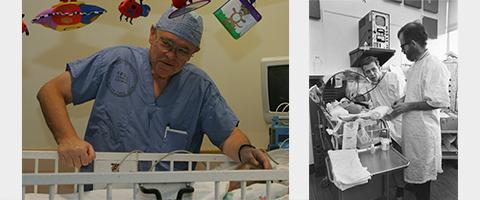
We are pleased to announce that Anesthesia Resident Stephanie Gilbert, MD, BS (Class of 2021), and UCSF School of Medicine student Tuyen Thanh Nguyen, MS-4, are the winners of the California Society of Anesthesiologists’ 2020 History of Anesthesia Essay Contest. Their essay (read below), describes Dr. George Gregory’s first use of CPAP for neonatal respiratory distress syndrome, how he developed this technique, and its profound impact on patient outcomes and medical practice.
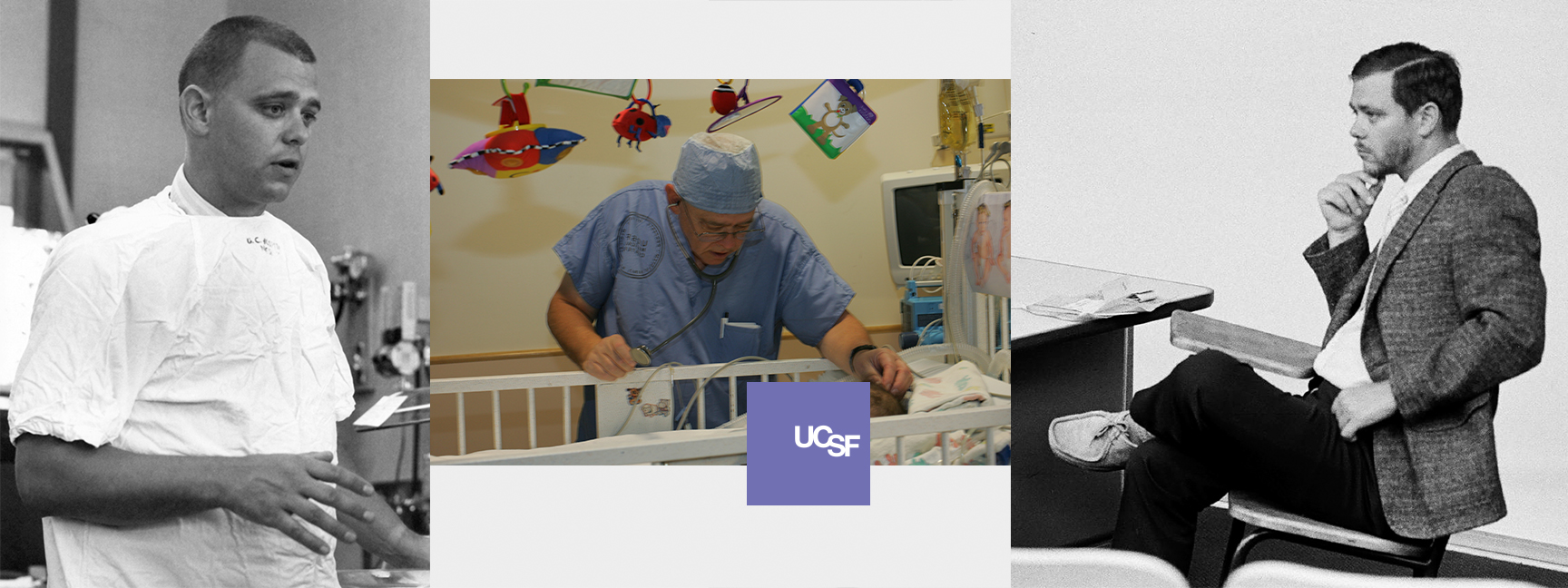
An interview with Dr. George Gregory
Stephanie Ranz Gilbert, MD, CA-2 | UCSF Anesthesia and Perioperative Care
Tuyen Thanh Nguyen, MS-4 | UCSF School of Medicine
Late one night in the Intensive Care Nursery, the anesthesiologist was called in to hand-ventilate another hypoxemic baby. This time, it was the child of a faculty member known to the anesthesiologist, and he was dismayed to receive the first blood gas with PaO2 30 mmHg. Since the baby was premature and the cardiology team had recommended catheterization, the anesthesiologist hand-ventilated the baby through the procedure, but he feared intubation was imminent. He thought back to his prior cases of neonatal respiratory distress syndrome (RDS) in premature infants, and felt frustrated as he thought: “This one will go just like the others. Intubation only leads to worsening hypoxemia and acidosis, and exposure to high inspired oxygen concentration can lead to an inflammatory response with morbid sequelae after only 5 minutes” (George Gregory, M.D., oral communication, February 2020). In fact, at that time, many of the babies treated conventionally for hyaline membrane disease– particularly the ones under 1 kilogram—had around 15% survival, recalled the anesthesiologist when retelling the story decades later. This was 1968 and a lack of understanding of neonatal pulmonary physiology often resulted in ineffective mechanical ventilation.1
As he ran through the management options for the deteriorating newborn, the young anesthesiologist thought of a recent paper which posited that many babies with hyaline membrane disease grunted as they breathed spontaneously in order to stent alveoli open at end expiration.2 Based on this information, he then wondered if the application of positive end-expiratory pressure (PEEP) would help keep his colleague’s child alive, and in a stroke of genius, he applied 8 of PEEP using an Ayres T-piece run under 8 cm of water. The Ayres T-piece was connected to fresh gas flow as well as a reservoir bag, and the system could be pressurized either by application of pressure to the bag, or by adjusting the flow rates. Holding his breath, he followed up with a blood gas and noted the PaO2 had risen to 80 mmHg, then to 230 mmHg over the next hour. He could hardly believe that he was actually able to lower the inspired oxygen!
