBrugge K, Kondziolka D, Morgan MK, Moon K, Spetzler RF. Brain arteriovenous malformations. Nat Rev Dis Prim. 2015 May 28;1:15008
PubMed abstract
Zhang R, Zhu W, Su H. Vascular integrity in the pathogenesis of brain arteriovenous malformation. 2015. Acta Neurochir Suppl. 2016;121:29-35.
PubMed abstract
Shen F, Mao L, Zhu W, Lawton MT, Pechan P, Colosi P, Wu Z, Scaria A, Su H. Inhibition of pathological brain angiogenesis through systemic delivery of AAV vector expressing soluble FLT1. Gene Ther. 2015 Nov;22(11):893-900.
PubMed abstract
Krings T, Kim H, Power S, Nelson J, Faughnan M, Young WL, TerBrugge KG. Neurovascular manifestations in hereditary hemorrhagic telangiectasia: imaging features and genotype-phenotype correlations. AJNR Am J Neuroradiol. 2015 May;36(5):863-870.
PubMed abstract
Wang L, Shi W, Su Z, Liu X, Su H, Liu J, Liu Z, Lawton MT. Endovascular treatment of severe acute basilar artery occlusion. J Clin Neurosci. 2015 Jan;22(1):195-198.
PubMed abstract
Kim H, Nelson J, Krings T, terBrugge K, McCulloch CE, Lawton MT, Young WL, Faughnan ME. Hemorrhage rates from brain arteriovenous malformation in patients with hereditary hemorrhagic telangiectasia. Stroke. 2015 May;46:1362-1364.
PubMed abstract
Abla AA, Nelson J, Kim H, Hess CP, Tihan T, Lawton MT. Silent arteriovenous malformation hemorrhage and the recognition of "unruptured" arteriovenous malformation patients who benefit from surgical intervention. Neurosurgery. 2015 May;76(5):592-600.
PubMed abstract
Abla AA, Rutledge WC, Seymour ZA, Guo D, Kim H, Gupta N, Sneed PK, Barani I, Larson D, McDermott MW, Lawton MT. A treatment paradigm for high-grade brain arteriovenous malformations: volume-staged radiosurgical downgrading followed by microsurgical resection. J Neurosurg. 2015 Feb;122(2):419-432.
PubMed abstract
Wang L, Wang X, Su H, Han Z, Yu H, Wang D, Jiang R, Liu Z, Zhang J. Recombinant human erythropoietin improves the neurofunctional recovery of rats following traumatic brain injury via an increase in circulating endothelial progenitor cells. Transl Stroke Res. 2015 Feb;6(1):50-59.
PubMed abstract
Kremer PH, Koeleman BP, Pawlikowska L, Weinsheimer S, Bendjilali N, Sidney S, Zaroff JG, Rinkel GJ, van den Berg LH, Ruigrok YM, de Kort GA, Veldink JH, Kim H, Klijn CJ. Evaluation of genetic risk loci for intracranial aneurysms in sporadic arteriovenous malformations of the brain. J Neurol Neurosurg Psychiat. 2015 May;86(5):524-529.
PubMed abstract
Pawlikowska L, Nelson J, Guo DE, McCulloch CE, Lawton MT, Young WL, Kim H, Faughnan ME. The ACVRL1 c.314-35A>G polymorphism is associated with organ vascular malformations in hereditary hemorrhagic telangiectasia patients with ENG mutations, but not in patients with ACVRL1 mutations. Am J Med Genet A. 2015 Jun;167(6):1262-1267.
PubMed abstract
Alexander MD, Cooke DL, Nelson J, Guo DE, Dowd CF, Higashida RT, Halbach VV, Lawton MT, Kim H, Hetts SW. Association between venous angioarchitectural features of sporadic brain arteriovenous malformations and intracranial hemorrhage. AJNR Am J Neuroradiol. 2015 May;36(5):949-952.
PubMed abstract
Golden MJ, Morrison LA, Kim H, Hart BL. Increased number of white matter lesions in patients with familial cerebral cavernous malformations. AJNR Am J Neuroradiol. 2015 May;36(5):899-903.
PubMed abstract
Kim H, Abla AA, Nelson J, McCulloch CE, Bervini D, Morgan MK, Stapleton C, Walcott BP, Ogilvy CS, Spetzler RF, Lawton MT. Validation of the supplemented Spetzler-Martin grading system for brain arteriovenous malformations in a multicenter cohort of 1009 surgical patients. Neurosurgery. 2015 Jan;76(1):25-33.
PubMed abstract
Potts MB, Lau D, Abla A, Kim H, Young WL, Lawton MT. Current surgical results with low-grade brain arteriovenous malformations. J Neurosurg. 2015 Apr;122(4):912-920.
PubMed abstract
Cooke DL, Bauer D, Sun Z, Stillson C, Nelson J, Barry D, Hetts SW, Higashida RT, Dowd CF, Halbach VV, Su H, Saeed MM. Endovascular biopsy: Technical feasibility of novel endothelial cell harvesting devices assessed in a rabbit aneurysm model. Interven Neuroradiol. 2015 Feb;21(1):120-128.
PubMed abstract
Han SJ, Englot DJ, Kim H, Lawton MT. Brainstem arteriovenous malformations: anatomical subtypes, assessment of "occlusion in situ" technique, and microsurgical results. J Neurosurg. 2015 Jan;122(1):107-117.
PubMed abstract
Yang ST, Rodriguez-Hernandez A, Walker EJ, Young WL, Su H, Lawton MT. Adult mouse venous hypertension model: common carotid artery to external jugular vein anastomosisn. J Vis Exp. 2015 Jan(95):e50472.
PubMed abstract
2014
Choquet H, Pawlikowska L, Nelson J, McCulloch CE, Akers A, Baca B, Khan Y, Hart B, Morrison L, Kim H. Polymorphisms in inflammatory and immune response genes associated with cerebral cavernous malformation type 1 severity. Cerebrovas Dis. 2014 Dec 3;38(6):433-440.
PubMed abstract
Latino GA, Kim H, Nelson J, Pawlikowska L, Young WL, Faughnan ME. Severity score for Hereditary Hemorrhagic Telangiectasia. Orphanet J Rare Dis. 2014 Dec 29;9:188.
PubMed abstract
Abla AA, Nelson J, Rutledge WC, Young WL, Kim H, Lawton MT. The natural history of AVM hemorrhage in the posterior fossa: comparison of hematoma volumes and neurological outcomes in patients with ruptured infra- and supratentorial AVMs. Neurosurg Focus. 2015. 2014 Sep;37(3):E6.
PubMed abstract
Guo Y, Tihan T, Lawton MT, Kim H, Young WL, Zhao Y, Su H. Distinctive distribution of lymphocytes in unruptured and previously untreated brain arterviovenous malformation. Neuroimmunol Neuroinflamm. 2014;1(3):147-152.
PubMed abstract
Rutledge WC, Abla AA, Nelson J, Halbach VV, Kim H, Lawton MT. Treatment and outcomes of ARUBA eligible patients with unruptured brain arteriovenous malformations at a single institution. Neurosurg Focus. 2014 Sep;37(3):E8.
PubMed abstract
Han Z, Li L, Wang L, Degos V, Maze M, Su H. Alpha-7 nicotinic acetylcholine receptor agonist treatment reduces neuroinflammation, oxidative stress and brain injury in mice with ischemic stroke and bone fracture. J Neurochem. 2014 Jul 10. 2014 Nov;131(4):498-508.
PubMed abstract
Sun Z, Su H, Long B, Sinclair E, Hetts SW, Higashida RT, Dowd CF, Halbach VV, Cooke DL. Endothelial cell high-enrichment from endovascular biopsy sample by laser capture microdissection and fluorescence activated cell sorting. J Biotechnol. 2014 Dec 20;192PA:34-39.
PubMed abstract
Rutledge WC, Ko NU, Lawton MT, Kim H. Hemorrhage rates and risk factors in the natural history course of brain arteriovenous malformations. Transl Stroke Res. 2014 Oct;5(5):538-542.
PubMed abstract
Kim H, Al-Shahi Salman R, McCulloch CE, Stapf C, Young WL. Untreated brain arteriovenous malformation: patient level meta-analysis of hemorrhage predictors. Neurology. 2014 Aug 12;83(7):590-597.
PubMed abstract
Shen F, Degos V, Chu PL, Han Z, Westbroek EM, Choi EJ, Marchuk D, Kim H, Lawton MT, Maze M, Young WL, Su H. Endoglin deficiency impairs stroke recovery. Stroke. 2014 Jul;45(7):2101-2106.
PubMed abstract
Potts MB, Jahangiri A, Jen M, Sneed PK, McDermott MW, Gupta N, Hetts SW, Young WL, Lawton MT. Deep arteriovenous malformations in the basal ganglia, thalamus, and insula: multimodality management, patient selection, and results. World Neurosurg. 2014 September – October; 82(3-4):386-394.
PubMed abstract
Bendjilali N, Nelson J, Weinsheimer S, Sidney S, Zaroff JG, Hetts SW, Segal M, Pawlikowska L, McCulloch CE, Young WL, Kim H. Common variants on 9p21.3 are associated with brain arteriovenous malformations with accompanying arterial aneurysms. J Neurol Neurosurg Psychiatry. 2014 Nov;85(11):1280-1283.
PubMed abstract
Chen W, Choi EJ, McDougall CM, Su H. Brain arteriovenous malformation modeling, pathogenesis and novel therapeutic targets. Transl Stroke Res. 2014 Jun;5(3):316-329.
PubMed abstract
Chen W, Sun Z, Han Z, Jun K, Camus M, Wankhede M, Mao L, Arnold T, Young WL, Su H. De novo cerebrovascular malformation in the adult mouse after endothelial Alk1 deletion and angiogenic stimulation. Stroke. 2014 Mar;45(3):900-902.
PubMed abstract
Choi EJ, Chen W, Jun K, Arthur HM, Young WL, Su H. Novel brain arteriovenous malformation mouse models for type 1 hereditary hemorrhagic telangiectasia. PLoS One. 2014;9(2):e88511.
PubMed abstract
Choquet H, Nelson J, Pawlikowska L, McCulloch CE, Akers A, Baca B, Khan Y, Hart B, Morrison L, Kim H. Association of cardiovascular risk factors with disease severity in cerebral cavernous malformations type 1 subjects with the common Hispanic mutation. Cerebrovas Dis. 2014 Jan;37(1):57-63.
PubMed abstract
Mohr JP, Parides MK, Stapf C, Moquete E, Moy CS, Overbey JR, Salman RA, Vicaut E, Young WL, Houdart E, Cordonnier C, Stefani MA, Hartmann A, von Kummer R, Biondi A, Berkefeld J, Klijn CJ, Harkness K, Libman R, Barreau X, Moskowitz AJ. Medical management with or without interventional therapy for unruptured brain arteriovenous malformations (ARUBA): a multicentre, non-blinded, randomised trial. Lancet. 2014 Feb 15;383(9917):614-621.
PubMed abstract
Chen W, Young WL, Su H. Induction of cerebrovascular malformation in the adult mouse. Methods Mol Biol. 2014;1135:309-316.
PubMed abstract
Hetts SW, Cooke DL, Nelson J, Gupta N, Fullerton H, Amans MR, Narvid JA, Moftakhar P, McSwain H, Dowd CF, Higashida RT, Halbach VV, Lawton MT, Kim H. Influence of patient age on angioarchitecture of brain arteriovenous malformations. AJNR Am J Neuroradiol. 2014 Jul;35(7):1376-1380.
PubMed abstract
Sheth SA, Potts MB, Sneed PK, Young WL, Cooke DL, Gupta N, Hetts SW. Angiographic features help predict outcome after stereotactic radiosurgery for the treatment of pediatric arteriovenous malformations. Childs Nerv Syst. 2014 Feb;30(2):241-247.