This memorable night changed the course of Dr. George Gregory’s career, and with it, the history of pediatric anesthesia internationally. He began to study neonatal pulmonary compliance and resistance and measured functional residual capacity (FRC) with and without PEEP. He performed an initial study on neonates with respiratory distress syndrome and found that out of the first babies treated with nasal continuous positive airway pressure (CPAP), none had developed chronic lung disease, even to this day. The survival rate went from 15% in 1960 to 85% by 2000.1 In Dr. Gregory’s landmark NEJM publication in 1971, he presented two methods to apply CPAP: via an endotracheal tube as described above, and using a plastic pressure chamber without an endotracheal tube, making him the first to apply CPAP without an endotracheal tube.4 In the latter system, a plastic chamber surrounded the infant’s head and had openings for fresh gas inflow and for outflow of gas. The chamber itself could be squeezed manually to apply increased positive pressure.4
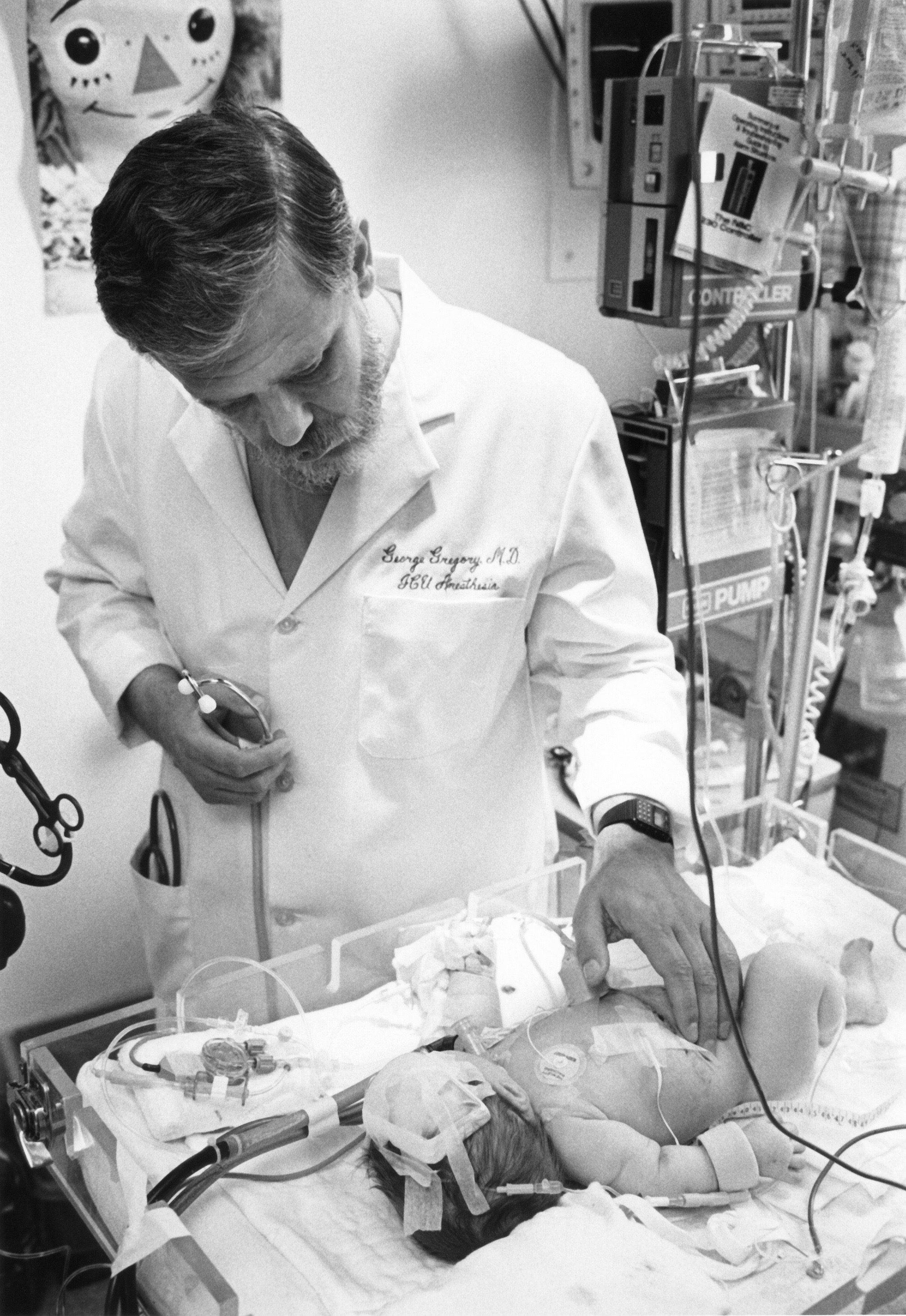 Years before Dr. Gregory discovered the use of the CPAP that would go on to save many lives, he was born in Denver, Colorado. At 8 years of age, when an abscess formed on his leg, the pain and its immediate alleviation once the abscess was lanced sparked a desire to learn about the field of medicine, and eventually led him to pursue a career in anesthesia.3 He attended UCLA for undergraduate studies and went on to receive his medical degree from UCSF School of Medicine. He remained at UCSF to complete his anesthesia residency (1965-1967) and fellowship at the Cardiovascular Research Institute (1967-1968). After fellowship, he was introduced to Dr. William Hamilton, who was then chair of anesthesia at UCSF. Based on his interest in neonatology and respiratory distress syndrome (RDS), Dr. Hamilton recommended Dr. Gregory for the role of intensive care nursery anesthesiologist, making him one of the first in this role nationally at that time.
Years before Dr. Gregory discovered the use of the CPAP that would go on to save many lives, he was born in Denver, Colorado. At 8 years of age, when an abscess formed on his leg, the pain and its immediate alleviation once the abscess was lanced sparked a desire to learn about the field of medicine, and eventually led him to pursue a career in anesthesia.3 He attended UCLA for undergraduate studies