PubMed abstract
2013
Potts MB, Young WL, Lawton MT. Deep arteriovenous malformations in the basal ganglia, thalamus, and insula: microsurgical management, techniques, and results. Neurosurgery. 2013 Sep;73(3):417-429.
PubMed abstract
Cooke D, Su H, Guo Y, Guo D, Saeed MM, Hetts SW, Higashida RT, Dowd CF, Young WL, Halbach VV. Endovascular biopsy: evaluating the feasibility of harvesting endothelial cells using detachable coils. Interven Neuroradiol. 2013. (in press)
PubMed abstract
Hasan DM, Chalouhi N, Jabbour P, Magnotta VA, Kung DK, Young WL. Imaging aspirin effect on macrophages in the wall of the human cerebral aneurysms using ferumoxytol-enhanced MRI: Preliminary results. J Neuroradiol. 2013 Jul;40(3):187-191.
PubMed abstract
Bendjilali N, Kim H, Weinsheimer S, Guo D, Kwok PY, Zaroff JG, Sidney S, Lawton MT, McCulloch CE, Koeleman BP, Klijn CJ, Young WL, Pawlikowska L. A genome-wide investigation of copy number variation in patients with sporadic brain arteriovenous malformation. PLoS One. 2013 Oct;8(10):e71434.
PubMed abstract
Gabarros Canals A, Rodriguez-Hernandez A, Young WL, Lawton MT. Temporal lobe arteriovenous malformations: anatomical subtypes, surgical strategy, and outcomes. J Neurosurg. 2013 Sep;119(3):616-628.
PubMed abstract
Akers AL, Ball KL, Clancy M, Comi AM, Faughnan ME, Gopal-Srivastava R, Jacobs TP, Kim H, Krischer J, Marchuk DA, McCulloch CE, Morrison L, Moses MA, Pawlikowska L, Young WL. Brain Vascular Malformation Consortium: Overview, progress and future directions. J Rare Disorders [Internet]. 2013 Apr;1(1):1-15.
PubMed abstract
Degos V, Maze M, Vacas S, Hirsch J, Guo Y, Shen F, Jun K, van Rooijen N, Gressens P, Young WL, Su H. Bone fracture exacerbates murine ischemic cerebral injury. Anesthesiology. 2013 Jun;118(6):1362-1372.
PubMed abstract
Degos V, Westbroek EM, Lawton MT, Hemphill JC III, del Zoppo GJ, Young WL. Perioperative management of coagulation in non-traumatic intracerebral hemorrhage. Anesthesiology. 2013 2013 Jul;119(1):218-227.
PubMed abstract
Hasan D, Chalouhi N, Jabbour PM, Dumont AS, Kung D, Magnotta V, Young WL, Hashimoto T, Winn HR, Hesitad D. Evidence that acetylsalicylic acid attenuates inflammation in the wall of human cerebral aneurysms: preliminary results. J Am Heart Assoc. 2013 Feb 22;2(1):e000019.
PubMed abstract
Chen W, Guo Y, Walker EJ, Shen F, Jun K, Oh SP, Degos V, Lawton MT, Tihan T, Davalos D, Akassoglou K, Nelson J, Pile-Spellman J, Su H, Young WL. Reduced mural cell coverage and impaired vessel integrity after angiogenic stimulation in the Alk1-deficient brainn. Arterioscler Thromb Vasc Biol. 2013 Feb;33(2):305-310.
PubMed abstract
Choi EJ, Walker EJ, Degos V, Jun K, Kuo R, Su H, Young WL. Endoglin deficiency in bone marrow is sufficient to cause cerebrovascular dysplasia in the adult mouse after vascular endothelial growth factor stimulation. Stroke. 2013 Mar;44(3):795-798.
PubMed abstract
Degos V, Vacas S, Han Z, van Rooijen N, Gressens P, Su H, Young WL, Maze M. Depletion of bone marrow-derived macrophages perturbs the innate immune response to surgery and reduces postoperative memory dysfunction. Anesthesiology. 2013 Mar;118(3):527-536.
PubMed abstract
Shen F, Kuo R, Milon-Camus M, Han Z, Jang L, Young WL, Su H. Intravenous delivery of AAV9 vector mediates effective gene expression in ischemic stroke lesion and brain angiogenic foci. Stroke. 2013 Jan;44(1):252-254.
PubMed abstract
Boshuisen K, Brundel M, de Kovel CG, Letteboer TG, Rinkel GJ, Westermann CJ, Kim H, Pawlikowska L, Koeleman BP, Klijn CJ. Common polymorphisms in ACVRL1 and Endoglin genes are not associated with sporadic and HHT related brain arteriovenous malformations in Dutch patients. Transl Stroke Res. 2013 Jun;4(3):375-378.
PubMed abstract
2012
Hasan D, Chalouhi N, Jabbour P, Dumont AS, Kung DK, Magnotta VA, Young WL, Hashimoto T, Winn HR, Heistad D. Early change in ferumoxytol-enhanced magnetic resonance imaging signal suggests unstable human cerebral aneurysm. A pilot study. Stroke. 2012 Dec;43(12):3258-3265.
PubMed abstract
Rodriguez-Hernandez A, Kim H, Pourmohamad T, Young WL, Lawton MT. Cerebellar arteriovenous malformations: anatomical subtypes, surgical results, and increased predictive accurary of the supplementary grading system. Neurosurgery. 2012 Dec;71(6):1111-1124.
PubMed abstract
Nishida T, Faughnan ME, Krings T, Chakinala M, Gossage JR, Young WL, Kim H, Pourmohamad T, Henderson KJ, Schrum SD, James M, Quinnine N, Bharatha A, terBrugge KG, White RI, Jr. Brain arteriovenous malformations associated with Hereditary Hemorrhagic Telangiectasia: genotype-phenotype correlations. Am J Med Genet. 2012 Nov;158(A)(11):2829-2834.
PubMed abstract
Weinsheimer S, Brettman A, Pawlikowska L, Mancuso MR, Kuhnert F, Lawton MT, Sidney S, Zaroff JG, McCulloch CE, Young WL, Kuo C, Kim H. G protein-coupled receptor 124 (GPR124) gene polymorphisms and risk of brain arteriovenous malformation. Transl Stroke Res. 2012 Dec;3(4):418-427.
PubMed abstract
Degos V, Gourraud PA, Trehel-Tursis V, Whelan R, Colonne C, Korinek AM, Clarencon F, Boch AL, Nouet A, Young WL, Apfel CC, Puybasset L. Elderly age as a prognostic marker of 1-year poor outcome for subarachnoid hemorrhage patients through its interaction with admission hydrocephalus. Anesthesiology. 2012 Dec;117(6):1289-1299.
PubMed abstract
Kim H, Pourmohamad T, Westbroek EM, McCulloch CE, Lawton MT, Young WL. Evaluating performance of the Spetzler-Martin supplemented model in selecting patients with arteriovenous malformation patients for surgery. Stroke. 2012 Sep;43(9):2497-2499.
PubMed abstract
Englot DJ, Young WL, Han SJ, McCulloch CE, Chang EF, Lawton MT. Seizure predictors and control after microsurgical resection of supratentorial arteriovenous malformations in 440 patients. Neurosurgery. 2012 Sep;71(3):572-580.
PubMed abstract
Westbroek EM, Pawlikowska L, Lawton MT, McCulloch CE, Young WL, Kim H. Brain-derived neurotrophic factor Val66Met polymorphism predicts worse functional outcome after surgery patients with unruptured brain arteriovenous malformation. Stroke. 2012 Aug;43(8):2255-2257.
PubMed abstract
Kahle MP, Lee B, Pourmohamad T, Cunningham A, Su H, Kim H, Chen Y, McCulloch CE, Barbaro NM, Lawton MT, Young WL, Bix GJ. Perlecan domain V is upregulated in human brain arteriovenous malformation and could mediate the vascular endothelial growth factor effect in lesional tissue. NeuroReport. 2012 Jul;11;23(10):627-630.
PubMed abstract
Sapru A, Zaroff JG, Pawlikowska L, Liu KD, Khush KK, Ann-Baxter-Lowe L, Hayden V, Menza RL, Convery M, Lo V, Poon A, Kim H, Young WL, Kukreja J, Matthay MA. The 4G/4G genotype of the PAI-1 (Serpine-1) 4G/5G polymorphism is associated with decreased lung allograft utilization. Am J Transplant. 2012. Jul;12(7):1848-1854.
PubMed abstract
Wang DD, Englot DJ, Garcia PA, Chen T, Lawton MT, Young WL. Minocycline and tetracycline-class antibiotics protective against partial seizures in vivo. Epilepsy Res. 2012. Jul;43(7):1325-1330.
PubMed abstract
Walker EJ, Su H, Shen F, Degos V, Jun K, Young WL. Bevacizumab attenuates VEGF-induced angiogenesis and vascular malformations in the adult mouse brain. Stroke. 2012. Jul;43(7):1325-1330.
PubMed abstract
Hasan DM, Amans M, Tihan T, Hess C, Guo Y, Cha S, Su H, Martin AJ, Lawton MT, Neuwelt EA, Saloner DA, Young WL. Ferumoxytol-enhanced MRI to image inflammation within human brain arteriovenous malformations: a pilot investigation. Transl Stroke Res. 2012 Jul;3(Supplement 1):166-173.
PubMed abstract
Choi EJ, Walker EJ, Shen F, Oh SP, Arthur HM, Young WL, Su H. Minimal homozygous endothelial deletion of Eng with VEGF stimulation is sufficient to cause cerebrovascular dysplasia in the adult mouse. Cerebrovasc Dis 2012 Jun;33(6):540-547.
PubMed abstract
Hasan DM, Mahaney KB, Magnotta VA, Kung DK, Lawton MT, Hashimoto T, Winn HR, Saloner D, Martin A, Gahramanov S, Dosa E, Neuwelt E, Young WL. Macrophage imaging within human cerebral aneurysms wall using ferumoxytol-enhanced MRI: a pilot study. Arterioscler Thromb Vasc Biol. 2012 Apr;32(4):1032-1038.
PubMed abstract
Guo Y, Saunders T, Su H, Kim H, Akkoc D, Saloner DA, Hetts SW, Hess C, Lawton MT, Bollen AW, Pourmohamad T, McCulloch CE, Tihan T, Young WL. Silent intralesional microhemorrhage as a risk factor for brain arteriovenous malformation rupture. Stroke. 2012 May;43(5):1240-1246.
PubMed abstract
Hetts SW, Keenan K, Fullerton H, Young WL, English JD, Gupta N, Dowd CF, Higashida RT, Lawton MT, Halbach VV: Pediatric intracranial non-galenic pial arteriovenous fistulas: clinical features, angioarchitecture, and outcomes. AJNR Am J Neuroradiol. 2012 Oct;33(9):1710-1719.
PubMed abstract
Degos V, Apfel CC, Sanchez P, Colonne C, Renuit I, Clarancon F, Nouet A, Boch AL, Pourmohamad T, Kim H, Gourraud PA, Young WL, Puybasset L: An admission bio-clinical score for coiled-aneurysm to predict 1-year outcomes. Stroke. 2012. May;43(5):1253-1259.
PubMed abstract
Alexander MJ, Hetts SW, Young WL, Halbach VV, Dowd CF, Higashida RT, English JD: Supernova hemorrhage: obliterative hemorrhage of brain arteriovenous malformations following gamma knife radiosurgery. J Neurointerv Surg. 2012 Sep 1;4(5):365-367.
PubMed abstract
Potts MB, Chang EF, Young WL, Lawton MT: Transsylvian-transinsular approaches to the insula and basal ganglia: operative techniques and results with vascular lesions. Neurosurgery. 2012 Apr;70(4):824-834.
PubMed abstract
Bharatha A, Faughnan ME, Kim H, Pourmohamad T, Krings T, Bayrak-Toydemir P, Pawlikowska L, McCulloch CE, Lawton MT, Dowd CF, Young WL, Terbrugge KG: Brain arteriovenous malformation multiplicity predicts the diagnosis of hereditary hemorrhagic telangiectasia: quantitative assessment. Stroke 2012 Jan;43(1):72-78.
PubMed abstract
Davies JM, Kim H, Young WL, Lawton MT: Classification schemes for arteriovenous malformations. Neurosurg Clin N Am. 2012 Jan;23(1):43-53.
PubMed abstract
Zaroff JG, Leong J, Kim H, Young WL, Cullen SP, Rao VA, Sorel M, Quesenberry CP, Jr., Sidney S: Cardiovascular predictors of long-term outcomes after non-traumatic subarachnoid hemorrhage. Neurocrit Care. 2012. Dec;17(3):374-381.
PubMed abstract
2011
Weinsheimer S, Xu H, Achrol AS, Stamova B, McCulloch CE, Pawlikowska L, Tian Y, Ko NU, Lawton MT, Steinberg GK, Chang SD, Jickling G, Ander BP, Kim H, Sharp FR, Young WL: Gene expression profiling of blood in brain arteriovenous malformation patients. Transl Stroke Res, 2:575-587, 2011.
PubMed abstract
Sun H, Le T, Tiffany TJ, Habib A, Wu S, Shen F, Young WL, Su H, Liu J: AAV-mediated netrin-1 overexpression increases peri-infarct blood vessel density and improves motor function recovery after experimental stroke. Neurobiol Dis, 44:73-83, 2011.
PubMed abstract
Terrando N, Brzezinski M, Degos V, Eriksson LI, Kramer JH, Leung JM, Miller BL, Mucke L, Seeley WW, Vacas S, Weiner MW, Yaffe K, Young WL, Xie Z, Maze M: Perioperative cognitive decline with the aging population. Mayo Clin Proc, 86:885-893, 2011.
PubMed abstract
Shen F, Walker EJ, Jiang L, Li J, Sun B, Heriyanto F, Young WL, Su H: Co-expression of angiopoietin1 with VEGF increases the structural integrity of the blood-brain barrier and reduces atrophy volume. J Cereb Blood Flow Metab, 31:2343-2351, 2011.
PubMed abstract
Hoffmann A, Bredno J, Wendland MF, Derugin N, Hom J, Schuster T, Su H, Ohara PT, Young WL, Wintermark M: Validation of in vivo MRI blood-brain barrier permeability measurements by comparison with gold standard histology. Stroke, 42:2054-2060, 2011.
PubMed abstract
Kim H, Su H, Weinsheimer S, Pawlikowska L, Young WL: Brain arteriovenous malformation pathogenesis: a response-to-injury paradigm. Acta Neurochir Suppl, 111:83-92, 2011.)
PubMed abstract
Walker EJ, Shen F, Young WL, Su H: Cerebrovascular casting of adult mouse for 3D imaging and morphological analysis. J Vis Exp, 57:pii: 2958, 2011.
PubMed abstract
Jiang L, Shen F, Degos V, Schonemann M, Pleasure SJ, Mellon S, Young WL, Su H: Oligogenesis and oligodendrocyte progenitor maturation vary in different brain regions and partially correlate with local angiogenesis after ischemic stroke. Transl Stroke Res, 2:366-375, 2011
PubMed abstract
Taub PR, Fields JD, Wu AH, Miss JC, Lawton MT, Smith WS, Young WL, Zaroff JG, Ko NU: Elevated BNP is associated with vasospasm-independent cerebral infarction following aneurysmal subarachnoid hemorrhage. Neurocrit Care, 15:13-18, 2011.
PubMed abstract
Zhu Y, Wang A, Patel S, Kurpinski K, Diao E, Bao J, Kwong G, Young WL, Li S: Engineering bi-layer nanofibrous conduits for peripheral nerve regeneration. Tissue Eng Part C Methods, 17:705-715, 2011
PubMed abstract
Su H, Yang GY: Treatment of focal brain ischemia with viral vector-mediated gene transfer. Methods Mol Biol, 686:429-446, 2011.
PubMed abstract
Mikhak B, Weinsheimer S, Pawlikowska L, Poon A, Kwok PY, Lawton MT, Chen Y, Zaroff JG, Sidney S, McCulloch CE, Young WL, Kim H: Angiopoietin-like 4 (ANGPTL4) gene polymorphisms and risk of brain arteriovenous malformations (BAVM). Cerebrovasc Dis, 31:338-345, 2011.
PubMed abstract
Monson KL, Matsumoto MM, Young WL, Manley GT, Hashimoto T: Abrupt increase in rat carotid blood flow induces rapid alteration of artery mechanical properties. J Mech Behav Biomed Mater, 4:9-15, 2011
PubMed abstract
Hao Q, Su H, Palmer D, Sun B, Gao P, Yang GY, Young WL: Bone marrow-derived cells contribute to VEGF-induced angiogenesis in the adult mouse brain by supplying MMP-9. Stroke, 42:453-458, 2011.
PubMed abstract
Kanematsu Y, Kanematsu M, Kurihara C, Tada Y, Tsou TL, van Rooijen N, Lawton MT, Young WL, Liang EI, Nuki Y, Hashimoto T: Critical roles of macrophages in the formation of intracranial aneurysm. Stroke, 42:173-178, 2011.
PubMed abstract
Gabarros A, Young WL, McDermott MW, Lawton MT: Language and motor mapping during resection of brain arteriovenous malformations: indications, feasibility, and utility. Neurosurgery, 2011, 68:744-752, 2011.
PubMed abstract
Kim YB, Young WL, Lawton MT: Parafalcine and midline arteriovenous malformations: surgical strategy, techniques, and outcomes. J Neurosurg, 114:984-993, 2011.
PubMed abstract
Boussel L, Rayz V, Martin AJ, Lawton MT, Higashida RT, Smith WS, Young WL, Saloner D: Temporal stability of dysmorphic, fusiform aneurysms of the intra-cranial internal carotid artery. J Vasc Interv Radiol, 22:1007-1011, 2011.
PubMed abstract
Walker E, Su H, Shen F, Choi EJ, Oh SP, Chen G, Lawton MT, Kim H, Chen Y, Chen W, Young WL: Arteriovenous malformation in the adult mouse brain resembling the human disease. Ann Neurol, 69:954-962, 2011.
PubMed abstract
2010
Kuhnert F, Mancuso MR, Shamloo A, Wang HT, Choksi V, Florek M, Su H, Fruttiger M, Young WL, Heilshorn SC, Kuo CJ: Essential regulation of CNS angiogenesis by the orphan G protein-coupled receptor GPR124. Science, 330:985-989, 2010.
PubMed abstract
Logvinova A, Litt L, Young WL, Lee CZ: Anesthetic concerns in patients with known cerebrovascular insufficiency. Anesthesiol Clin, 28:1-12, 2010
PubMed abstract
Mohr JP, Moskowitz AJ, Stapf C, Hartmann A, Lord K, Marshall SM, Mast H, Moquete E, Moy CS, Parides M, Pile-Spellman J, Al-Shahi Salman R, Weinberg A, Young WL, Estevez A, Kureshi I, Brisman JL: The ARUBA trial current status, future hopes. Stroke, 41:e537-e540, 2010.
PubMed abstract
Hao Q, Zhu Y, Su H, Shen F, Yang GY, Kim H, Young WL: VEGF induces more severe cerebrovascular dysplasia in Endoglin+/- than in Alk1+/- mice. Transl Stroke Res, 1:197-201, 2010.
PubMed abstract
Delaloy C, Liu L, Lee J-A, Shen F, Su H, Yang GY, Young WL, Ivey KN, Gao FB: MicroRNA-9 coordinates proliferation and migration of human embryonic stem cell-derived neural progenitors. Cell Stem Cell, 6:323-335, 2010
PubMed abstract
Kim H, McCulloch CE, Johnston SC, Lawton MT, Sidney S, Young WL: Comparison of two approaches for determining the natural history risk of brain arteriovenous malformation rupture. Am J Epidemiol, 171:1317-1322, 2010.
PubMed abstract
Gao P, Chen Y, Lawton MT, Barbaro NM, Yang GY, Su H, Ling F, Young WL: Evidence of endothelial progenitor cells in the human brain and spinal cord arteriovenous malformations. Neurosurgery, 67:1029-1035, 2010.
PubMed abstract
Fan Y, Shen F, Frenzel T, Zhu W, Ye J, Liu J, Chen Y, Su H, Young WL, Yang GY: Endothelial progenitor cell transplantation improves long-term outcome in mice. Ann Neurol, 67:488-497, 2010.
PubMed abstract
Lawton MT, Kim H, McCulloch CE, Mikhak B, Young WL: A supplementary grading scale for selecting patients with brain arteriovenous malformations for surgery. Neurosurgery, 2010. (in press)
Gabriel RA, Kim H, Sidney S, McCulloch CE, Singh V, Johnston SC, Ko NU, Achrol AS, Zaroff JG, Young WL: Ten-year detection rate of brain arteriovenous malformations in a large, multiethnic, defined population. Stroke, 41:21-26, 2010.
PubMed abstract
Su H, Kim H, Pawlikowska L, Kitamura H, Shen F, Cambier S, Markovics J, Lawton MT, Sidney S, Bollen AW, Kwok PY, Reichardt L, Young WL, Yang GY, Nishimura SL: Reduced expression of integrin {alpha}v{beta}8 is associated with brain arteriovenous malformation pathogenesis. Am J Pathol, 176:1018-1027, 2010.
PubMed abstract
2009
Potter CA, Armstrong-Wells J, Fullerton HJ, Young WL, Higashida RT, Dowd CF, Halbach VV, Hetts SW: Neonatal giant pial arteriovenous malformation: genesis or rapid enlargement in the third trimester. J NeuroIntervent Surg, 1:151-153, 2009.
PubMed abstract
Liu J, Segal M, Yoo S, Yang GY, Kelly M, James TL, Litt L: Antioxydant effect of ethyl pyruvate in respiring neonatal cerebrocortical slices after H(2)O(2) stress. Neurochemistry Int,54:106-110, 2009
PubMed abstract
ZhuGe Q, Zhou M, Zheng W, Yang GY, Mao X, Xie L, Gourong C, Chen Y, Lawton MT, Young WL, Greenberg DA, Jin K: Notch1 signaling is activated in brain arteriovenous malformation in humans. Brain, 132:3231-3241, 2009.
PubMed abstract
Leblanc GG, Golanov E, Awad IA, Young WL: Biology of vascular malformations of the brain. Stroke, 40:e694-e702, 2009.
PubMed abstract
Weinsheimer S, Kim H, Pawlikowska L, Chen Y, Lawton MT, Sidney S, Kwok PY, McCulloch CE, Young WL: Ephrin receptor B4 (EPHB4) gene polymorphisms and risk of intracranial hemorrhage in patients with brain arteriovenous malformations. Circ Cardiovasc Genet, 2:476-482, 2009.
PubMed abstract
Gao P, Shen F, Gabriel RA, Law D, Yang E, Yang GY, Young WL, Su H: Attenuation of brain response to VEGF-mediated angiogenesis and neurogenesis in aged mice. Stroke, 40:3596-3600, 2009.
PubMed abstract
Ota R, Kurihara C, Tsou TL, Young WL, Yeghiazarians Y, Chang M, Mobashery S, Sakamoto A, Hashimoto T: Roles of matrix metalloproteinases in flow-induced outward vascular remodeling. J Cereb Blood Flow Metab, 29:1547-1558, 2009.
PubMed abstract
Zhu W, Fan Y, Hao Q, Shen F, Hashimoto T, Yang GY, Gasmi M, Bartus RT, Young WL, Chen Y: Post-ischemic IGF-1 gene transfer promotes neurovascular regeneration after experimental stroke. J Cereb Blood Flow Metab, 29:1528-1537, 2009.
PubMed abstract
Gao P, Zhu Y, Ling F, Shen F, Lee B, Gabriel RA, Hao Q, Yang GY, Su H, Young WL: Nonischemic cerebral venous hypertension promotes a pro-angiogenic state through HIF-1 downstream genes and leukocyte-derived MMP-9. J Cereb Blood Flow Metab, 29:1482-1490, 2009.