and went on to receive his medical degree from UCSF School of Medicine. He remained at UCSF to complete his anesthesia residency (1965-1967) and fellowship at the Cardiovascular Research Institute (1967-1968). After fellowship, he was introduced to Dr. William Hamilton, who was then chair of anesthesia at UCSF. Based on his interest in neonatology and respiratory distress syndrome (RDS), Dr. Hamilton recommended Dr. Gregory for the role of intensive care nursery anesthesiologist, making him one of the first in this role nationally at that time.
When Dr. Gregory first began work at UCSF in the 1960s, anesthesia and critical care, particularly in pediatrics, were in their infancy. Dr. Gregory recalled being taught to intubate infants by sticking his finger into the mouth and passing the endotracheal tube along the palpated epiglottis, looking for improvement in pulse rate and cyanosis to indicate successful intubation. This was before Dr. Severinghaus’ landmark contribution to the advent of pulse oximetry and arterial blood gas analysis.5 Ventilators for pediatric patients were very rudimentary, leading to pulmonary trauma and diffuse systemic complications, and contributing to the alarming mortality rates for infants with RDS when Dr. Gregory began his career.1
In addition to his life-saving contributions to the use of CPAP in neonates with RDS, Dr. Gregory is known for numerous subsequent contributions to the field of pediatric anesthesia, such as defining differing anesthetic requirements for children compared with adults. His landmark textbook—Gregory’s Pediatric Anesthesia—remains a cornerstone reference material for trainees in anesthesia and critical care. Today, he tirelessly continues to devote his time to training pediatric anesthesia residents, fellows, and attendings at UCSF as Professor Emeritus in Anesthesia and Pediatrics.
References
1. Philip, A. The Evolution of Neonatology. Pediatr Res 2005; 58: 799-815.
2. Harrison VC, Heese Hde V, Kline M. The significance of grunting in hyaline membrane disease. Pediatrics 1968; 41: 549-559.
3. Mai CL, Yaster M, Firth P. The development of continuous positive airway pressure: an interview with Dr. George Gregory. Pediatric Anesthesia. 2012;23(1):3-8. doi:10.1111/pan.12075
4. Gregory GA, Kitterman JA, Phibbs RH et al. Treatment of the idiopathic respiratory-distress syndrome with continuous positive airway pressure. N Engl J Med 1971; 284: 1333-1320.