PubMed abstract
Sanchez-Mejia RO, McDermott MW, Tan J, Kim H, Young WL, Lawton MT: Radiosurgery facilitates resection of brain arteriovenous malformations and reduces surgical morbidity. Neurosurgery, 64:231-238, 2009
PubMed abstract
Lee CZ, Xue Z, Hao Q, Yang GY, Young WL: Nitric oxide in vascular endothelial growth factor-induced focal angiogenesis and matrix metalloproteinase-9 activity in the mouse brain. Stroke, 40:2879-2881, 2009.
PubMed abstract
Chen Y, Hao Q, Kim H, Su H, Letarte M, Karumanchi SA, Lawton MT, Barbaro NM, Yang GY, Young WL: Soluble endoglin modulates aberrant cerebral vascular remodeling. Ann Neurol, 66:19-27, 2009.
PubMed abstract
Zhu Y, Cuevas IC, Gabriel RA, Su H, Nishimura S, Gao P, Fields A, Hao Q, Young WL, Yang GY, Boudreau NJ: Restoring HoxA5 expression inhibits the growth of experimental hemangiomas in the brain. J Neuropathol Exp Neurol, 68:626-632, 2009.
PubMed abstract
Boussel L, Rayz V, Martin AJ, Acevedo-Bolton G, Lawton MT, Higashida RT, Smith WS, Young WL, Saloner D: Phase-contrast magnetic resonance imaging measurements in intracranial aneurysms in vivo of flow patterns, velocity fields, and wall shear stress: comparison with computational fluid dynamics. Magn Reson Med., 61:409-417, 2009
PubMed abstract
Kim H, Hysi PG, Pawlikowska L, Poon A, Burchard EG, Zaroff JG, Sidney S, Ko NU, Achrol AS, Lawton MT, McCulloch CE, Kwok PY, Young WL: Common variants in interleukin-1-beta gene are associated with intracranial hemorrhage and susceptibility to brain arteriovenous malformation. J Cerebrovasc Dis, 27:176-182, 2009
PubMed abstract
Nuki Y, Matsumoto MM, Tsang E, Young WL, van Rooijen N, Kurihara C, Hashimoto T: Roles of macrophages in flow-induced outward vascular remodeling. J Cereb Blood Flow Metab, 29:495-503, 2009
PubMed abstract
Kim H, Pawlikowska L, Chen Y, Su H, Yang GY, Young WL: Brain arteriovenous malformation biology relevant to hemorrhage and implication for therapeutic development. Stroke, 40[suppl 1]:S95-S97, 2009
PubMed abstract
2008
Hao Q, Su H, Marchuk DA, Rola R, Wang Y, Liu W, Young WL, Yang GY: Increased tissue perfusion promotes capillary dysplasia in the ALK1-deficient mouse brain following VEGF stimulation. Am J Physiol Heart Circ Physiol, 295:H2250-H2256, 2008
PubMed abstract
Hao Q, Liu J, Pappu R, Su H, Rola R, Gabriel RA, Young WL, Yang GY: The contribution of bone marrow-derived cells associated with brain angiogenesis is primarily through leukocytes and macrophages. Arterioscler Thromb Vasc Biol, 28:2151-2157, 2008.
PubMed abstract
Rayz VL, Boussel L, Lawton MT, Acevedo-Bolton G, Ge L, Young W, Higashida RT, Saloner D: Numerical modeling of the flow in intracranial aneurysms: prediction of regions prone to thrombus formation. Ann Biomed Eng, 36:1793-1804, 2008.
PubMed abstract
Rayz VL, Boussel L, Acevedo-Bolton G, Martin AJ, Young WL, Lawton MT, Higashida R, Saloner D: Numerical simulations of flow in cerebral aneurysms: comparison of CFD results and in vivo MRI measurements. J Biomech Eng, 130:051011, 2008
PubMed abstract
Kim H, Hysi PG, Pawlikowska L, Choudhry S, Burchard EG, Kwok PY, Sidney S, McCulloch CE, Young WL: Population stratification in a case control study of brain arteriovenous malformation (BAVM) in Latinos. Neuroepidemiology, 31:224-228, 2008
PubMed abstract
Lawton MT, Arnold CM, Kim YJ, Bogarin EA, Stewart CL, Wulfstat AA, Derugin N, Deen D, Young WL: Radiation arteriopathy in the transgenic arteriovenous fistula model. Neurosurgery, 62:1129-1138
PubMed abstract
Fan Y, Zhu W, Yang M, Zhu Y, Shen F, Hao Q, Young WL, Yang GY, Chen Y: Del-1 gene transfer induces cerebral angiogenesis in mice. Brain Res, 1219:1-7, 2008
PubMed abstract
Su H, Hao Q, Shen F, Zhu Y, Lee CZ, Young WL, Yang GY: Development of cerebral microvascular dysplasia model in rodents. Acta Neurochir Suppl, 105:185-189, 2008.
PubMed abstract
Boussel L, Rayz V, McCulloch CE, Martin A, Acevedo-Bolton G, Lawton M, Higashida R, Smith WS, Young WL, Saloner D: Aneurysm growth occurs at region of low wall shear stress: patient-specific correlation of hemodynamics and growth in a longitudinal study. Stroke, 39:2997-3002, 2008
PubMed abstract
Kim H, Marchuk DA, Chen Y, Su H, Yang GY, Young WL: Genetic considerations relevant to intracranial hemorrhage and brain arteriovenous malformations. Acta Neurochir Suppl, 105:199-206, 2008.
PubMed abstract
Fan Y, Shen F, Hao Q, Chen Y, Liu W, Su H, Young WL, Yang GY: Overexpression of Netrin-1 induces neovascularization in the adult mouse brain. J Cereb Blood Flow Metab, 28:1543-1551, 2008
PubMed abstract
Singh V, Smith WS, Lawton MT, Halbach VV, Young WL: Risk factors for hemorrhagic presentation in patients with dural arteriovenous fistulae. Neurosurgery, 62:628-635; discussion 628-635, 2008
PubMed abstract
Chen Y, Zhu W, Bollen AW, Lawton MT, Barbaro NM, Dowd CF, Hashimoto T, Yang GY, Young WL: Evidence for inflammatory cell involvement in brain arteriovenous malformations. Neurosurgery, 62:1340-1349; discussion 1349-1350, 2008, 2008
PubMed abstract
Zhu W, Khachi S, Hao Q, Shen F, Young WL, Yang GY, Chen Y: Upregulation of EMMPRIN after permanent focal cerebral ischemia. Neurochem Int, 52:1086-91, 2008
PubMed abstract
Shen F, Fan Y, SU H, Zhu Y, Chen Y, Liu W, Young WL, Yang GY: Adeno-associated viral vector-mediated hypoxia-regulated VEGF factor gene transfer promotes angiogenesis following focal cerebral ischemia in mice. Gene Ther, 15:30-39, 2008
PubMed abstract
Fan Y, Ye J, Shen F, Zhu W, Zhu Y, Yeghiazarians Y, Chen Y, Lawton MT, Young WL, Yang GY: Interleukin-6 stimulates circulating blood-derived endothelial progenitor cell angiogenesis in vitro. J Cereb Blood Flow Metab, 28:90-98, 2008
PubMed abstract
Zhu W, Fan Y, Frenzel T, Gasmi M, Bartus RT, Young WL, Yang GY, Chen Y: IGF-1 gene transfer enhances neurovascular remodeling and improves long-term stroke outcome in mice. Stroke, 39:1254-61, 2008
PubMed abstract
Ko NU, Rajendran P, Kim H, Rutkowski M, Pawlikowska L, Kwok PY, Higashida RT, Lawton MT, Smith WS, Zaroff JG, Young WL: Endothelial nitric oxide synthase polymorphisms (-786T>C) and increased risk of angiographic vasospasm after aneurysmal subarachnoid hemorrhage. Stroke, 39:1103-8, 2008
PubMed abstract
Zhu W, Tian Y, Zhou LF, Wang Y, Song D, Mao Y, Yang GY: Development of a novel endothelial cell-seeded endovascular stent for intracranial aneurysm therapy. J Biomed Mater Res A, 85:715-721, 2008
PubMed abstract
Rayz VL, Lawton MT, Martin AJ, Young WL, Saloner D: Numerical simulation of pre- and post-surgical flow in a giant basilar aneurysm. J Biomech Eng., 130:021004, 2008
PubMed abstract
Boussel L, Wintermark M, Martin AJ, Dispensa B, VanTijen R, Leach J, Rayz V, Acevedo-Bolton G, Lawton MT, Higashida RT, Smith WS, Young WL, Saloner D: Monitoring serial change in the lumen and outer wall of vertebro-basilar aneurysms. AJNR Am J Neuroradiol, 29:259-64, 2008
PubMed abstract
Frenzel T, Lee CZ, Kim H, Quinnine N, Hashimoto T, Lawton MT, Guglielmo BJ, McCulloch CE, Young WL: Feasibility of minocycline and doxycycline use as potential vasculostatic therapy for brain vascular malformations: pilot study of adverse events and tolerance. Cerebrovasc Dis, 25:157-163, 2008
PubMed abstract
2007
Zeng J, Liu J, Yang GY, Kelly MJ, James TL, Litt L: Exogenous ethyl pyruvate versus pyruvate during metabolic recovery after oxidative stress in neonatal rat cerebrocortical slices. Anesthesiology,107:630-640, 2007.
PubMed abstract
Gabriel RA, Yang GY: Gene therapy in cerebrovascular diseases. Curr Gene Ther, 7:421-33, 2007
PubMed abstract
Achrol AS, Kim H, Pawlikowska L, Poon KYT, Ko NU, McCulloch CE, Zaroff JG, Johnston SC, McDermott MW, Lawton MT, Kwok PY, Young WL: Association of tumor necrosis factor-alpha-238G>A and apolipoprotein E2 polymorphisms with intracranial hemorrhage after brain arteriovenous malformation treatment. Neurosurgery, 2007, 61:731-9; discussion 740, 2007
PubMed abstract
Hashi CK, Zhu Y, Yang GY, Young WL, Hsiao BS, Wang K, Chu B, Li S: Antithrombogenic property of bone marrow mesenchymal stem cells in nanofibrous vascular grafts. Proc Natl Acad Sci USA, 104:11915-20, 2007
PubMed abstract
Kim H, Sidney S, McCulloch CE, Poon KYT, Singh V, Johnston SC, Ko NU, Achrol AS, Lawton MT, Higashida RT, Young WL: Racial/ethnic differences in longitudinal risk of intracranial hemorrhage in brain arteriovenous malformation patients. Stroke, 38:2430-37, 2007
PubMed abstract
Lawton MT, Lu DC, Young WL: Sylvian fissure arteriovenous malformations: an application of the Sugita classification to 28 surgical patients. Neurosurgery 61:29-38, 2007
PubMed abstract
Lee CZ, Xue Z, Zhu Y, Yang GY, Young WL: Matrix metalloproteinase-9 inhibition attenuates vascular endothelial growth factor-induced intracranial hemorrhage. Stroke, 38:2563-68, 2007
PubMed abstract
Du R, Hashimoto T, Tihan T, Young WL, Perry V, Lawton MT: Growth and regression of an arteriovenous malformation in a patient with hereditary hemorrhagic telangiectasia: case report. J Neurosurg 106:470-7, 2007.
PubMed abstract
Yao JS, Fan Y, Zhai W, Lawton MT, Barbaro NM, Young WL, Yang G-Y: Interleukin-6 upregulates expression of KDR and stimulates proliferation of human cerebrovascular smooth muscle cells. J Cereb Blood Flow Metab 27:510-20, 2007.
PubMed abstract
Yao JS, Shen F, Young WL, Yang G-Y: Comparison of doxycycline and minocycline in the inhibition of VEGF-induced smooth muscle cell migration. Neurochem Int 50:524-530, 2007.
PubMed abstract
Hao Q, Chen Y, Zhu Y, Fan Y, Young WL, Yang GY: Neutrophil depletion decreases VEGF-induced focal angiogenesis in the mature mouse brain. J Cereb Blood Flow Metab , 27:1853-60, 2007
PubMed abstract
Du R, Keyoung HM, Dowd CF, Young WL, Lawton MT: The effects of diffuseness and deep perforating artery supply on outcomes after microsurgical resection of brain arteriovenous malformations. Neurosurgery 60:638-46, 2007.
PubMed abstract
Dispensa BP, Saloner DA, Acevedo-Bolton G, Achrol, AS, Jou L-D, McCulloch CE, Higashida RT, Dowd CF, Halbach VV, Ko NU, Lawton MT, Martin AJ, Quinnine NJ, Young WL: Estimation of fusiform intracranial aneurysm growth by serial magnetic resonance imaging. J Magn Reson Imaging 26:177-83, 2007.
PubMed abstract
2006
Pawlikowska L, Poon KYT, Achrol AS, McCulloch CE, Ha C, Lum K, Zaroff J, Ko NU, Johnston SC, Sidney S, Marchuk DA, Lawton MT, Kwok P-Y, Young WL: Apoliprotein E epsilon 2 is associated with new hemorrhage risk in brain arteriovenous malformation. Neurosurgery 58:838-43; discussion 838-43, 2006.
PubMed abstract
Chen Y, Fan Y-F, Yao JS, Poon KYT, Achrol AS, Lawton MT, Zhu Y, McCulloch CE, Hashimoto T, Lee C, Barbaro NM, Bollen AW, Yang G-Y, Young WL: MMP-9 expression is associated with leukocytic but not endothelial markers in brain arteriovenous malformations. Front Biosci 11:3121-8, 2006.
PubMed abstract
Acevedo-Bolton G, Jou LD, Dispensa BP, Lawton MT, Higashida RT, Martin AJ, Young WL, Saloner D: Estimating the hemodynamic impact of interventional treatments of aneurysms: numerical simulation with experimental validation: technical case report. Neurosurgery 59:E429-30; author reply E429-30, 2006.
PubMed abstract
Yarlaggada S, Rajendran P, Miss JC, Banki NM, Kopelnik A, Wu AHB, Ko NU, Gelb AW, Lawton MT, Smith WS, Young WL, Zaroff JG: Cardiovascular predictors of inpatient mortality after subarachnoid hemorrhage. Neurocrit Care 5:102-107, 2006.
PubMed abstract
Zhu Y, Lawton MT, Du R, Shwe Y, Shen F, Young WL, Yang G-Y: Expression of hypoxia-inducible factor-1 and vascular endothelial growth factor in response to venous hypertension. Neurosurgery 59:687-696, 2006.
PubMed abstract
Zhu Y, Shwe Y, Du R, Chen Y, Shen F, Young WL, Yang G-Y: Effects of angiopoietin-1 on the vascular endothelial growth factor-induced angiogenesis in the mouse brain Acta Neurochir Suppl 96:438-43, 2006.
PubMed abstract
Zaroff JG, Pawlikowska L, Miss, JC, Yarlagadda, S, Ha C, Achrol AS, Kwok P-Y, McCulloch CE, Lawton, MT, Ko NU, Smith WS, Young WL: Adrenoceptor polymorphisms and the risk of cardiac injury and dysfunction after subarachnoid hemorrhage. Stroke, 37:1680-1685, 2006.
PubMed abstract
Shen F, Su H, Liu W, Kan YW, Young WL, Yang G-Y: Recombinant adeno-associated viral vector encoding human VEGF165 induces neomicrovessel formation in the adult mouse brain. Front Biosci 11:3190-8, 2006.
PubMed abstract
Shen F, Su H, Fan Y, Chen Y, Zhu Y, Liu W, Young WL, Yang G-Y: Adeno-associated viral vector-mediated hypoxia-inducible vascular endothelial growth factor gene expression attenuates ischemic brain injury following focal cerebral ischemia in mice. Stroke 37:2601-6, 2006.
PubMed abstract
Sanchez-Mejia RO, Chenaputi S, Nalin G, Fullerton HJ, Young WL, Lawton MT: Superior outcomes in children versus adults after microsurgical resection of brain arteriovenous malformations. J Neurosurg 105:82-7, 2006.
PubMed abstract
Yao JS, Zhai W, Young WL, Yang GY. Related Articles, Links Interleukin-6 triggers human cerebral endothelial cells proliferation and migration: The role for KDR and MMP-9. Biochem Biophys Res Commun. 2006 Apr 21;342(4):1396-404.
PubMed abstract
Lee CZ, Yao JS, Huang Y, Zhai W, Liu W, Guglielmo BJ, Lin E, Yang GY, Young WL. Related Articles, Links Dose-response effect of tetracyclines on cerebral matrix metalloproteinase-9 after vascular endothelial growth factor hyperstimulation. J Cereb Blood Flow Metab. 2006 Jan 4;
PubMed abstract
Chen Y, Pawlikowska L, Yao JS, Shen F, Zhai W, Achrol AS, Lawton MT, Kwok PY, Yang GY, Young WL. Related Articles, Links Interleukin-6 involvement in brain arteriovenous malformations. Ann Neurol. 2006 Jan;59(1):72-80.
PubMed abstract
Achrol AS, Pawlikowska L, McCulloch CE, Poon KY, Ha C, Zaroff JG, Johnston SC, Lee C, Lawton MT, Sidney S, Marchuk DA, Kwok PY, Young WL; UCSF BAVM Study Project. Related Articles, Links Tumor necrosis factor-alpha-238G>A promoter polymorphism is associated with increased risk of new hemorrhage in the natural course of patients with brain arteriovenous malformations. Stroke. 2006 Jan;37(1):231-4.
PubMed abstract
2005
Pawlikowska L, Tran MN, Achrol AS, Ha C, Burchard E, Choudhry S, Zaroff J, Lawton MT, Castro R, McCulloch CE, Marchuk D, Kwok PY, Young WL; UCSF BAVM Study Project. Related Articles, Links Polymorphisms in transforming growth factor-beta-related genes ALK1 and ENG are associated with sporadic brain arteriovenous malformations. Stroke. 2005 Oct;36(10):2278-80.
PubMed abstract
Fullerton HJ, Achrol AS, Johnston SC, McCulloch CE, Higashida RT, Lawton MT, Sidney S, Young WL; UCSF BAVM Study Project. Related Articles, Links Long-term hemorrhage risk in children versus adults with brain arteriovenous malformations. Stroke. 2005 Oct;36(10):2099-104.
PubMed abstract
Zhu Y, Lee C, Shen F, Du R, Young WL, Yang GY. Related Articles, Links Angiopoietin-2 facilitates vascular endothelial growth factor-induced angiogenesis in the mature mouse brain. Stroke. 2005 Jul;36(7):1533-7.
PubMed abstract
Hashimoto T, Wu Y, Lawton MT, Yang GY, Barbaro NM, Young WL: Coexpression of angiogenic factors in brain arteriovenous malformations. Neurosurgery. 2005 May;56(5):1058-65; discussion 1058-65
PubMed abstract
Ko NU, Achrol AS, Chopra M, Saha M, Gupta D, Smith WS, Higashida RT, Young WL: Cerebral blood flow changes after endovascular treatment of cerebrovascular stenoses. Am J Neuroradiol. 2005 Mar;26(3):538-42
PubMed abstract
Lawton MT, Du R, Tran MN, Achrol AS, McCulloch CE, Johnston SC, Quinnine NJ, Young WL: Effect of presenting hemorrhage on outcome after microsurgical resection of brain arteriovenous malformations. Neurosurgery. 2005 Mar;56(3):485-93
PubMed abstract
Ko NU, Achrol AS, Martin AJ, Chopra M, Saloner DA, Higashida RT, Young WL: Magnetic resonance perfusion tracks 133Xe cerebral blood flow changes after carotid stenting. Stroke. 2005 Mar;36(3):676-8
PubMed abstract
Hashimoto T, Matsumoto MM, Li JF, Lawton MT, Young WL: Suppression of MMP-9 by doxycycline in brain arteriovenous malformations. BMC Neurol. 2005 Jan 24;5(1):1
PubMed abstract
2004
Chen Y, Xu B, Arderiu G, Hashimoto T, Young WL, Boudreau N, Yang GY: Retroviral delivery of homeobox D3 gene induces cerebral angiogenesis in mice. J Cereb Blood Flow Metab. 2004 Nov;24(11):1280-7
PubMed abstract
Young WL, Yang GY. Are there genetic influences on sporadic brain arteriovenous malformations? Stroke. 2004 Nov;35(11 Suppl 1):2740-5. Epub 2004 Oct 07
PubMed abstract
Pawlikowska L, Tran MN, Achrol AS, McCulloch CE, Ha C, Lind DL, Hashimoto T, Zaroff J, Lawton MT, Marchuk DA, Kwok PY, Young WL: UCSF BAVM Study Project. Polymorphisms in genes involved in inflammatory and angiogenic pathways and the risk of hemorrhagic presentation of brain arteriovenous malformations. Stroke. 2004 Oct;35(10):2294-300. Epub 2004 Aug 26
PubMed abstract
Hashimoto T, Wu Y, Boudreau N, Li J, Matsumoto M, Young W. : Regulation of Tie2 Expression by Angiopoietin-Potential Feedback System. Endothelium 2004;11(3-4):207-210
PubMed abstract
Yao JS, Chen Y, Zhai W, Xu K, Young WL, Yang GY. : Minocycle Exerts Multiple Inhibitory Effects on Vascular Endothelial Growth Factor-Induced Smooth Muscle Cell Migration. The Role of ERK1/2, PI3K, and Matrix Metalloproteinases. Circ Res. Jul 15
PubMed abstract
Lee CZ, Xu B, Hashimoto T, McCulloch CE, Yang GY, Young WL : Doxycycline suppresses cerebral matrix metalloproteinase-9 and angiogenesis induced by focal hyperstimulation of vascular endothelial growth factor in a mouse model. Stroke. 2004 Jul;35(7):1715-9. Epub 2004 May 27.
PubMed abstract
Halim AX, Johnston SC, Singh V, McCulloch CE, Bennett JP, Achrol AS, Sidney S, Young WL. : Longitudinal risk of intracranial hemorrhage in patients with arteriovenous malformation of the brain within a defined population. Stroke. 2004 Jul;35(7):1697-702.
PubMed abstract
Lawton MT, Stewart CL, Wulfstat AA, Derugin N, Hashimoto T, Young WL. : The transgenic arteriovenous fistula in the rat: an experimental model of gene therapy for brain arteriovenous malformations. Neurosurgery. 2004 Jun;54(6):1463-71; discussion 1471.
PubMed abstract
Kim EJ, Halim AX, Dowd CF, Lawton MT, Singh V, Bennett J, Young WL. : The relationship of coexisting extranidal aneurysms to intracranial hemorrhage in patients harboring brain arteriovenous malformations. Neurosurgery. 2004 Jun;54(6):1349-57; discussion 1357-8.
PubMed abstract
Lee CZ, Litt L, Hashimoto T, Young WL. : Physiologic monitoring and anesthesia considerations in acute ischemic stroke. J Vasc Interv Radiol. 2004 Jan;15(1 Pt 2):S13-9.
PubMed abstract
Yang GY, Yao JS, Huey M, Hashimoto T, Young WL: Participation of PI3K and ERK1/2 pathways are required for human brain vascular smooth muscle cell migration. Neurochem Int. 44(6):441-6, May 2004
PubMed abstract
Xu B, Wu YQ, Huey M, Arthur HM, Marchuk DA, Hashimoto T, Young WL, Yang GY: Vascular endothelial growth factor induces abnormal microvasculature in the endoglin heterozygous mouse brain. J Cereb Blood Flow Metab. 24(2): 237-244, February 2004
PubMed abstract
Hashimoto T, Lawton MT, Wen G, Yang GY, Chaly T JR, T, Stewart CL, Dressman HK, Barbaro NM, Marchuk DA, Young WL: Gene microarray analysis of human brain arteriovenous malformations. Neurosurgery 54(2): 410-425, February 2004
PubMed abstract
2003
Jou LD, Quick CM, Young WL, Lawton MT, Higashida R, Martin A, Saloner D. : Computational approach to quantifying hemodynamic forces in giant cerebral aneurysms. AJNR Am J Neuroradiol. 2003 Oct;24(9):1804-10.
PubMed abstract
Yang, GY, Xu B, Hashimoto T, Huey M, Chaly Jr T, Wen R, and Young WL. Induction of focal angiogenesis through adenoviral vector mediated vascular endothelial cell growth factor gene transfer in the mature mouse brain. Angiogenesis. 6(2): 151-158, 2003
PubMed abstract
Huang FP, Wang ZQ, Wu DC, Schielke GP, Sun Y, Yang GY.: Early NFkappaB activation is inhibited during focal cerebral ischemia in interleukin-1beta-converting enzyme deficient mice. J Neurosci Res. 1;73(5):698-707, 2003
PubMed abstract
Ko NU, Johnston SC, Young WL, Singh V, Klatsky AL: Distinguishing intracerebral hemorrhages caused by arteriovenous malformations. Cerebrovasc Dis 15:206-9, 2003
PubMed abstract
Lawton MT: Spetzler-Martin Grade III arteriovenous malformations: surgical results and a modification of the grading scale. Neurosurgery 52:740-8; discussion 748-9, 2003
PubMed abstract
Hashimoto T, Wen G, Lawton MT, Boudreau N, Bollen AW, Yang GY, Barbaro NM, Higashida RT, Dowd CF, Halbach VV, Young WL: Abnormal expression of matrix metalloproteinases and tissue inhibitors of metalloproteinases in brain arteriovenous malformations. Stroke 34:925-931, 2003
PubMed abstract
2002
Hashimoto T, Gupta DK, Young WL: Interventional neuroradiology--anesthetic considerations. Anesthesiol Clin North America, 20(2):347-59, vi, 2002
PubMed abstract
Quick CM, James DJ, Ning K, Joshi S, Halim AX, Hashimoto T, Young WL: Relationship of nidal vessel radius and wall thickness to brain arteriovenous malformation hemorrhage. Neurol Res, 24 (5):495-500, 2002
PubMed abstract
Hashimoto T, Young WL, Prohovnik I, Gupta DK, Ostapkovich ND, Ornstein E, Halim AX, Quick CM: Increased cerebral blood flow after brain arteriovenous malformation resection is substantially independent of changes in cardiac output. J Neurosurg Anesthesiol, 14 (3): 204-8, 2002
PubMed abstract
Halim AX, Young WL, Johnston SC: Reliability of angiographic assessment of brain arteriovenous malformations (editorial comment). Stroke 33 (6): 1508-9, 2002
PubMed abstract
Quick CM, Berger DS, Noordergraaf A: Pulse wave reflection as feedback in the arterial system. IEEE Trans. Biomed. Eng., 49: 440-445, 2002
PubMed abstract
Gupta DK, Young WL, Hashimoto T, Halim AX, Marshall RS, Lazar RM, Joshi S, Pile-Spellman J, Ostapkovich N: Characterization of the cerebral blood flow response to balloon deflation after temporary internal carotid artery test occlusion. J Neurosurg Anesthesiol, 14 (2):123-9, 2002
PubMed abstract
Halim AX, Singh V, Johnston SC, Higashida RT, Dowd CF, Halbach VV, Lawton MT, Gress DR, McCulloch CE, Young WL: Characteristics of brain arteriovenous malformations with coexisting aneurysms: a comparison of two referral centers. Stroke, 33 (3): 675-9, 2002
PubMed abstract
Young WL, Lawton MT, Gupta DK, Hashimoto T: Anesthetic management of deep hypothermic circulatory arrest for cerebral aneurysm clipping. Anesthesiology 96 (2): 497-503, 2002
PubMed abstract
Quick CM, Leonard EF, Young WL: Adaptation of the cerebral circulation to brain arteriovenous malformations increases feeding artery pressure and decreases regional hypotension. Neurosurgery 50: 167-175, 2002
PubMed abstract
2001
Hashimoto T, Young WL: Anesthesia-related considerations for cerebral arteriovenous malformations. Neurosurg Focus, 11 (5): Article 5, 2001
complete paper
Yang GY, Pang L, Ge HL, Tan M, Wu DC, Ye W, Huang FP, Liu XH, Che XM, Song Y, Wen R, Sun Y: Attenuation of ischemia-induced brain damage in mice by SAG, a redox inducible, antioxidant protein. J Cereb Blood Flow Metab. 2001:21: 722-733
PubMed abstract
Quick CM, Hashimoto T, Young WL: Lack of flow regulation may explain the development of arteriovenous malformations. Neurol Res 23: 641-644, 2001
PubMed abstract
Hashimoto T, Lam T, Boudreau NJ, Bollen AW, Lawton MT, Young WL: Abnormal balance in the angiopoietin-Tie2 system in human brain arteriovenous malformations. Circulation Research 89(2):111-3, 2001
PubMed abstract
Hashimoto T, Mesa-Tejada R, Quick CM, Bollen AW, Joshi S, Pile-Spellman J, Lawton MT, Young, WL: Evidence of increased endothelial cell turnover in brain arteriovenous malformations. Neurosurgery 49(1):124-132, 2001
PubMed abstract
Pang L, Ye W, Che XM, Roessler BJ, Betz AL, Yang GY: Reduction of inflammatory response in the mouse brain with adenoviral mediated transforming growth factor-beta 1 expression. Stroke 2001; 32: 544-555
PubMed abstract
Reporting terminology for brain arteriovenous malformation clinical and radiographic features for use in clinical trials. Stroke 32:1430-42, 2001
PubMed abstract
Ogilvy CS, Stieg PE, Awad I, Brown RD, Jr., Kondziolka D, Rosenwasser R, Young WL, Hademenos G: Recommendations for the management of intracranial arteriovenous malformations: a statement for healthcare professionals from a special writing group of the stroke council, american stroke association. Circulation 103:2644-57, 2001
PubMed abstract
Marshall RS, Lazar RM, Pile-Spellman J, Young WL, Duong DH, Joshi S, Ostapkovich N. Recovery of brain function during induced cerebral hypoperfusion. Brain Jun;124(Pt 6):1208-1217, 2001
PubMed abstract
Joshi S, Hashimoto T, Ostapkovich N, Pile-Spellman J, Duong DH, Hacien-Bey L, Marshall RS, James DJ, Young WL. Effect of intracarotid papaverine on human cerebral blood flow and vascular resistance during acute hemispheric arterial hypotension. Journal of Neurosurgical Anesthesiology. Apr;13(2):146-51, 2001
PubMed abstract
Quick CM, Berger DS, Noordergraaf A: Constructive and destructive addition of forward and reflected arterial pulse waves. American Journal of Physiology. Heart and Circulatory Physiology 280: H1519-H1527, 2001
PubMed abstract
Quick CM, Young WL, Noordergraaf A: Infinite solutions to the hemodynamic inverse problem. American Journal of Physiology. Heart and Circulatory Physiology 280(4):H1472-H1479, 2001
PubMed abstract
Choksi F, Weinsheimer S, Nelson J, Pawlikowska L, Fox CK, Zafar A, Mabray MC, Zabramski J, Akers A, Hart BL, Morrison L, McCulloch CE, Kim H. Assessing the association of common genetic variants in EPHB4 and RASA1 with phenotype severity in familial cerebral cavernous malformation. Mol Genet Genomic Med. 2021 Sep 07; e1794. PubMed
Fox CK, Nelson J, McCulloch CE, Weinsheimer S, Pawlikowska L, Hart B, Mabray M, Zafar A, Morrison L, Zabramski JM, Akers A, Kim H. Seizure Incidence Rates in Children and Adults With Familial Cerebral Cavernous Malformations. Neurology. 2021 Aug 13. PubMed
Hart BL, Mabray MC, Morrison L, Whitehead KJ, Kim H. Systemic and CNS manifestations of inherited cerebrovascular malformations. Clin Imaging. 2021 Jan 20; 75:55-66.
Girard R, Li Y, Stadnik A, Shenkar R, Hobson N, Romanos S, Srinath A, Moore T, Lightle R, Shkoukani A, Akers A, Carroll T, Christoforidis GA, Koenig JI, Lee C, Piedad K, Greenberg SM, Kim H, Flemming KD, Ji Y, Awad IA. A Roadmap for Developing Plasma Diagnostic and Prognostic Biomarkers of Cerebral Cavernous Angioma With Symptomatic Hemorrhage (CASH). Neurosurgery. 2021 Nov 18.
Choquet H, Pawlikowska L, Nelson J, McCulloch CE, Akers A, Baca B, Khan Y, Hart B, Morrison L, Kim H.Polymorphisms in inflammatory and immune response genes associated with cerebral cavernous malformation type 1 severity.Cerebrovas Dis. 2014 Dec 3;38(6):433-440. PubMed
Golden M, Saeidi S, Liem B, Marchand E, Morrison L, Hart B.Sensitivity of patients with familial cerebral cavernous malformations to therapeutic radiation.J Med Imaging Radiat Oncol. 2015 Feb;59(1):134-136. PubMed
Choquet H, Pawlikowska L, Lawton MT, Kim H.Genetics of cerebral cavernous malformations: current status and future prospects.J Neurosurg Sci. 2015 Sep;59(3):211-220. PubMed
Golden MJ, Morrison LA, Kim H, Hart BL.Increased number of white matter lesions in patients with familial cerebral cavernous malformations.AJNR Am J Neuroradiol. 2015 May;36(5):899-903. PubMed
Choquet H, Trapani E, Goitre L, Trabalzini L, Akers A, Fontanella M, Hart BL, Morrison LA, Pawlikowska L, Kim H, Retta SF.Cytochrome P450 and matrix metalloproteinase genetic modifiers of disease severity in Cerebral Cavernous Malformation type 1.Free Radic Biol Med. 2016 Mar;92:100-109. PubMed
Akers A, Al-Shahi Salman R, Awad IA, Dahlem K, Flemming K, Hart B, Kim H, Jusue-Torres I, Kondziolka D, Lee C, Morrison L, Rigamonti D, Rebeiz T, Tournier-Lasserve E, Waggoner D, Whitehead K.Synopsis of guidelines for the clinical management of cerebral cavernous malformations: Consensus recommendations based on systematic literature review by the Angioma Alliance Scientific Advisory Board Clinical Experts Panel.Neurosurgery. 2017 May 1;80(5):665-680. PubMed
Strickland CD, Eberhardt SC, Bartlett MR, Nelson J, Kim H, Morrison LA, Hart BL.Familial cerebral cavernous malformations are associated with adrenal calcifications on CT scans: an imaging biomarker for a hereditary cerebrovascular condition.Radiology. 2017 Aug;284(2):443-450. PubMed
Tang AT, Choi JP, Kotzin JJ, Yang Y, Hong CC, Hobson N, Girard R, Zeineddine HA, Lightle R, Moore T, Cao Y, Shenkar R, Chen M, Mericko P, Yang J, Li L, Tanes C, Kobuley D, Vosa U, Whitehead KJ, Li DY, Franke L, Hart B, Schwaninger M, Henao-Mejia J, Morrison L, Kim H, Awad IA, Zheng X, Kahn ML.Endothelial TLR4 and the microbiome drive cerebral cavernous malformations.Nature. 2017 May 18;545(7654):305-310. PubMed
Zou X, Hart BL, Mabray M, Bartlett MR, Bian W, Nelson J, Morrison LA, McCulloch CE, Hess CP, Lupo JM, Kim H.Automated algorithm for counting microbleeds in patients with familial cerebral cavernous malformations.Neuroradiology. 2017 Jul;59(7):685-690. PubMed
Morrison MA, Payabvash S, Chen Y, Avadiappan S, Shah M, Zou X, Hess CP, Lupo JM. A user-guided tool for semi-automated cerebral microbleed detection and volume segmentation: Evaluating vascular injury and data labelling for machine learning. Neuroimage Clin. 2018;20:498-505. PubMed
Zafar A, Quadri S, Farooqui M, Ikram A, Robinson M, Hart B, Mabray M, Vigil C, Tang A, Kahn M, Yonas H, Lawton M, Kim H, Morrison L: Familial Cerebral Cavernous Malformation (CCM). Stroke 2018. (in press)
Weinsheimer S, Nelson J, Abla AA, Ko NU, Tsang C, Okoye O, Zabramski JM, Akers A, Zafar A, Mabray MC, Hart BL, Morrison L, McCulloch CE, Kim H; Brain Vascular Malformation Consortium Cerebral Cavernous Malformation Investigator Group *. Intracranial Hemorrhage Rate and Lesion Burden in Patients With Familial Cerebral Cavernous Malformation. J Am Heart Assoc. 2023 Feb 7;12(3):e027572. doi: 10.1161/JAHA.122.027572. Epub 2023 Jan 25. PubMed
Kim SJW, Lupo JM, Chen Y, Pampaloni MH, VanBrocklin HF, Narvid J, Kim H, Seo Y. A feasibility study for quantitative assessment of cerebrovascular malformations using flutriciclamide ([(18)F]GE-180) PET/MRI. Front Med (Lausanne). 2023 Apr 5;10:1091463. doi: 10.3389/fmed.2023.1091463. eCollection 2023. PubMed
BVMC Project 2 – Publications on Sturge-Weber Syndrome since 2014
Lance EI, Lanier KE, Zabel TA, Comi AM. Stimulant use in patients with sturge-weber syndrome: safety and efficacy. Pediatr Neurol. 2014 Nov; 51(5):675-680. PubMed
Reidy TG, Suskauer SJ, Bachur CD, McCulloch CE, Comi AM. Preliminary reliability and validity of a battery for assessing functional skills in children with Sturge-Weber syndrome. Childs Nerv Syst. 2014 Dec; 30(12):2027-2036. PubMed
Comi A. Current therapeutic options in Sturge-Weber Syndrome. Semin Pediatr Neurol. 2015 Dec;22(4):295-301. PubMed
Comi AM, Sahin M, Hammill A, Kaplan EH, Juhasz C, North P, Ball KL, Levin AV, Cohen B, Morris J, Lo W, Roach ES, Sturge-Weber Syndrome Research W. Leveraging a Sturge-Weber Gene Discovery: An Agenda for Future Research. Pediatr Neurol. 2016 May;58:12-24. PubMed
Kaplan EH, Kossoff EH, Bachur CD, Gholston M, Hahn J, Widlus M, Comi AM. Anticonvulsant efficacy in Sturge-Weber syndrome. Pediatr Neurol. 2016 May;58:31-36. PubMed
Kavanaugh B, Sreenivasan A, Bachur C, Papazoglou A, Comi A, Zabel TA. Intellectual and adaptive functioning in Sturge-Weber Syndrome. Child Neuropsychol. 2016;22(6):635-648. PubMed
Dymerska M, Kirkorian AY, Offermann EA, Lin DD, Comi AM, Cohen BA. Size of Facial Port-Wine Birthmark May Predict Neurologic Outcome in Sturge-Weber Syndrome. J Pediatr. 2017 Sep;188:205-209 e201. PubMed PubMed
Offermann EA, Sreenivasan A, DeJong MR, Lin DDM, McCulloch CE, Chung MG, Comi AM, National Institute of Health S, Rare Disease Clinical Research C, Brain, Vascular Malformation C, National Sturge-Weber Syndrome W. Reliability and Clinical Correlation of Transcranial Doppler Ultrasound in Sturge-Weber Syndrome. Pediatr Neurol. 2017 Sep;74:15-23 e15. PubMed
De la Torre AJ, Luat AF, Juhász C, Ho ML, Argersinger DP, Cavuoto KM, Enriquez-Algeciras M, Tikkanen S, North P, Burkhart CN, Chugani HT, Ball KL, Pinto AL, Loeb JA. A Multidisciplinary Consensus for Clinical Care and Research Needs for Sturge-Weber Syndrome. Pediatr Neurol. 2018 Jul;84:11-20. Epub 2018 Apr 18. Review. PubMed
Wellman RJ, Cho SB, Singh P, Tune M, Pardo CA, Comi AM; BVMC Sturge–Weber syndrome Project Workgroup. Gαq and hyper-phosphorylated ERK expression in Sturge-Weber syndrome leptomeningeal blood vessel endothelial cells. Vasc Med. 2018 Aug 16. [Epub ahead of print] PubMed
Day AM, Hammill AM, Juhasz C, Pinto AL, Roach ES, McCulloch CE, Comi AM and collaborators. Pre-symptomatic treatment of Sturge-Weber Syndrome with Aspirin and Antiepileptic Drugs May Delay Seizure Onset. Pediatric Neurology, 2018 (In Press). PMC Journal – In Progress.
BVMC Project 3 – Publications on Hereditary Hemorrhagic Telangiectasia since 2014
Cheng KH, Mariampillai A, Lee K, Vuong B, Luk TW, Ramjist J, Curtis A, Jakubovic H, Kertes P, Letarte M, Faughnan ME, Yang VX. Histogram flow mapping with optical coherence tomography for in vivo skin angiography of hereditary hemorrhagic telangiectasia. J Biomed Opt. 2014 Aug; 19(8):086015. PubMed
Latino GA, Kim H, Nelson J, Pawlikowska L, Young W, Faughnan ME, Brain Vascular Malformation Consortium HHT Investigator Group. Severity score for hereditary hemorrhagic telangiectasia. Orphanet J Rare Dis. 2014 Dec 29;9:188. PubMed
Kim H, Nelson J, Krings T, terBrugge K, McCulloch CE, Lawton MT, Young WL, Faughnan ME, Brain Vascular Malformation Consortium HHT Investigator Group. Hemorrhage rates from brain arteriovenous malformation in patients with hereditary hemorrhagic telangiectasia. Stroke. 2015 May;46(5):1362-1364. PubMed
Krings T, Kim H, Power S, Nelson J, Faughnan M, Young WL, terBrugge KG, Brain Vascular Malformation Consortium HHT Investigator Group. Neurovascular manifestations in hereditary hemorrhagic telangiectasia: imaging features and genotype-phenotype correlations. AJNR Am J Neuroradiol. 2015 May;36(5):863-870. PubMed
Pawlikowska L, Nelson J, Guo DE, McCulloch CE, Lawton MT, Young WL, Kim H, Faughnan ME, Brain Vascular Malformation Consortium HHT Investigator Group. The ACVRL1 c.314-35A>G polymorphism is associated with organ vascular malformations in hereditary hemorrhagic telangiectasia patients with ENG mutations, but not in patients with ACVRL1 mutations. Am J Med Genet A. 2015 Jun;167(6):1262-1267. PubMed
Kasthuri RS, Montifar M, Nelson J, Kim H, Lawton MT, Faughnan ME, Brain Vascular Malformation Consortium HHT Investigator Group. Prevalence and predictors of anemia in hereditary hemorrhagic telangiectasia. Am J Hematol. 2017 Jun 22. (Epub ahead of print) PubMed
Meybodi AT, Kim H, Nelson J, Hetts SW, Krings T, terBrugge KG, Faughnan ME, Lawton MT, Brain Vascular Malformation Consortium HHT Group. Surgical Treatment vs Nonsurgical Treatment for Brain Arteriovenous Malformations in Patients with Hereditary Hemorrhagic Telangiectasia: A Retrospective Multicenter Consortium Study. Neurosurgery. 2018 Jan 1;82(1):35-47. PubMed
Klostranec JM, Chen L, Mathur S, McDonald J, Faughnan ME, Ratjen F, Krings T. A Theory for Polymicrogyria and Brain Arteriovenous Malformations in HHT. Neurol 2018. (in press). PMC Journal – In Progress.
Pawlikowska L, Nelson J, Guo D, McCulloch C, Lawton M, Kim H, Faughnan M, Group BVMCHI. Association of Common Candidate Variants with Vascular Malformations and Intracranial Hemorrhage in Hereditary Hemorrhagic Telangiectasia. MGGM. 2018 May PubMed
Quantification metrics for telangiectasia using optical coherence tomography. Sci Rep. 2022 02 02; 12(1):1805. Cardinell JL, Ramjist JM, Chen C, Shi W, Nguyen NQ, Yeretsian T, Choi M, Chen D, Clark DS, Curtis A, Kim H, Faughnan ME, Yang VXD, Brain Vascular Malformation Consortium HHT Investigator Group. PubMed
Neurovascular Complications and Pulmonary Arteriovenous Malformation Feeding Artery Size. Ann Am Thorac Soc. 2022 Apr 20. Ananiadis T, Faughnan ME, Clark D, Prabhudesai V, Kim H, Lawton MT, Vozoris NT, Brain Vascular Malformation Consortium HHT Investigator Group. PubMed
Kilian A, Latino GA, White AJ, Ratjen F, McDonald J, Whitehead KJ, Gossage JR, Krings T, Lawton MT, Kim H, Faughnan ME, The Brain Vascular Malformation Consortium Hht Investigator Group. Comparing Characteristics and Treatment of Brain Vascular Malformations in Children and Adults with HHT. J Clin Med. 2023 Apr 4;12(7):2704. PubMed
Cannavicci A, Zhang Q, Kutryk MJB. The Potential Role of MiRs-139-5p and -454-3p in Endoglin-Knockdown-Induced Angiogenic Dysfunction in HUVECs. Int J Mol Sci. 2023 Mar 3;24(5):4916. doi: 10.3390/ijms24054916. PubMed

The UCSF home departments of the CCR are Anesthesia and Perioperative Care, Neurological Surgery and Neurology, with allied and collaborating faculty in a number of basic science and clinical departments.
OUR MISSION STATEMENT
To advance and translate seminal metadisciplinary neuroscience, by combining insights and investigation across multiple perspectives and disciplines, with the common goal of providing effective, safe, and humane treatment of cerebrovascular diseases.
To provide the opportunity for students and faculty to pursue all levels of pre-doctoral, post-doctoral, and post-graduate training and intellectual development.
Principal Investigators
 Helen Kim, PhD
Helen Kim, PhD
Director, Clinical & Genetics Research
 Hua Su, MD
Hua Su, MD
Associate Director for Basic Science Research
 Mervyn Maze, MB, ChB
Mervyn Maze, MB, ChB
Principal Investigator
 Shantel Weinsheimer, PhD
Shantel Weinsheimer, PhD
Genetics of Brain AVMs
Collaborating Investigators
 Adib Abla, MD
Adib Abla, MD
Cerebrovascular Neurosurgery / Vascular Biology
 Rosemary Akurst, PhD
Rosemary Akurst, PhD
Vascular biology
 Tom Arnold, MD
Tom Arnold, MD
Pediatrics /Critical Care
 Aravind Asokan, PhD
Aravind Asokan, PhD
Synthetic Virology / Gene Therapy
 Krystof Bankiewicz, MD, PhD
Krystof Bankiewicz, MD, PhD
Gene Therapy / Translational Research
 Daniel Cooke, MD
Daniel Cooke, MD
Interventional Neuroradiology / Vascular diseases
 Zhonghui Guan, MD
Zhonghui Guan, MD
Acute Pain
 Tomoki Hashimoto, MD
Tomoki Hashimoto, MD
Vascular Biology / Clinical Anesthesiology
Barrow Neurological Institute Profile
 Akiko Hata, PhD
Akiko Hata, PhD
Molecular pathogenesis of pulmonary arterial hypertension
 Judith Hellman, MD
Judith Hellman, MD
Basic and translational research on sepsis
 Christopher Hess, MD, PhD
Christopher Hess, MD, PhD
Vascular Anomalies / Diffusion imaging, ultra-high field MRI
 Steven Hetts, MD
Steven Hetts, MD
Interventional Neuroradiology / Neurointerventional Surgery
 Nerissa Ko, MD
Nerissa Ko, MD
Neurovascular Service / Neurocritical Care Program
 Michael Lawton, MD
Michael Lawton, MD
Cerebrovascular Neurosurgery
Barrow Neurological Institute Profile
 Chanhung Lee, MD, PhD
Chanhung Lee, MD, PhD
Anesthesiologist / Endovascular treatment
 Jialing Liu, PhD
Jialing Liu, PhD
Neural regeneration and vascular remodeling
 Charles E. McCulloch, PhD
Charles E. McCulloch, PhD
Epidemiology / Biostatistics
 Paul S. Oh, PhD
Paul S. Oh, PhD
Molecular Biology / Vascular Biology
Barrow Neurological Institute Profile
 Jonathan Pan, MD, PhD
Jonathan Pan, MD, PhD
Spinal Cord Injury
 Tarik Tihan, MD, PhD
Tarik Tihan, MD, PhD
Molecular Pathology / Oncological Pathology
 Jonathan G. Zaroff, MD
Jonathan G. Zaroff, MD
Neurocardiac Injury / Transplant Genomics
Staff
 Phillip Evans
Phillip Evans
Research Analyst
 Lynn Ha
Lynn Ha
Research Admin
 Philippe Jolivalt
Philippe Jolivalt
Programmer
 Calvin Wang
Calvin Wang
Staff Research Associate
 Jeffrey Nelson
Jeffrey Nelson
Statistician
 Nhu Nuynh
Nhu Nuynh
Clinical Research Coordinator
 Eliel Rios Leon
Eliel Rios Leon
Clinical Research Coordinator
Trainees
 Alka Yadav, PhD
Alka Yadav, PhD
Postdoctoral fellow
 Zahra Shabani, PhD
Zahra Shabani, PhD
Postdoctoral fellow
 Ipsit Shah
Ipsit Shah
Visiting Graduate Student Researcher
Prior Faculty, Staff and Collaborators at the Center for Cerebrovascular Research whose involvement was at least one year. This list is provided solely as a professional courtesy. It implies no endorsement by any of the listed individuals of past, current or future activities of the CCR.
Contact Us

How to reach us:
UCSF Center for Cerebrovascular Research
UCSF Dept of Anesthesia Box 1363
1001 Potrero Ave
San Francisco, CA 94143
Phone: 628-206-8906
Fax: 628-206-8907
Email: [email protected]
Map: PDF Map of Zuckerberg San Francisco General (91 KB).

The Center for Cerebrovascular Research (CCR) is a core group of faculty and staff pursuing integrative and interdisciplinary studies of cerebrovascular disease, utilizing the tools of cell biology, in-vivo and in-vitro models, human genetics, epidemiology, and treatment outcomes research. Our main area of focus is vascular malformations of the brain, which are an important cause of hemorrhagic stroke, and include arteriovenous malformations (AVM), cerebral cavernous malformations (CCM). We have several National Institutes of Health (NIH)-funded clinical and basic science research studies involving collaborations with investigators across the country and internationally.
We are currently recruiting for the following positions:
Pilot Project Program
The NIH-funded Brain Vascular Malformation Consortium (BVMC, U54 NS065705) is soliciting proposals for a one-year pilot project proposal. Proposals should focus on the following rare diseases and/or related outcomes in cerebral cavernous malformation (CCM), Sturge Weber syndrome (SWS), or hereditary hemorrhagic telangiectasia (HHT). https://www.rarediseasesnetwork.org/cms/bvmc/About-Us
Instructions:
Applications must include the following:
• Two-page research description in standard NIH format (Specific Aims, Significance, Innovation, and Approach). All proposals should include one additional page outlining the timeline and significant milestones, with clear go/no go criteria.
• NIH Biosketch for key investigators involved in the project
• Budget and brief Justification
• Applications must be submitted to [email protected] no later than Friday, January 13, 2023.
Funding:
• Pilot projects proposals will be capped at $50,000.
• Proposals will be reviewed by the BVMC Executive Steering Committee and selected for funding based on the following criteria: clinical research potential in rare diseases, potential to enhance clinical trial readiness for any of the three BVMC diseases; thematic relationship to the aims and scope of the BVMC; scientific quality of the proposal; leverage existing BVMC (and RDCRN) resources and infrastructure, especially patient registries/databases; feasibility in projected time frame; ability to support promising junior investigators; ability to seed new collaborations that might lead to novel research concepts or therapeutic approaches; and ability to seed new collaborations that might lead to new grant proposals.
• Anticipated Start date is July 1, 2023.
Trainee/Clinical & Translational Investigator
The NIH-funded Brain Vascular Malformation Consortium (BVMC, U54 NS065705) is soliciting applications to support clinical/translational investigators who focus on the study of rare neurovascular diseases, including: cerebral cavernous malformation (CCM), Sturge Weber syndrome (SWS), or hereditary hemorrhagic telangiectasia (HHT). For more information about the BVMC, please visit: https://www.rarediseasesnetwork.org/cms/bvmc/About-Us
We are seeking to support advanced post-doctoral or clinical fellows, junior faculty, or established investigators who wish to develop or refocus their careers on clinical research in rare diseases. Under exceptional circumstances, we will consider applications from medical and graduate students proposing year-long projects. BVMC scholars should choose a mentor and research project aligned with one or more of the three BVMC Projects at cooperating institutions. There is wide breadth and depth of expertise spread across the BVMC that provides a rich research and mentoring environment.
Selected scholars will be expected to develop a detailed training plan with input from their mentor that is appropriate for their career stage and is expected to conduct the following:
(1) Design and implement a clinical research project related to one of the three main BVMC Projects
(2) With the aid of local or BVMC biostatistician, perform the data analysis for the research project
(3) Make a presentation describing the results in a local research seminar series, scientific conference, and to the BVMC Executive Committee
(4) Draft and submit a manuscript for publication describing the results of the research
(5) Draft a five-page outline of a proposal for future grant funding
INSTRUCTIONS:
Applicants should submit:
• Two-page letter of intent that briefly describes the candidate (areas of expertise, past training, and past and current research along with their role), primary mentor and mentorship record, trainee project, training plan (e.g., coursework, seminars, workshops, etc.), and how this support will further their careers.
• Curriculum vitae of applicant
• NIH biosketch of primary mentor
Budget and budget justification
• Applications must be submitted to [email protected] no later than Monday, February 13, 2023.
FUNDING:
• The total budget cannot exceed $55,000 per year. Typically, this is used to support trainee salary and fringe benefits with a minimum of three calendar months of effort devoted to training and the research project.
• However, if the full amount is not needed for salary and benefits, part or all of it can be used for research expenses (research personnel, supplies, etc.) for the trainee’s project. In such cases, a detailed budget and justification are required.
• Funding duration is for one year.
• Applications will be evaluated by the BVMC Executive Committee in five domains: (1) Track Record; (2) Research Plan; (3) Training Plan; (4) Resources; and (5) Career potential.
• Anticipated start date is July 1, 2023.
Assistant/Associate Specialist
The Center for Cerebrovascular Research in the Department of Anesthesia & Perioperative Care at the University of California, San Francisco, seeks an outstanding candidate for a position of Assistant/Associate Specialist. The Center established by the Departments of Anesthesia, studies a range of topics related to the cerebral circulation with special reference to cerebral vascular malformations and occlusive cerebrovascular diseases.
Required Qualifications:
- Specialists appointed at the Assistant rank must possess (or in process of obtaining) a master’s degree (or equivalent degree) or must have at least five years of experience in the relevant specialization.
- Specialists appointed at the Associate rank must possess (or in process of obtaining) a master’s degree (or equivalent degree) or must have at least five to ten years of experience in the relevant specialization.
- Applicant’s materials must list (pending) qualifications upon submission.
- Have previous experience in vascular biology with strong interest in neuroscience and vascular diseases.
- Be familiar with transgenic and knockout technologies.
- Have hands-on experience on cell culture, flow cytometry, qRT-PCR, ELISA and Western blot analysis.
- Have experience in management of a basic research laboratory.
- Able to work both independently and, in a team.
Preferred Qualifications:
- Knowledge of bioinformatics is desired.
UC San Francisco seeks candidates whose experience, teaching, research, or community service that
has prepared them to contribute to our commitment to diversity and excellence. The University of
California is an Equal Opportunity/Affirmative Action Employer. All qualified applicants will receive
consideration for employment without regard to race, color, religion, sex, sexual orientation, gender
identity, national origin, disability, age or protected veteran status.
Please apply online at https://aprecruit.ucsf.edu/JPF0
Postdoctoral Fellow in Cerebrovascular Biology
The Center for Cerebrovascular Research in the Department of Anesthesia & Perioperative Care at the University of California, San Francisco, seeks an outstanding candidate for a position of Postdoctoral Fellow. The Center established by the Departments of Anesthesia, studies a range of topics related to the cerebral circulation with special reference to cerebral vascular malformations and occlusive cerebrovascular diseases. There are allied and collaborating faculty in a number of neuroscience and vascular biology fields. The setting is ideal for a broad exposure to many aspects of cerebrovascular disease and pathophysiology.
Candidates should (1) have previous experience in vascular biology with strong interest in neuroscience and vascular diseases; (2) be familiar with transgenic and knockout technologies; (3) have hands-on experience on cell culture, flow cytometry, qRT-PCR, ELISA and Western blot analysis. Knowledge of bioinformatics is desired.
Applicants must possess a PhD, MD, or other doctoral level degree. It is essential that candidate has ability to work both independently, and in a team consisting of a diverse group of scientists with varying backgrounds and expertises.
Send curriculum vitae, names and contact information for three references, and a summary of research plan to:
Hua Su
Center for Cerebrovascular Research
Department of Anesthesia & Perioperative Care UCSF
PO BOX 1363
San Francisco, CA 94110
[email protected]
Postdoctoral Position
Opportunities for training and research are available in many areas, including vascular biology, mouse models of human disease, clinical and translational stroke research, epidemiology and biostatistics, bioinformatics and human genetics. The research environment is enhanced by strong national and international collaborative ties. Our group is highly interactive and multidisciplinary and includes physicians, geneticists, molecular biologists, and epidemiologists and biostatisticians. Candidates should have a strong background in neuroscience, statistical genetics or genetic epidemiology, and/or bioinformatics. Ability to work well with others, and strong communication and writing skills are required. Experience analyzing GWAS, sequencing, gene expression or other ‘omic’ datasets preferred.
Interested candidates should send email cover letter, curriculum vitae, and three letters of recommendation to: [email protected].
UCSF is an equal opportunity/affirmative action employer committed to excellence through diversity.
Updated: 11.30.2022
Ways to Give to the UCSF Center for Cerebrovascular Research
We thank you for considering a gift to cerebrovascular research at the UCSF Center for Cerebrovascular Research. The Center?s core mission is to improve our understanding of contemporary issues and problems in cerebrovascular disease using an integrative strategy that uses translational, interdisciplinary approaches to study the various diseases which cause stroke. The research provides a basis for more effective and safe treatment of cerebrovascular diseases.
Make a Gift Online
To make a donation through a secure online donation form, please click https://makeagift.ucsf.edu
Step 1) Click the "Direct your gift to a specific area" button

Step 2) Select "Center for Cerebrovascular Research" and click Continue
Step 3) Choose your donation amount and provide the request personal information and payment information.
Mail in Your Gift
Please make your check payable to UCSF Foundation* and mail it to:
UCSF Foundation
Box 45339
San Francisco, CA 94145
*Please note on your check "Center for Cerebrovascular Research"
Thank you for your choice to support research at the UCSF Center for Cerebrovascular Research!
The Center for Cerebrovascular Research wishes to express its gratitude to the following organizations for their generosity or support.








